
Office of the Inspector G eneral
U.S. Department of Justice
The Impact of an Aging Inmate
Population on the Federal Bureau of
Prisons
Revised February 2016
Evaluation and I nspections D
ivision 1
5-05 May 2 015

EXECUTIVE SUMMARY
Introduction
In September 2013, the Federal Bureau of Prisons (BOP) incarcerated
164,566 federal inmates in 119 BOP-managed institutions.
1
According to
BOP data, inmates age 50 and older were the fastest growing segment of its
inmate population, increasing 25 percent from 24,857 in fiscal year
(FY) 2009 to 30,962 in FY 2013.
2
By contrast, during the same period, the
population of inmates 49 and younger decreased approximately 1 percent,
including an even larger decrease of 16 percent in the youngest inmates (age
29 and younger).
3
Based on BOP cost data, we estimate that the BOP spent
approximately $881 million, or 19 percent of its total budget, to incarcerate
aging inmates in FY 2013.
4
The Office of the Inspector General (OIG)
conducted this review to assess the aging inmate population’s impact on the
BOP’s inmate management, including costs, health services, staffing,
housing, and programming. We also assessed the recidivism of inmates who
were age 50 and older at the time of their release.
Results in Brief
The OIG found that aging inmates are more costly to incarcerate than
their younger counterparts due to increased medical needs. We further
found that limited institution staff and inadequate staff training affect the
BOP’s ability to address the needs of aging inmates. The physical
infrastructure of BOP institutions also limits the availability of appropriate
housing for aging inmates. Further, the BOP does not provide programming
opportunities designed specifically to meet the needs of aging inmates. We
also determined that aging inmates engage in fewer misconduct incidents
while incarcerated and have a lower rate of re-arrest once released;
however, BOP policies limit the number of aging inmates who can be
considered for early release and, as a result, few are actually released early.
Aging inmates are more costly to incarcerate, primarily due to their
medical needs. We found that the BOP’s aging inmate population contributes
to increases in incarceration costs. Aging inmates on average cost 8 percent
1
For this review, we examined sentenced inmates incarcerated in BOP-managed
institutions only. We excluded approximately 29,000 inmates who are incarcerated in contract
institutions, as well as approximately 14,000 pre-trial inmates.
2
For the purposes of this review, we define inmates age 50 and older as “aging.” For
more information, see page 2.
3
The percentage decrease in the youngest inmates (age 29 and younger) was listed
incorrectly as 29 percent when this report originally was issued in May 2015. We discovered
the error and have revised the report to correct it.
4
For more information, see Appendix 1.
i
more per inmate to incarcerate than inmates age 49 and younger (younger
inmates). In FY 2013, the average aging inmate cost $24,538 to incarcerate,
whereas the average younger inmate cost $22,676. We found that this cost
differential is driven by increased medical needs, including the cost of
medication, for aging inmates. BOP institutions with the highest percentages
of aging inmates in their population spent five times more per inmate on
medical care ($10,114) than institutions with the lowest percentage of aging
inmates ($1,916). BOP institutions with the highest percentages of aging
inmates also spent 14 times more per inmate on medication ($684) than
institutions with the lowest percentage ($49).
BOP institutions lack appropriate staffing levels to address the needs of
an aging inmate population and provide limited training for this purpose.
Aging inmates often require assistance with activities of daily living, such as
dressing and moving around within the institution. However, institution staff
is not responsible for ensuring inmates can accomplish these activities. At
many institutions, healthy inmates work as companions to aging inmates;
but training and oversight of these inmate companions vary among
institutions. We further found that the increasing population of aging
inmates has resulted in a need for increased trips outside of institutions to
address their medical needs but that institutions lack Correctional Officers to
staff these trips and have limited medical staff within institutions. As a
result, aging inmates experience delays receiving medical care. For example,
using BOP data from one institution, we found that the average wait time for
inmates, including aging inmates, to be seen by an outside medical specialist
for cardiology, neurosurgery, pulmonology, and urology to be 114 days. In
addition, we found that while Social Workers are uniquely qualified to
address the release preparation needs of aging inmates, such as aftercare
planning and ensuring continuity of medical care, the BOP, which employs
over 39,000 people, has only 36 Social Workers nationwide for all of its
institutions. Institution staff told us they themselves did not receive enough
training to identify the signs of aging.
The physical infrastructure of BOP institutions cannot adequately
house aging inmates. Aging inmates often require lower bunks or
handicapped-accessible cells, but overcrowding throughout the BOP system
limits these types of living spaces. Aging inmates with limited mobility also
encounter difficulties navigating institutions without elevators and with
narrow sidewalks or uneven terrain. The BOP has not conducted a
nationwide review of the accessibility of its institutions since 1996.
The BOP does not provide programming opportunities specifically
addressing the needs of aging inmates. BOP programs, which often focus on
education and job skills, do not address the needs of aging inmates, many of
whom have already obtained an education or do not plan to seek further
employment after release. Though BOP institutions can and do design
programs, including release preparation programs, to meet the needs of their
ii
individual populations, even institutions with high percentages of aging
inmates rarely have programs specifically for aging inmates.
Aging inmates commit less misconduct while incarcerated and have a
lower rate of re-arrest once released. Aging inmates, comprising 19 percent
of the BOP’s inmate population in FY 2013, represented 10 percent of all the
inmate misconduct incidents in that year. Also, studies have concluded that
post-release arrests decrease as an individual ages, although BOP does not
maintain such data. The OIG conducted a sampling of data and found that
15 percent of aging inmates were re-arrested for a new crime within 3 years
of release. Based on our analysis, the rate of recidivism of aging inmates is
significantly lower than the 41 percent re-arrest rate that the BOP’s research
has found for all federal inmates. We further found that most of the aging
inmates who were re-arrested already had a documented history of
recidivism.
Aging inmates could be viable candidates for early release, resulting in
significant cost savings; but BOP policy strictly limits those who can be
considered and, as a result, few have been released. Over a year ago, the
Department concluded that aging inmates are generally less of a public
safety threat and the BOP announced an expanded compassionate release
policy to include them as part of the Attorney General’s “Smart on Crime”
initiative. However, the Department significantly limited the number of
inmates eligible for this expanded release policy by imposing several
eligibility requirements, including that inmates be at least age 65, and we
found that only two inmates had been released under this new provision.
According to institution staff, it is difficult for aging inmates to meet all of the
eligibility requirements of the BOP’s new provisions. Our analysis shows that
if the BOP reexamined these eligibility requirements its compassionate
release program could result in significant cost savings for the BOP, as well
as assist in managing the inmate population.
Recommendations
In this report, we make eight recommendations to improve the BOP’s
management of its aging inmate population. These recommendations
include enhancing BOP oversight and training of inmate companions,
studying the impact of the aging inmate population on infrastructure,
developing programs to address the needs of aging inmates during their
incarceration and as they prepare for release, and revising the requirements
that limit the availability of compassionate release for these inmates.
iii
TABLE OF CONTENTS
BACKGROUND ............................................................................................... 1
PURPOSE, SCOPE, AND METHODOLOGY............................................................ 9
RESULTS OF THE REVIEW ............................................................................. 10
Aging inmates are more costly to incarcerate, primarily due to their medical
needs..................................................................................................... 10
BOP institutions lack appropriate staffing levels to address the needs of an aging
inmate population and provide limited training for this purpose..................... 16
The physical infrastructure of BOP institutions cannot adequately house aging
inmates.................................................................................................. 23
The BOP does not provide programming opportunities specifically addressing the
needs of aging inmates ............................................................................ 30
Aging inmates commit less misconduct while incarcerated and have a lower rate
of re-arrest once released......................................................................... 37
Aging inmates could be viable candidates for early release, resulting in
significant cost savings; but new BOP policy strictly limits those who can be
considered and as a result, few have been released..................................... 41
CONCLUSION AND RECOMMENDATIONS......................................................... 51
APPENDIX 1: EXPANDED METHODOLOGY....................................................... 55
APPENDIX 2: THE BOP’S RESPONSE TO THE DRAFT REPORT ............................ 60
APPENDIX 3: OIG ANALYSIS OF THE BOP’S RESPONSE.................................... 63

BACKGROUND
Introduction
From fiscal year (FY) 2009 to FY 2013, the BOP experienced a shift in
the age demographic of its inmate population. During those 5 years, the
number of inmates age 50 and older in BOP-managed institutions was the
fastest growing segment of the BOP population, increasing by 25 percent,
from 24,857 to 30,962. During the same period, the population of inmates
49 and younger decreased approximately 1 percent, including an even larger
decrease of 16 percent in the youngest inmates age 29 and younger.
5
The OIG assessed the impact of an aging inmate population on the
BOP’s inmate management, including costs, health services, staffing,
housing, and programming, between FY 2009 and FY 2013. In this
background section, we define the BOP’s aging inmate population and discuss
the demographics and trends of this population. In addition, we outline the
new compassionate release provisions related to aging inmates. Finally, we
discuss the similar challenges faced by state correctional systems and the
different methods they use to address the growing aging inmate population.
Defining the BOP’s Aging Inmate Population
The BOP does not establish a specific age at which an inmate is
considered “aging.”
6
For the purposes of this report, we define inmates age
50 and older as aging.
7
Our definition is based on several factors including
studies, state programs and policies, as well as the opinions of BOP officials
and institution staff. In a 2004 report, the BOP’s National Institute of
Corrections (NIC) defined inmates age 50 and older as aging.
8
The NIC
further reported that seven state correctional agencies considered inmates
age 50 and older to be aging.
9
Several studies, including one published by
the American Journal of Public Health, state that an inmate’s physiological
5
The percentage decrease in the youngest inmates (age 29 and younger) was listed
incorrectly as 29 percent when this report originally was issued in May 2015. We discovered
the error and have revised the report to correct it.
6
When we asked BOP staff how they defined aging, their responses ranged from age
40 to age 78.
7
Throughout this report, we will use the term “aging inmates” to refer to inmates age
50 and older and the term “younger inmates” to refer to inmates age 49 and younger.
8
The NIC is an agency within the BOP. The NIC provides training, technical
assistance, information services, and policy and program development assistance to federal,
state, and local correctional agencies.
9
The NIC surveyed correctional systems in all 50 states, the District of Columbia,
U.S. territories, and Canada and found that seven states (Alaska, Florida, Idaho, New Mexico,
North Carolina, Ohio, and West Virginia) and Canada defined inmates as aging at age 50.
1

age averages 10–15 years older than his or her chronological age due to the
combination of stresses associated with incarceration and the conditions that
he or she may have been exposed to prior to incarceration.
10
During our
review, BOP officials and staff agreed that the combination of these factors
expedites the aging process. A Clinical Director told us that because most
aging inmates have preexisting conditions and are sicker than the general
population, they appear to be older than their actual age.
The BOP’s aging inmate population made up 19 percent of the BOP’s
overall population in FY 2013
Aging inmates made up 16 percent of the BOP’s total population in
FY 2009 and increased to 19 percent of the BOP’s total population in
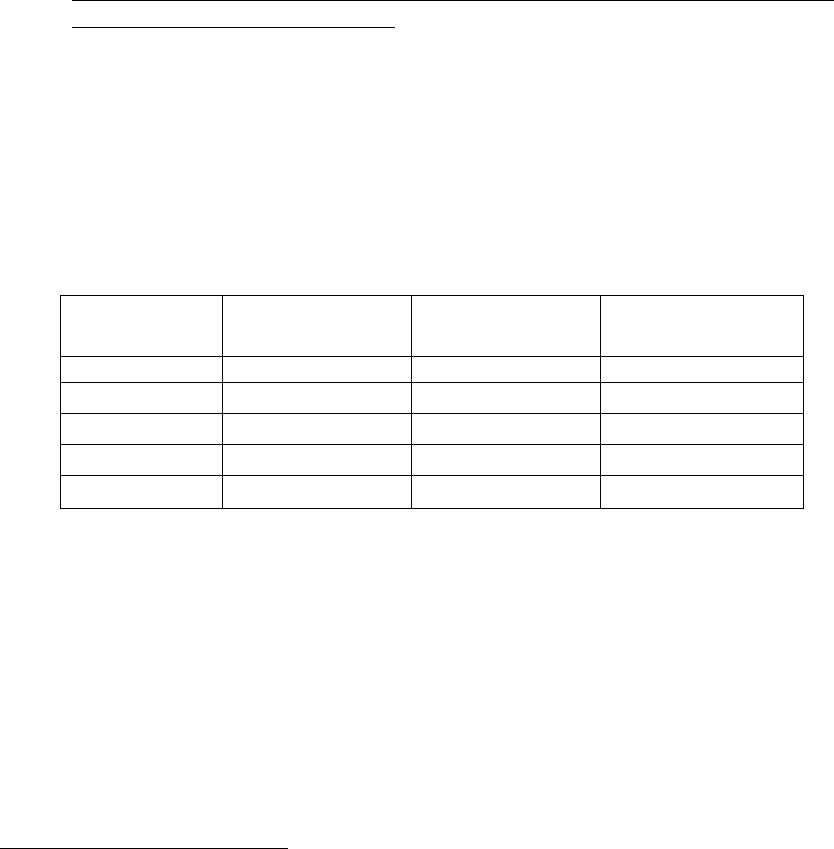
FY 2013. Table 1 presents the total number of sentenced BOP inmates, the
number of younger inmates, and the number of aging inmates from FY 2009
through FY 2013.
11
Table 1
Total Sentenced Inmate Population by Age
Fiscal Year
Sentenced
Inmates
Aging Inmates
(50 and older)
Younger Inmates
(49 and younger)
2009
159,189
24,857
134,332
2010 159,660 26,221 133,439
2011 165,797 28,239 137,558
2012 164,257 29,332 134,925
2013 164,566 30,962 133,604
Source: BOP population snapshots.
According to BOP data, not only are the numbers of aging inmates
increasing, they are generally increasing at a faster rate in older age groups.
Specifically, the number of inmates age 65 to 69 increased 41 percent;
inmates age 70 to 74 increased 51 percent; inmates age 75 to 79 increased
43 percent; and inmates age 80 and over increased 76 percent.
Nevertheless, inmates age 65 and older represented only 14 percent of the
aging inmate population in FY 2013, while inmates age 50 to 64 represented
86 percent of the 30,962 aging inmates. Figure 1 shows the increase in the
10
B. Williams, et al., “Aging in Correctional Custody: Setting a Policy Agenda for
Older Prisoner Health Care,” American Journal of Public Health 102, no. 8 (August 2012):
1475–1481, p. 3.
11
For this review, we examined sentenced inmates incarcerated in BOP-managed
institutions only. We excluded approximately 29,000 inmates who are incarcerated in contract
institutions, as well as approximately 14,000 pre-trial inmates.
2
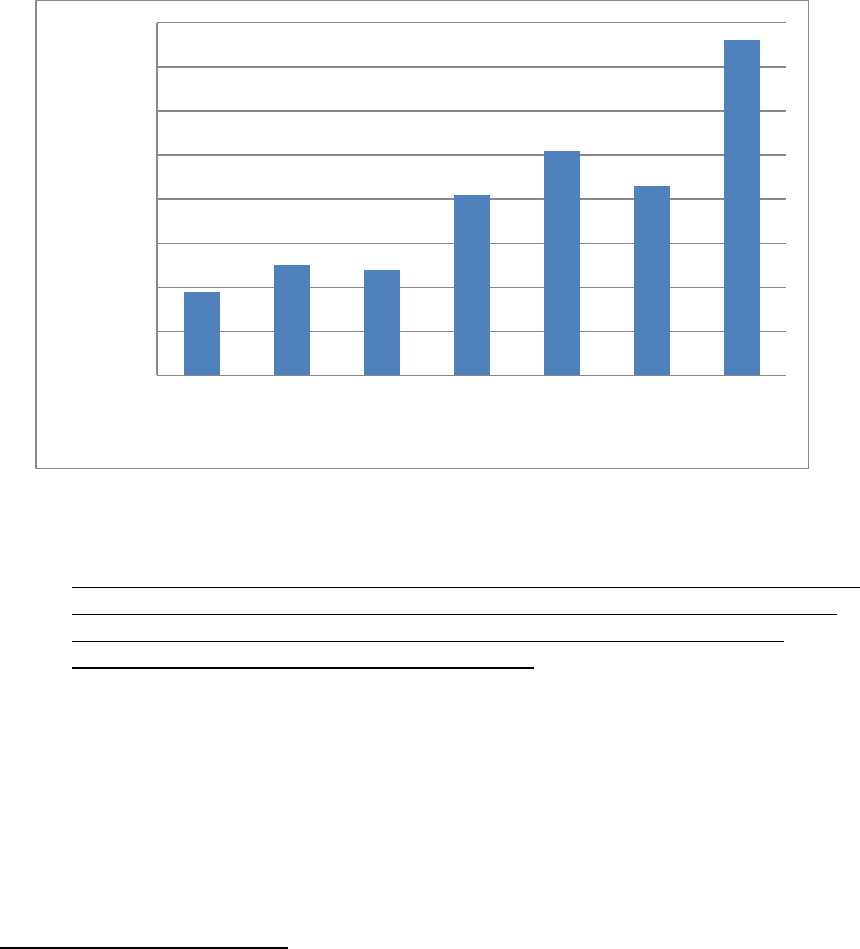
number of aging inmates, distributed in 5-year increments, from FY 2009
through FY 2013.
Figure 1
Percent Change in Population of Aging Inmates from FY 2009 to
FY 2013
Percent Change
0%
10%
20%
30%
40%
50%
60%
70%
80%
75-79 80+ 50-54 55-59 60-64 65-69 70-74
Age Cohorts
Source: BOP population snapshots.
Elimination of parole, use of mandatory minimum sentences, increases
in average sentence length over the past 3 decades, and an increase
in white collar offenders and sex offenders, among other things,
contribute to the aging inmate population
Research indicates that the growth in the aging inmate population can
be attributed to sentencing reforms beginning in the late 1980s, including the
elimination of federal parole and the introduction of mandatory minimums
and determinate sentences.
12
BOP staff and management officials agreed
that these sentencing reforms contributed to longer sentences, leading to an
increase in aging inmates. In addition to the increase in the aging inmate
population, there has also been a 9 percent increase in the number of
younger inmates who will be age 50 and older when they are ultimately
released.
13
(See Table 2 below.)
12
Nathan James, “The Federal Prison Population Buildup: Overview, Policy Changes,
Issues, and Options,” Congressional Research Service, April 15, 2014.
13
We based our analysis on each inmate’s release date as of the date we received
BOP data. We did not include younger inmates with life sentences, death sentences, or those
inmates who did not have release dates.
3

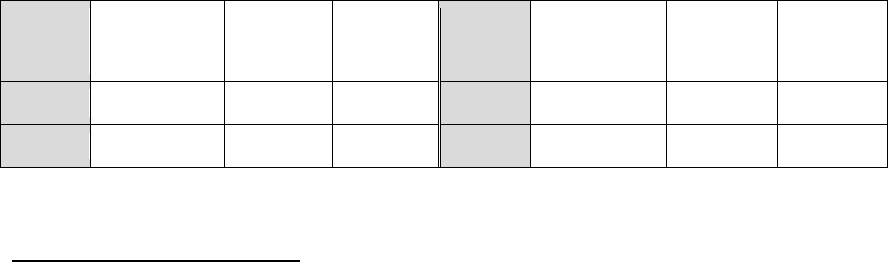
Table 2
Number of Younger Inmates Who Will Be Age 50 and Older at
Release
Fiscal Year
Number of Younger
Inmates
2009
19,385
2010
19,790
2011
20,488
2012
20,761
2013
21,221
Percent Change
9%
Source: BOP population snapshots.
The growth of the aging inmate population can also be attributed to
the increase in the number of aging offenders who are first-time white collar
or sex offenders.
14
From FY 2009 to FY 2013, the BOP experienced a
28 percent increase (7,944 to 10,153) in the number of first-time, aging
offenders. Further, the number of aging inmates incarcerated for fraud,
bribery, or extortion offenses increased by 43 percent and the number of
aging inmates incarcerated for sex offenses increased by 77 percent. White
collar offenders and sex offenders made up approximately 24 percent of the
aging inmate population in FY 2013. Conversely, these offenders made up
less than 10 percent of the younger inmate population.
Aging inmates make up a disproportionate share of the inmate
population in institutions providing higher levels of medical care
In 2002, the BOP implemented a system that assigned care levels to
inmates based on the inmate’s medical needs and to institutions based on
the resources available to provide care. Under this system, the BOP assigns
each inmate a care level from 1 to 4 based on documented medical history,
with Care Level 1 being the healthiest inmates and Care Level 4 being
inmates with the most significant medical conditions. The BOP also assigns
each institution a care level from 1 to 4, based on the institution’s level of
medical staffing and resources. Inmates are designated to an institution with
a corresponding care level.
15
(See Table 3 below.)
14
BOP data also indicated that 17,995 of the 30,962 (58 percent) aging inmates in
FY 2013 were sentenced at age 50 and older and 7,351 (41 percent) of those sentenced at 50
and older were first-time offenders.
15
For more information about the BOP’s care level system, see DOJ, OIG, The Federal
Bureau of Prisons’ Efforts to Manage Inmate Health Care.
4
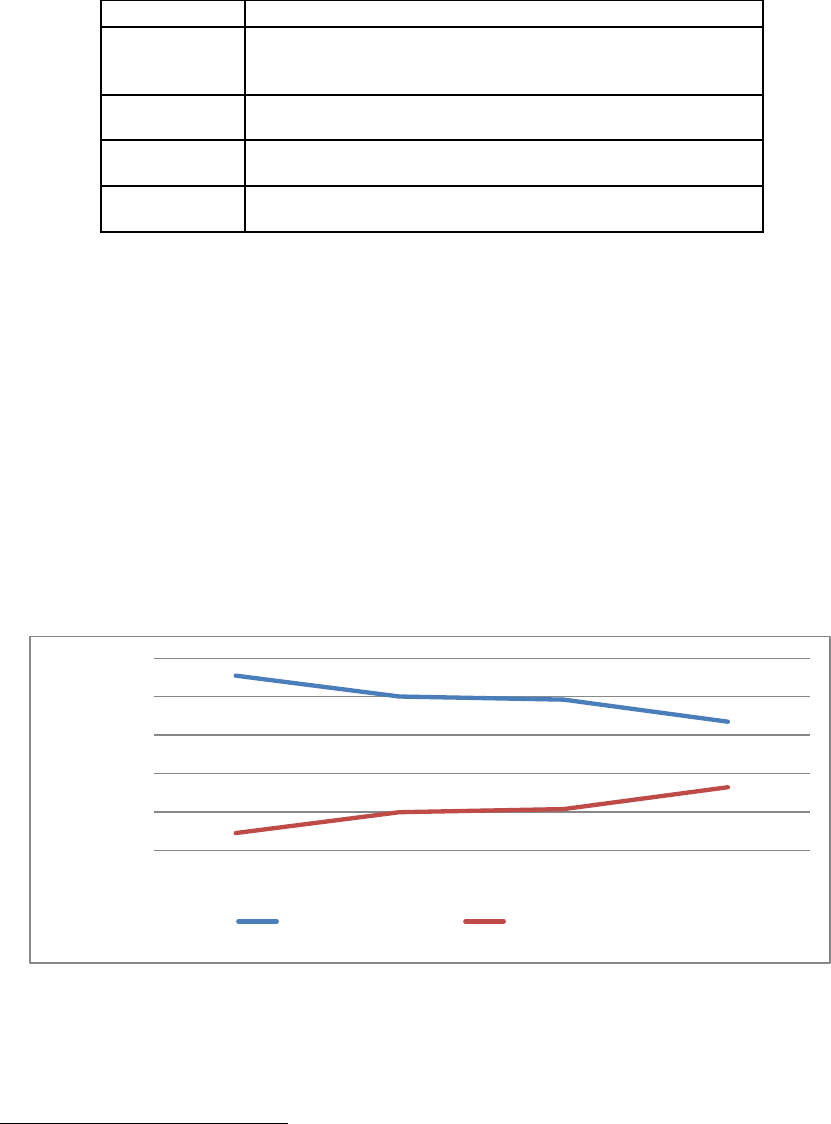
Table 3
Description of the BOP’s Care Levels
Care Level
Description
1
Inmates who are younger than 70, with limited
medical needs requiring clinical contact no more than
once every 6 months
2
Inmates who are stable outpatients, with chronic
illnesses requiring clinical contact every 3 months
3
Inmates who are fragile outpatients, with conditions
requiring daily to monthly clinical contact
4
Inmates requiring inpatient care: Care Level 4
institutions are BOP medical centers.
Source: U.S. Department of Justice (DOJ), OIG, The Federal Bureau of
Prisons’ Efforts to Manage Inmate Health Care, Audit Report 08-08
(February 2008).
According to BOP data, in FY 2013 aging inmates made up a
disproportionate share of the inmates housed in Care Level 3 and 4
institutions. Specifically, aging inmates made up 21 percent of the
population of Care Level 3 institutions and 33 percent of the population of
Care Level 4 institutions, compared to only 19 percent of the overall inmate
population.
16
Figure 2 illustrates the proportion of aging inmates assigned to
each care level.
Figure 2
Percentage of Aging Inmates Assigned to Each Care Level, FY 2013
100%
20%
40%
60%
80%
Percentage
0%
1 2 3 4
Care Level
Younger Inmates Aging Inmates
Source: BOP population snapshots.
16
Care Level 4 institutions also house cadre inmates who have work assignments and
are primarily made up of healthier, non–Care Level 4 inmates.
5

BOP Program Statement 5050.49 (Compassionate Release)
The increase of the aging inmate population adversely affects crowding
levels, particularly in minimum security, low security, and medical
institutions. At the end of FY 2013, the BOP as a whole was 34 percent over
capacity, with minimum security institutions at 19 percent over capacity, low
security institutions at 32 percent over capacity, and medical centers at
16 percent over capacity.
17
According to BOP data, aging inmates made up
26 percent of the population of minimum-security institutions, 23 percent of
the population of low-security institutions, and 33 percent of the population
of medical centers.
In the Sentencing Reform Act of 1984, Congress authorized the BOP
Director to request that a federal judge reduce an inmate’s sentence based
on “extraordinary and compelling” circumstances. Under the statute, the
request can be based on either medical or nonmedical conditions that could
not reasonably have been foreseen by the judge at the time of sentencing.
The BOP has issued regulations and a Program Statement entitled
“Compassionate Release” to implement this authority. In April 2013, the OIG
released a report that found significant problems with the management of
the BOP’s compassionate release program and that an effectively managed
program would help the BOP better manage its inmate population and result
in cost savings. We also found, in considering the impact of the
compassionate release program on public safety, a recidivism rate of
3.5 percent for inmates released through the program. By comparison, the
general recidivism rate for federal inmates has been estimated as high as
41 percent.
In August 2013, following the release of our review, the BOP
implemented new provisions to its Compassionate Release Program
Statement making inmates at least age 65 eligible for consideration for both
medical and nonmedical reasons.
18
One provision applies to inmates
sentenced for an offense that occurred on or after November 1, 1987, who
are age 70 years or older at the time of consideration for release and who
have served 30 years or more of their sentence of imprisonment. A second
provision applies to inmates:
17
Over-capacity level is based on our analysis of the BOP’s FY 2013 population
snapshot, combined with information about each institution’s security level as reported on the
BOP’s website. Our analysis excluded detention centers and contract institutions. The BOP’s
Long Range Capacity Plan, which includes all institutions, reports that at the end of FY 2013
the BOP as a whole was 36 percent overcrowded. At the end of FY 2014, the BOP reported
that its inmate population had dropped slightly from the year before. However, for this report
we examined population data only through FY 2013.
18
See BOP, Compassionate Release/Reduction in Sentence: Procedures for
Implementation of 18 U.S.C. § 3582(c)(1)(A) and 4205(g), Program Statement 5050.49
(August 12, 2013).
6

1. age 65 and older,
2. suffering from chronic or serious medical conditions related to the
aging process,
3. experiencing deteriorating mental or physical health that substantially
diminishes their ability to function in a correctional facility,
4. for whom conventional treatment promises no substantial
improvement to their mental or physical condition, and
5. who have served at least 50 percent of their sentence.
A third provision applies to inmates who are age 65 and older and
have served the greater of 10 years or 75 percent of their sentence. An
inmate’s medical condition is not evaluated under the first or third provisions.
To determine whether inmates applying under any of the three provisions are
suitable for compassionate release, the BOP further evaluates each inmate in
light of several factors, including but not limited to the nature and
circumstance of the inmate’s offense, criminal history, input from victims,
age at the time of offense and sentencing, release plans, and whether
release would minimize the severity of the offense.
States have begun addressing the challenges the of the aging inmate
population
State correctional systems are also facing an increase in aging inmate
populations. Specifically, according to a 2014 report, the number of inmates
age 55 and older in state and federal institutions increased 204 percent
between 1999 and 2012.
19
State correctional systems have also experienced
a substantial increase in healthcare costs. According to the report,
correctional healthcare spending rose in 41 states by a median of 13 percent
during the 5-year period from FY 2007 to FY 2011. The report indicates that
states generally incurred higher inmate healthcare spending where aging
inmates represented a larger proportion of the inmate population. For
example, the median healthcare spending per inmate in the 10 states with
the highest percentage of inmates age 55 and older averaged $7,142, while
the 10 states with the lowest percentage of these inmates averaged $5,196
per inmate. Later in this report, we provide a similar analysis based on BOP
institutions with the highest and lowest percentage of aging inmates.
To address the growth of aging inmate populations, at least 15 states
have provisions that would allow for the consideration of early release for
19
Pew Charitable Trusts and the John D. and Catherine T. MacArthur Foundation,
“State Prison Health Care Spending,” July 8, 2014, http://www.pewtrusts.org/en/research-
and-analysis/reports/2014/07/08/state-prison-health-care-spending (accessed April 9, 2015).
The report did not break out the increase between state and federal institutions.
7

aging inmates, but with varying eligibility requirements.
20
Some states
restrict eligibility to aging inmates with physically or mentally debilitating
conditions, while other states open eligibility to all aging inmates who meet
age and time served requirements. Outside of early release considerations,
several states have developed separate housing units or institutions for aging
inmates, including housing units dedicated to older inmates with chronic
health problems. For example, the Florida Department of Corrections has
several institutions with units designed specifically for aging inmates,
including one dedicated for inmates age 50 and older. States have also
recognized the need for different programming for aging inmates, including
one program in Nevada designed for inmates age 55 and older to enhance
their overall health through daily activities.
20
Tina Chiu, “It’s About Time: Aging Prisoners, Increasing Costs, and Geriatric
Release,” VERA Institute of Justice, April 2010.
8

PURPOSE, SCOPE, AND METHODOLOGY
Purpose
Our review examined the BOP’s aging inmate population by assessing
the population’s impact on incarceration costs, health services, staffing,
housing, and programming. We also determined the recidivism rate of aging
inmates released from BOP custody.
Scope and Methodology
Our review analyzed BOP inmate population and cost data, as well as
BOP policies and programs from FY 2009 through FY 2013. Our review
focused on federal offenders incarcerated in the 119 institutions operated by
the BOP during our scope years. We excluded inmates housed in private
correctional institutions, contract community corrections centers, and
contract state and local institutions from our analysis. We also excluded
inmates who were in pre-trial detention.
Our fieldwork, conducted from February 2014 through
September 2014, included interviews, data collection and analyses, and
document reviews. We interviewed BOP officials, including the Assistant
Directors responsible for eight Central Office divisions.
21
We conducted
13 site visits to BOP institutions, including 5 institutions through video
teleconferences and 8 institutions in person. For each site visit, we
interviewed institution officials and staff. For those institutions that we
visited in person, we also interviewed inmates, toured housing units, and
observed the physical landscapes. Our site visits encompassed
BOP institutions representing all security levels, including minimum-, low-,
medium-, and high-security institutions, as well as administrative security
institutions such as federal medical centers and detention centers. A detailed
description of the methodology of our review is in Appendix 1.
21
The BOP’s Central Office is located in Washington, D.C. We interviewed the
Assistant Directors of the Administration; Human Resource Management; Health Services;
Information, Policy, and Public Affairs; Reentry Services; Correctional Programs; and
Industries, Education and Vocational Training Divisions. We also interviewed the General
Counsel.
9

RESULTS OF THE REVIEW
Aging inmates are more costly to incarcerate, primarily due to their
medical needs
According to BOP officials and staff, an aging inmate population’s most
significant impact is on medical costs. From fiscal year (FY) 2009 to
FY 2013, the BOP’s spending on inmate healthcare increased by 29 percent,
according to BOP data. In FY 2009, the BOP spent $854 million of its
$5.5 billion budget (16 percent) to provide medical care for its inmate
population. By FY 2013, medical costs increased to $1.1 billion, representing
17 percent of the BOP’s $6.5 billion budget that year. While the BOP states
that it cannot determine the specific medical costs associated with individual
inmates, we found that aging inmates, as a group, are more expensive to
incarcerate than younger inmates, primarily due to their medical needs. We
also found that medical costs are increasing at a rate higher than the BOP’s
total budget, especially at institutions housing more aging inmates, and are
driven by medications and medical trips outside of institutions. Finally, we
found aging inmates are receiving more medical services, both within BOP
institutions and from outside healthcare providers.
Using BOP inmate population and cost data, we estimated costs per
inmate based on security level and the number of days incarcerated within a
fiscal year.
22
We found that an aging inmate, on average, costs 8 percent
more to incarcerate than a younger inmate. For example, in FY 2013, the
average aging inmate cost $24,538 to incarcerate, whereas the average
younger inmate cost $22,676. We also found that average cost per inmate
rises with age, with the 8,831 inmates age 18 to 24 costing an average of
$18,505 each and the 157 inmates age 80 and older costing an average of
$30,609 each. While the aging inmate population represents only 19 percent
of the BOP’s total population, the costs to incarcerate them are increasing at
a faster rate than for younger inmates. For example, the cost of
incarcerating aging inmates grew 23 percent, from $715 million in FY 2010 to
$881 million in FY 2013, while the cost of incarcerating younger inmates
grew 3 percent, from $3.5 billion to $3.6 billion over the same period. (See
Figure 3 below for the average annual cost per inmate in FY 2013.)
22
The BOP determines the average cost to incarcerate inmates by the type of
institution where an inmate is housed, such as a low-security institution or a federal medical
center, not by the specific cost to incarcerate each inmate. Therefore, we calculated the
number of days served by each inmate in each fiscal year and applied the cost of the type of
institution where that inmate was housed. See Appendix 1 for more details on our analysis.
10
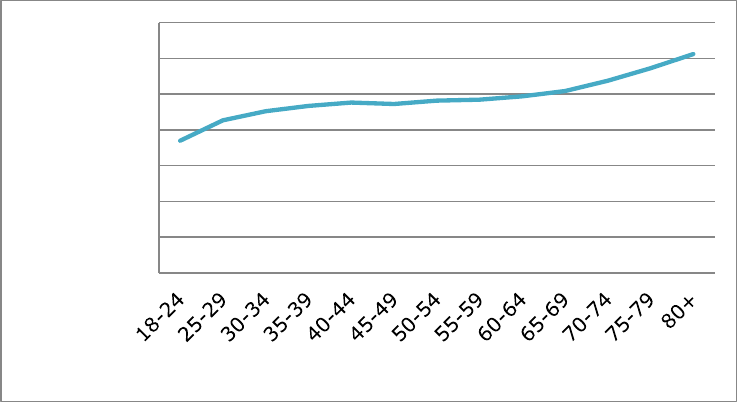
Figure 3
Av
erage Annual Cost per Inmate by Age, FY 2013
Average Cost
$35,000
$30,000
$25,000
$20,000
$15,000
$10,000
$5,000
$0
Age
Source: BOP population and daily cost data.
According to the BOP’s Assistant Director for Health Services and
Medical Director, inmates in their fifties and sixties place the greatest burden
on the BOP because their numbers are increasing and many of them have
significant health problems stemming from years of substance abuse.
Similarly, BOP officials and staff at each institution we visited said the most
significant impact of aging inmates on the BOP is the cost associated with
addressing their increased medical needs. For example, a Health Services
Administrator of an institution where aging inmates were 27 percent of the
population told us that her institution’s medical budget increased from
$3 million to $9 million in FY 2012 alone due to the aging inmate population.
Aging inmates we interviewed also acknowledged their impact on the BOP’s
medical costs. One aging inmate told us that he has had two heart attacks,
two strokes, open-heart surgery, cancer, and has diabetes. He told us that it
must cost the BOP “a fortune” to keep him incarcerated. We discuss the
impact aging inmates have on BOP institutions’ medical costs, as well as
factors that drive increased medical costs for aging inmates, below.
11
Healthcare spending per inmate is greater at institutions with the highest
percentage of aging inmates
Using BOP population and medical cost data, we calculated medical
spending per inmate within each institution and found that the BOP’s
healthcare spending coincides with the percentage of aging inmates at an
institution.
23
Specifically, we found that the five institutions with the highest
percentage of aging inmates spend significantly more per inmate on medical
costs than the five institutions with the lowest percentage of aging inmates
(see Table 4).
24
Table 4
Medical Spending per Inmate at Institutions with the Five Highest
and Lowest Percentages of Aging Inmates
FY 2009
Percentage
of Aging
Inmates
Cost Per
Inmate
FY 2013
Percentage
of Aging
Inmates
Cost Per
Inmate
Highest
27%
$6,528
Highest
31%
$10,114
Lowest
5%
$2,110
Lowest
7%
$1,916
Source: BOP medical spending data.
As Table 4 shows, in FY 2009, institutions with the highest percentage
of aging inmates spent on average $6,528 per inmate on medical costs while
institutions with the lowest percentage of aging inmates averaged $2,110 per
inmate. The same pattern of spending emerged in FY 2013, when
institutions with the highest percentage of aging inmates spent on average
$10,114 per inmate while institutions with the lowest percentage of aging
inmates spent $1,916 per inmate.
23
According to the BOP, there is no direct way to associate medical care provided
with the costs incurred for each inmate because its electronic medical records system and
financial management system are not connected. The BOP’s Assistant Director for
Administration told us that the BOP does not track costs by inmate because its accounting
system tracks spending by program area only.
24
We excluded BOP medical centers, detention centers, and correctional complexes
from this analysis. We excluded correctional complexes because spending data is reported in
the aggregate instead of separately for each institution within the complex. For example, one
correctional complex spent $99 million on medical care in FY 2013 but we could not determine
how much was specifically spent by a medical center and each of three other institutions
within the complex. Because we excluded these institution types, our cost estimates of
spending per inmate are lower. See Appendix 1 for additional details.
12

Institutions with the highest percentage of aging inmates spend more per
inmate on medical care provided both inside and outside BOP institutions
All BOP institutions operate ambulatory clinics that incur medical
expenses for inmate care provided inside the institution. If an inmate has a
medical condition that becomes emergent, escalates, or requires further
examination or diagnosis from a specialist, the inmate may be transported
outside the institution for services. We found that medical costs incurred for
care provided both inside and outside institutions account for 86 percent of
the BOP’s medical costs each year.
25
According to the BOP, costs for medical
services provided inside all BOP institutions increased 19 percent, from
$413 million in FY 2009 to $493 million in FY 2013. Costs for medical
services provided outside BOP institutions (often in private or public
hospitals) increased even more sharply, rising 31 percent, from $320 million
in FY 2009 to $420 million in FY 2013.
We also found that costs for medical services provided both inside and
outside institutions increased at a higher rate at institutions with the highest
percentage of aging inmates when compared to institutions with the lowest
percentage of aging inmates. For example, in FY 2009, institutions with the
highest percentage of aging inmates spent about four times as much on
medical care provided outside of institutions than those with the lowest
percentage of aging inmates. By FY 2013, the gap widened even more
significantly, with institutions with the highest percentage of aging inmates
spending on average over 10 times more on outside medical care than
institutions with the lowest percentage of aging inmates. (See Table 5
below.)
Table 5
Average Cost Per Inmate for Medical Services Provided Inside and
Outside Institutions with the Highest and Lowest Percentages of
Aging Inmates
FY
2009
Percentage
of Aging
Inmates
Inside
Services
Outside
Services
FY
2013
Percentage
of Aging
Inmates
Inside
Services
Outside
Services
Highest 27% $2,551 $2,826 Highest 31% $3,436 $5,751
Lowest
5%
$1,244
$658
Lowest
7%
$1,224
$563
Source: BOP medical spending data.
25
Medical costs also include salaries for U.S. Public Health Service employees, who
staff many institution medical clinics; medical transport costs; and costs of handling
unforeseen medical events at institutions. These costs, when combined with inside and
outside medical services, total the BOP’s medical budget. See Appendix 1 for additional
details.
13

Institution staff also
told us that aging inmates
incur more medical costs
due to increased visits to
medical clinics inside the
institution and medical trips
outside the institution. For
example, a Warden told us
that aging inmates are more
likely to be chronic care
patients seen more
frequently by healthcare
services.
26
Aging inmates
also told us they are
receiving more medical
services. For example, a
different aging inmate from
the one referenced above
told us he gets two shots
per day, requires dialysis,
and has a number of ailments including congestive heart failure, diabetes,
sleep apnea, cataracts, and Hepatitis C. In addition to medical care provided
inside the institution to treat his medical conditions, every 6 months he
receives outside medical care for his heart. Below, we discuss two specific
factors that we found drive increased medical costs associated with an aging
inmate population: medication costs and staff overtime to meet inmate
medical needs.
Budgetary Impact of Hepatitis C Treatment
According to the BOP, as medication costs continue
to increase, they will place even greater pressure on
the BOP’s budget in the future. For example,
institution staff told us about treatments recently
approved by the Food and Drug Administration (FDA)
regarding Hepatitis C, a condition that is particularly
prevalent among aging inmates. Approximately
12,000 inmates have Hepatitis C, and 47 percent of
those are aging inmates. Medical staff at a BOP
medical center told us that while they did not yet
know the cost of the new Hepatitis C medication at
the time of our interview, they anticipated costs to be
“astronomical” because Hepatitis C is one of the most
common infectious diseases in the inmate population.
The BOP reports that former treatments cost $6,600
per patient, while the treatment recently approved by
the FDA will cost an additional $20,000 to $40,000
per patient.
Source: BOP FY 2015 congressional budget
justification.
14
Me
dications and staff overtime to meet inmate medical needs are significant
drivers of increasing medical costs
Due to their medical needs and chronic health problems, aging
inmates require more medications and are substantially driving up the BOP’s
medical costs. We found that the BOP’s spending on medications increased
32 percent, from $62 million in FY 2009 to $82 million in FY 2013. We also
found that the BOP’s spending on medications was higher, and increased
faster, at institutions with the highest percentage of aging inmates. The
BOP’s Assistant Director for Health Services and Medical Director told us that
medication for inmates requiring chronic care is one of the BOP’s major
healthcare cost drivers. A Warden also said that a high percentage of aging
inmates are being treated for chronic medical conditions and that
medications drive the costs to care for these inmates. By contrast,
medication costs were lower and increased more slowly at institutions with
26
The BOP schedules inmates with ongoing medical problems for frequent
appointments with BOP medical staff to reassess their status and renew their prescriptions.

the lowest percentage of aging inmates. For example, in FY 2013 institutions
with the highest percentage of aging inmates spent an average of $684 per
inmate on medications, or about 14 times more than those with the lowest
percentage of aging inmates, which spent an average of $49 per inmate on
medications in FY 2013.
Institution staff also told us that aging inmates with chronic conditions
require treatment from specialists outside the institution and that overtime
paid to Correctional Officers who escort inmates to such appointments is a
significant budget item. According to BOP data, in FY 2013, in addition to
paying for outside medical care, the BOP spent $53 million in overtime to
transport inmates to outside medical care, a 17 percent increase from the
$46 million spent in FY 2009. As one example, an Associate Warden said
overtime costs associated with transporting aging inmates to outside medical
appointments and hospitalizations were “phenomenal” and that his institution
was over its allotted overtime budget less than half way through the fiscal
year for this reason.
Aging inmates disproportionately require catastrophic medical care
In May 2012, the BOP Assistant Director for Health Services and
Medical Director issued to all institutions a memorandum on “Catastrophic
Case Management”; it defined catastrophic medical cases as those where the
estimated or actual cost of outside medical care for an inmate housed in a
nonmedical BOP institution exceeds $35,000 for a single medical event and
provided guidance on how to track and monitor these cases.
27
We analyzed
catastrophic care data from one BOP region between FY 2009 and FY 2013
and found that while only 18 percent of the inmates in this region were aging
inmates during this period, 59 percent of the catastrophic medical cases
involved aging inmates (see Table 6). Moreover, because the aging inmate
population in this region was about four times smaller than the younger
inmate population, the probability of an aging inmate having a catastrophic
medical issue was about eight times higher than for a younger inmate.
27
As of FY 2012, all BOP regions adopted a catastrophic case management system
designed to track and monitor cases and to measure the fiscal and clinical outcomes of care.
While beyond the scope of this review, we learned that the BOP’s six regions do not
consistently track catastrophic medical cases and that the BOP’s Central Office does not
process or analyze that data to better understand the impact of catastrophic healthcare events
on budget and decision-making. Due to the inconsistency of regional tracking, we were able
to analyze catastrophic case spending in only one region. See Appendix 1 for details.
15
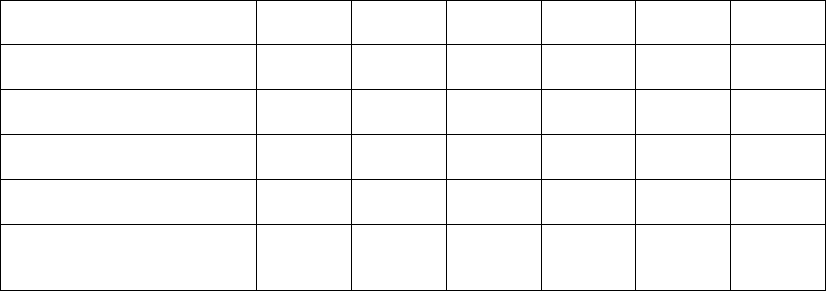
Table 6
Catastrophic Cases in One BOP Region, FY 2009 to FY 2013
Age
FY
2009
FY
2010
FY
2011
FY
2012
FY
2013
Total
Cases Involving Younger
Inmates
53 58 70 60 79 320
Cases Involving Aging
Inmates
58 76 104 104 126 468
Total 111 134 174 164 205 788
Percent of Aging Inmates
in this Region
16% 17% 18% 18% 19% 18%
Percent of Catastrophic
Cases Involving Aging
Inmates
51% 57% 60% 63% 61% 59%
Source: BOP catastrophic case data.
We also found that during this time, this region spent $71 million on
catastrophic medical care, 60 percent ($45 million) of which was spent on
aging inmates. Based on our review of available data, we found that aging
inmates received catastrophic medical services for a variety of medical
conditions, particularly heart and lung conditions. Services from this region
included treatment of clogged arteries, heart failure, cardiovascular issues,
respiratory failure, lung disease, and cellulitis. Finally, while the costs
associated with catastrophic care cases must all exceed at least $35,000, we
found cases with significantly more costs. For example, the most expensive
case from this region involved over $850,000 spent for an aging inmate who
was treated for complicated coronary artery disease.
In addition, we found that the increase in catastrophic medical cases in
this region was not limited to Care Level 3 institutions, which, as described
above, are specifically intended to care for outpatient inmates with medical
conditions that require daily to monthly outpatient clinical contact. For
example, a Care Level 2 institution, which incarcerates inmates who are
stable outpatients and typically require clinical contact only every 3 months,
accounted for 30 percent of the region’s catastrophic medical cases in
FY 2013. Aging inmates comprised 62 percent of this institution’s
catastrophic medical cases, even though they represented only 27 percent of
its population.
BOP institutions lack appropriate staffing levels to address the needs
of an aging inmate population and provide limited training for this
purpose
As described above, the increasing aging inmate population has
resulted in an increase in trips outside of institutions to address their medical
needs. We found that institutions lack Correctional Officers to staff these
trips and have limited medical staff within institutions to address aging
16

inmates’ medical needs. As a result, aging inmates experience delays in
receiving medical care. In addition, the needs of aging inmates differ from
their younger counterparts, including the need for increased assistance with
activities of daily living. According to BOP staff, however, staff is not
responsible for ensuring inmates can accomplish these activities. We found
that, instead, institutions rely on local inmate companion programs in which
healthy inmates provide assistance for aging or disabled inmates. Further,
aging inmates, specifically those with unique medical needs, also require
advanced release preparation. We found that Social Workers are uniquely
qualified and trained to address these needs, yet few institutions have them.
Finally, we found that institution staff has limited training to identify signs of
aging in inmate conduct, which can be mistakenly viewed as reflecting
disciplinary issues rather than signs that the inmate needs medical or mental
health care.
Understaffed health services units limit access to medical care and contribute
to delays for aging inmates
Aging inmates have an increased need for health services; but,
according to BOP officials, staff, and inmates, institutions lack adequate
health services staff to address these needs.
28
For example, the Clinical
Director of a medical center told us that only 80 percent of that institution’s
health services positions are staffed and that the vacancies limit the number
of inmates, including aging inmates, the institution can treat.
29
A Case
Manager at a nonmedical institution told us that the institution was “over a
thousand inmates behind” in servicing those enrolled in chronic care clinics.
An aging inmate told us that the health services staff at his institution is
“inundated” with requests for care and that, while they work hard, they can
only do so much. Aging inmates at numerous institutions also told us that
limited health services staff sometimes resulted in long waiting periods for
care.
30
For example, an aging inmate told us that he requested dentures in
28
BOP officials told us that hiring health service staff is difficult. According to the
Assistant Director for Human Resources, it is difficult to hire medical staff in urban areas
because the BOP cannot offer doctors and nurses salaries and benefits that are comparable to
those offered by private employers. Although the salaries and benefits are more competitive
in rural areas, the BOP is challenged with finding medical staff willing to live in remote areas.
The BOP uses some incentives such as periodically increasing employee pay, paying relocation
expenses, and offering to a pay a portion of student loans. Nevertheless, as of August 2014,
only 84 percent of the BOP’s medical doctor positions were filled, which is below the BOP’s
goal of 90 percent.
29
This medical center had two physician vacancies, two mid-level practitioner
vacancies, and several nurse vacancies open at the time of our fieldwork.
30
The BOP’s Assistant Director for Health Services and Medical Director told us that in
November 2014 the BOP launched a survey of inmates in all BOP institutions to assess
inmates’ access to healthcare. He told us that once the survey is complete, the Health
Services Division will analyze the results by institution. For institutions where inmates report
delays in receiving care, the BOP will try to determine the underlying causes of delay at each
institution in order to develop potential responses.
17

2010 and had yet to receive them.
31
He said this makes it extremely hard to
eat because he cannot chew food.
Additionally, the lack of an adequate number of health services staff
increases the need for outside care. A Case Manager told us that the lack of
health services staff at his institution has led to more emergency trips to
hospitals outside the institution because the institution does not have a
Physician Assistant to address medical needs. We also found that trips to
outside medical providers are often limited by the availability of Correctional
Officers to escort inmates. According to BOP policy, correctional staff is
required to escort inmates to outside medical appointments.
32
The limited
availability of Correctional Officers restricts aging inmates’ access to medical
care outside the institutions, and institution staff told us that, as a result,
there are waitlists to send inmates to outside medical specialists.
Using BOP data from one institution, we found that the average wait
time for inmates, including aging inmates, to be seen by an outside medical
specialist for cardiology, neurosurgery, pulmonology, and urology to be
114 days. The wait time at this institution increased to 256 days for those
inmates waiting to see outside specialists for additional or routine
appointments.
33
The Assistant Health Services Administrator at this
institution told us that there was no doctor at the institution and, while staff
used to be able to send inmates on 10 medical trips per day, the institution
now has the staff to provide only 6 planned trips and 2 emergency trips per
day. We found similar difficulties staffing outside medical trips at other
institutions. The Associate Warden at one institution told us his staff can
accommodate 6 trips to outside medical specialists per day, even though the
inmate population requires 8 to 10 trips per day. We also noted that outside
medical trips depend on appointment availability and that, while an
institution may be able to provide the necessary number of medical trips per
week, specialists in the community must also be available and willing to see
an inmate.
We additionally found that the management of outside medical care
waitlists affects the medical care provided to aging inmates. Specifically, we
were provided examples of inmate appointments not being rescheduled when
canceled, being rescheduled when the appointment had already taken place,
31
Inmates with dental problems, such as abscesses, that could cause harm if left
untreated, receive priority for dental appointments. The BOP’s Assistant Director for Health
Services and Medical Director told us that the BOP has also initiated a National Dental Waiting
List so that inmates awaiting dental care do not fall back to the end of the list if they are
transferred to a different institution.
32
BOP, Escorted Trips, Program Statement 5538.06 (August 29, 2014).
33
Only one institution tracked waitlist times, and we requested this data from the
BOP. Based on the data available to us, we could not determine how much of the delay in
receiving outside medical care is due to limited staffing and how much is due to limited
availability of appointments with specialists.
18

or not being scheduled at all. A Health Services Administrator told us that
inmates who are on waitlists for outside medical care can “fall through the
cracks” if their appointments are canceled and not rescheduled. An aging
inmate told us that he was sent outside the institution for a medical
appointment and 2 months later was rescheduled for the same medical need.
When he brought the issue to the Clinical Director, he was told that it was
just an appointment reminder. However, the inmate told us that he believes
staff did not realize he had already been seen. Another aging inmate told us
that at the time of our interview he had been waiting 2 years to be taken
outside his institution for an examination to receive eyeglasses and had
resorted to using a magnifying glass in the meantime.
The availability and purpose of inmate companion programs used to help
aging inmates accomplish their activities of daily living vary by institution
All inmates are expected to perform activities of daily living, including
dressing, cleaning their cells, and moving around within the institution.
However, staff told us that aging inmates often cannot perform these
activities on their own because of their medical conditions and staff is not
responsible for ensuring inmates can accomplish these activities. Some
institutions we visited have established local inmate companion programs to
address the increasing number of aging inmates who need assistance with
these activities. These programs utilize healthier inmates to provide support
to inmates, including aging inmates, who experience difficulty functioning in
a correctional environment.
Institution staff we interviewed found their local inmate companion
programs beneficial to both aging inmates and staff. For example, a Health
Services Administrator described to us an aging inmate with dementia and
Alzheimer’s disease who needed increased resources and attention. In this
case, an inmate companion served as staff’s “eyes and ears,” alerting them
to changes in the inmate’s behavior. A Counselor told us he does not know
how he would manage the unit without the assistance of inmate companions.
However, not all institutions have inmate companion programs. At one
institution without an inmate companion program, an Assistant Health
Services Administrator told us that aging inmates typically pair with a friend
or cellmate for assistance. A Health Services Administrator at another
institution said that inmates who cannot perform their activities of daily living
and require daily or weekly assistance beyond what the inmate companions
there are trained to provide are referred for transfer to an institution that can
meet their needs.
34
34
Inmates needing a medical transfer had been waiting for an average of 1–2 months
in October 2014. We further discuss issues regarding transfers for medical reasons below.
19
Also, the implementation of inmate companion programs varies by
institution, particularly between nonmedical institutions and medical centers.
For example, medical centers had local policies and position descriptions
establishing expectations for inmate companions. Inmate companions at one
medical center are expected to work in contact with bodily fluids and to help
care for inmates suffering from chronic and acute diseases. They also
provide assistance with moving inmates within an institution, feeding,
answering patient call lights, and changing diapers. However, at nonmedical
institutions, including those with high percentages of aging inmates, inmate
companion programs have no policies or job descriptions. Instead, inmate
companions are often referred to as “wheelchair pushers” because their
primary responsibility is to help inmates confined to a wheelchair travel
within an institution. Staff at two institutions we visited said they use inmate
companions only as part of their institution’s suicide prevention programs.
An Associate Warden told us that each of the eight institutions where he has
worked implemented its local inmate companion program differently. We
found other differences between how institutions implement inmate
companion programs, including:
• Training: At some institutions we visited, inmate companions are
provided training on medical safety standards, confidentiality, listening
skills, and job expectations. However, training at other institutions is
less extensive. For example, at one institution where inmate
companions are utilized as wheelchair pushers, inmate companions
complete 1 day of training on wheelchair ergonomics and safety
precautions. At another institution, there is no formal training for
wheelchair pushers.
• Selection: Each institution we visited that had an inmate companion
program selected inmates who were considered responsible and had
few misconduct incidents. Institutions with more robust programs also
require inmate companions to meet specific selection criteria, such as
having passed a General Education Development (GED) test.
• Compensation: At institutions we visited, inmate companion pay
varied based on companions’ levels of responsibility. For example, a
Counselor at an institution where inmate companions have more
responsibility told us that most companions are paid $40 a month. A
Case Manager at an institution where inmates have less responsibility
told us that companions are paid $5 to $7 a month.
• Oversight: One institution with a local inmate companion policy
developed a committee of nursing staff and selected inmate
companion representatives to oversee the program. The committee
reviews inmate companion assignments, develops plans of care, and
identifies training needs. At another institution, where the program
20

does not operate out of the health services or nursing departments,
unit teams informally manage the inmate companions.
35
According to institution staff and inmates, despite the benefits of and
need for inmate companion programs, aging inmates face risks when these
programs are inconsistently implemented. An aging inmate told us that most
inmate companions really try to help, but sometimes companions take
advantage of aging inmates. For example, a Supervisor of Education told us
about an inmate who had an inmate companion who was threatening the
inmate’s wife and forcing her to send money in return for the inmate’s
protection. The inmate told the Supervisor that it had been going on for a
long time but that he had been unable to tell institution staff because the
companion accompanied him everywhere, including to personal meetings
with staff. Institution officials and staff said that the inmate companion
program should be a standardized national program, with a program
statement establishing policies that hold inmate companions accountable for
their responsibilities. At one institution with program guidelines, inmate
companions are expected to sign the guidelines, acknowledging they will
abide by program rules. If a companion violates any of the guidelines, the
inmate companion committee conducts a misconduct review. Without the
protections or oversight of national guidelines, however, each institution can
run the program inconsistently.
Social Workers are uniquely qualified and trained to address the needs of
aging inmates, particularly with release planning, but few institutions have
Social Workers
We found that Social Workers are a great benefit for aging inmates.
While Case Managers, Counselors, Social Workers, and other institution staff
work in concert to prepare inmates for release, only Social Workers have
extensive training in addressing the unique needs of aging inmates. Licensed
Social Workers can proficiently help with aftercare planning, resource
brokering, and medical continuity of care during reentry. A Social Worker
told us that they help aging inmates with accessing medical services and
equipment in the community upon release.
However, relatively few institutions have Social Workers. Specifically,
as of November 2014, there were only 36 Social Workers throughout all of
the BOP’s institutions. A Social Worker told us that at her institution there
are approximately 1,000 inmates for every Social Worker. Another Social
Worker told us that because there are so few Social Workers, he has to
prioritize the inmates he helps based on their more difficult problems and
35
The unit teams consist of a Unit Manager, Case Managers, Correctional Counselors,
Unit Secretaries, Correctional Officers, an Education Advisor, and a Psychologist who work with
all inmates assigned to live in a particular housing unit. The unit team directly observes an
inmate’s behavior and can make recommendations in programming areas.
21

greater reentry needs, limiting his ability to assist all inmates, including
aging inmates.
36
Although the BOP employs six Regional Social Workers to
assist institutions that do not have a Social Worker, they are limited in
availability because each of them is responsible for between 15 and
17 institutions. We reviewed the BOP’s Community Release Planning
Guidelines for Social Work and found that it did not define any duties for
regional Social Workers that were distinct from the duties for institution
Social Workers. BOP institution staff told us that regional Social Workers
provide resources so that institution staff can work with individual inmates.
We also found that the lack of availability of Social Workers within BOP
institutions hinders the BOP’s ability to effectively prepare aging inmates to
reenter society because other BOP staff do not have the training unique to
Social Workers. A Case Manager at an institution with Social Workers told us
that she relies on Social Workers because they know things she does not,
such as the “ins and outs” of applying for Social Security benefits. A Case
Management Coordinator at an institution without Social Workers said that
he has to try to find resources on the internet to assist aging inmates in
applying for Social Security. Staff at institutions without a Social Worker also
told us about the benefits a Social Worker would bring to their institution,
including addressing issues related to halfway house placement, explaining
eligibility for benefits to many uninformed or confused aging inmates before
they are released, and removing some of the burdens placed on Case
Managers.
Recognizing the benefit that Social Workers play in helping inmates
prepare for release, the BOP recently approved and budgeted for the hiring
of seven additional Social Workers to be assigned to 5 correctional
complexes, 1 medical center, and 1 female institution.
Institution staff is not adequately trained to identify the signs of aging, which
mistakenly can be viewed as reflecting disciplinary issues rather than a need
for medical or mental healthcare
The BOP provides brief, limited training for institution staff on
recognizing the signs of aging in its Annual Refresher Training, which states
that the significant increase in aging inmates requires staff to contend with
increased mobility issues, terminal illness, and cognitive impairments. The
training includes ways staff can be aware of changes in aging inmates and
provide increased monitoring to help with inmates’ cognitive and physical
deterioration. The training further elaborates on aging inmates’
36
In October 2014, the BOP released Community Release Planning Guidelines for
Social Work (Guidelines) to assist inmates in identifying necessary community resources for
release planning. While these Guidelines identify Social Workers as a resource for inmate
release planning, Social Workers are currently available only at Care level 3 and 4 institutions,
making their availability to Care level 1 and 2 inmates limited.
22
vulnerabilities, such as being forgetful, losing track of time, taking longer to
complete tasks, not being able to follow directives, and having increased
physical stress. The training also informs participants that aging inmates will
require time and understanding to acclimate to an institutional environment.
However, the Annual Refresher Training Instructor Guide states that training
on signs of aging as well as medical emergencies can be completed in
30 minutes.
The Assistant Director for Human Resources told us that the BOP
currently trains all staff to meet the local needs of its population and that, as
a result, staff at Care Level 3 and 4 institutions should be able to recognize
mobility issues and make necessary accommodations. However, we found
that inmates in Care Level 2 institutions also have mobility issues that would
require staff to recognize and accommodate those and other health issues in
aging inmates. For example, an anemic, wheelchair-bound aging inmate at a
Care Level 2 institution told us that he was disciplined several times for
pushing himself inside a building to wait for his medication rather than
waiting outside, including in cold weather, to receive it.
In March 2010, the BOP’s National Institute of Corrections (NIC)
released a training video on aging inmates, aimed at officials running state
and local institutions, which said that the most critical step institutions could
take to address an aging inmate population is staff training. According to the
video, training is important to help staff understand that aging inmates may
have a medical reason that explains behavior that would otherwise be
subject to discipline, such as an aging inmate who is in the wrong place
because he has dementia. Institution staff with whom we spoke agreed that
this type of training at the BOP would be helpful and provided us examples.
A Case Manager described to us how she once asked an inmate several
questions and received strange responses. She said she thought the inmate
was trying to “fool her,” but she later learned that the inmate had medical
conditions that prevented him from responding. She said training on how to
recognize behaviors resulting from dementia or other debilitating conditions
would be helpful. A Social Worker also said staff should be trained to
understand the behaviors associated with dementia. The Assistant Director
for the Health Services Division and Medical Director said that the BOP has
started to put more into annual training regarding officer sensitivity but that
the BOP should permanently incorporate training specifically for the care of
aging inmates across the institutions.
The physical infrastructure of BOP institutions cannot adequately
house aging inmates
The BOP’s mission includes confining federal offenders in controlled
environments that are safe, humane, cost-efficient, and appropriately secure.
However, the BOP’s ability to confine its aging inmate population is
insufficient due to overcrowding in its institutions, as well as problems with
23

their internal and external infrastructures. Lower bunks, essential for
accommodating aging inmates with mobility limitations or medical conditions,
is limited by the overcrowding of BOP institutions. As a result, institutions do
not always have enough lower bunks as well as handicapped-accessible cells
and bathrooms, and others cannot accommodate the number of inmates with
mobility devices that require elevators. Further, aging inmates cannot
consistently navigate the narrow sidewalks and uneven terrain at some
institutions. Staff and inmates told us that separate housing units, or entire
institutions, would be more appropriate to house aging inmates.
Lower bunks are limited due to the overcrowding of BOP institutions
According to BOP staff and officials, aging inmates generally require
lower bunks because of their physical limitations and risk of falling.
However, BOP institutions are consistently overcrowded, limiting the number
of available lower bunks.
37
Several officials and staff told us that their
institution has run out of lower bunks for aging inmates. We found that the
lack of sufficient lower bunks affects aging inmates in several ways.
First, the lack of lower bunks may prevent or delay aging inmates from
receiving lower bunks. Consequently, aging inmates may be housed in upper
bunks until a lower bunk becomes available. For example, a Warden told us
that aging inmates are sometimes assigned to an upper bunk out of
necessity, which could be a problem for aging inmates because climbing into
an upper bunk is not always easy. During our visits to BOP institutions, we
observed upper bunks that did not have ladders or steps, which required
inmates to climb on desks, chairs, or makeshift pedestals to access the upper
bunks.
Second, the lack of lower bunks has forced institutions to retrofit other
space to create additional lower bunks. A Supervisor of Education told us
that her institution was unable to accommodate all of the inmates who
needed lower bunks. As a result, the institution had to add beds to a room
not originally intended for housing. We also found that institutions modified
or added lower bunks within existing housing cells to accommodate aging
inmates and inmates with mobility limitations, including retrofitting two-man
cells or “cubes” to hold three inmates. A Case Manager told us that while
many three-man cells are composed of one double bunk and one single
bunk, her institution created some triple-level bunk beds in which both the
middle and bottom bunks are considered “lower bunks.” She also told us she
observed inmates with histories of seizures and high blood pressure receiving
middle bunks, which she said could create a liability for the BOP if the
inmates were to fall.
37
In FY 2013, the BOP as a whole operated at 36 percent over capacity and aging
inmates represented the fastest growing segment of the BOP’s population.
24

Finally, the lack of lower bunks requires staff to regularly reassign
lower bunks by prioritizing and reorganizing bed assignments, which
sometimes creates tension among the inmates being moved. Specifically,
institution staff told us that managing lower bunks can be a very difficult,
time-consuming endeavor and that it often takes a collaborative effort
between inmates and staff from other units to accommodate aging inmates.
A Counselor told us that trying to find a lower bunk is comparable to “finding
a needle in a haystack.” Moreover, accommodating aging inmates with lower
bunks has repercussions. Staff from institutions across all security levels
described to us situations in which moving a younger inmate to an upper
bunk to accommodate an aging inmate created tension or animosity within
the housing unit. In one case, a Counselor told us that the tension from
assigning a younger inmate from a lower to an upper bunk led to an assault.
To help manage lower bunks, institution medical staff issues lower
bunk passes to those inmates who meet criteria in a memorandum issued in
June 2012 by the Assistant Director of the BOP’s Health Services Division.
The memorandum, entitled “Lower Bunk Criteria,” standardizes the
assignment of lower bunks across the BOP by providing specific medical
criteria for institution medical staff to consider before assigning a lower
bunk.
38
However, several nonmedical institution staff told us that lower bunk
passes are given to inmates who do not need them. One Counselor said that
there is a disconnect between medical and nonmedical staff concerning
inmates’ needs for lower bunk passes. We found that other institutions faced
similar circumstances and issued lower-bunk passes exceeding the
availability of lower bunks. A Health Services Administrator told us that his
institution was operating at maximum lower-bunk capacity at all times and
provided us with a document that showed 452 inmates had lower bunk
passes at that time while the institution had only 444 lower bunks.
Overcrowding also limits the BOP’s ability to move aging inmates to the
institutions that best address their medical needs
The BOP primarily utilizes its Care Level 3 and 4 institutions to house
inmates with the most significant medical issues. The BOP’s Care Level 3
institutions treat inmates with medical conditions that require daily to
monthly outpatient clinical contact. These inmates may also require
assistance in some activities of daily living. But, we found that inmates
needing a transfer to a Care Level 3 institution may be temporarily housed in
38
The memorandum identifies a range of specific medical conditions for which a lower
bunk pass is recommended, including but not limited to orthopedic conditions, neurological
conditions, blood-clotting problems, balance problems, pregnancy, and obesity. The
memorandum does not specify at what age an inmate should receive a lower bunk. However,
staff told us they attempt to assign lower bunks to inmates by age, which varied by institution.
At one institution, the Health Services Administrator stated that he always places inmates over
the age of 70 on lower bunks. A Counselor at a different institution said that the majority of
inmates over the age of 55 are in lower bunks.
25

the receiving institution’s Special Housing Unit while waiting for an available
bed.
39
A Medical Designator in the BOP’s Office of Medical Designations and
Transportation told us that when an inmate is being transferred due to
medical needs, the BOP may decide to transfer the inmate as quickly as
possible, even if that means the inmate has to be assigned to the Special
Housing Unit until a bunk in the general population becomes available. An
Assistant Health Services Administrator and a Case Manager at a Care
Level 3 institution confirmed that their institution has sometimes placed
aging inmates in their institution’s Special Housing Unit until a bunk became
available elsewhere in the institution.
Access to the BOP’s Care Level 4 institutions, which comprise the
BOP’s six medical centers, is determined, in part, by the availability of bed
space, and we found that transfers to these institutions are often difficult to
complete in light of overcrowding. Inmates waiting for transfer to a BOP
medical center must remain in their institution’s general population until a
bed becomes available or their condition worsens. A Health Services
Administrator told us that inmates waiting for transfer place a huge strain on
staff because his institution does not have an infirmary. A Case Manager told
us that space is at a premium at the medical centers and if an inmate’s
condition is not an emergency most inmates will wait 2–3 months for a
transfer. We asked the BOP for all data on pending medical transfers and
found that in October 2014 two inmates awaiting an emergency transfer had
been waiting on average 11 days, inmates awaiting a routine urgent transfer
had been waiting an average of 31 days, and inmates awaiting a routine
transfer had been waiting an average of 57 days.
40
If an inmate’s condition
worsens, he is sent to a local hospital at government expense until the BOP’s
Office of Medical Designations and Transportation can approve his transfer to
a medical center.
A Medical Designator in the Office of Medical Designations and
Transportation said that institution staff is always inquiring about the wait
period for transfer, often requesting that inmates be transferred sooner.
However, because transfers depend on the availability of bed space, inmates
are placed in a queue and have to wait for a bed to become available in a
BOP medical center. A Health Services Administrator at a medical center told
us that one of her biggest concerns is delaying care for inmates who need to
39
A Special Housing Unit is a separate unit used to segregate inmates in
administrative detention status or disciplinary segregation status from the rest of the inmate
population. Inmates can be in administrative detention status for a variety of reasons,
including a pending transfer to another institution or a need for protection from the general
population. Inmates in disciplinary segregation status are being punished for violating
institution rules. See 28 C.F.R. §§ 541.20–541.24.
40
Routine urgent transfers occur for medical conditions such as operative wound care
and dialysis. Routine transfers occur for medical concerns such as poor medication compliance
or for further evaluation pending surgery approval.
26

transfer to her institution but cannot do so because there are no available
beds.
Institutions have difficulty accommodating inmates requiring handicapped-
accessible facilities
All BOP institutions are required to comply with the Architectural
Barriers Act of 1968, which requires that public buildings and infrastructure
be accessible to individuals with disabilities, including handicapped-accessible
hallways, doors, and cells.
41
The specific guideline addressing institutions
and cells states that “accessible cells or rooms should be dispersed among
different levels of security, housing categories, and holding classifications to
facilitate access.” Officials from the BOP’s Administrative Division said each
institution is built to meet all accessibility standards that were in place at the
time of its construction, with newer institutions being more accessible than
older institutions. However, the Deputy Chief from the BOP’s Design and
Construction Branch told us that some BOP institutions were built over a
century ago and many continue to have accessibility difficulties even after
retrofitting and renovation. A Case Manager at a medical center told us that
the institution is old and that many of the units cannot house wheelchair
inmates because they do not have wide enough doors. Also, BOP officials
and staff told us that the infrastructure of more recently built institutions was
not designed to handle the number of aging and handicapped inmates who
are housed in these institutions.
The BOP’s care level system has led to higher concentrations of aging
inmates in institutions with higher care levels and more inmates needing
handicapped-accessible infrastructure than the institutions were designed to
handle. During our visits to BOP institutions, we found a number of
infrastructure difficulties that limit the BOP’s ability to provide appropriate
accommodations to house aging inmates, particularly those with physical
disabilities. Institution staff expressed similar concerns regarding the
accessibility of housing units. Due to housing limitations, inmates using
wheelchairs and walkers are often housed together, creating cells with very
limited space. In one case, a Social Worker observed a cell that housed two
wheelchair inmates together where the wheelchairs had to be placed outside
the room because the cell could not accommodate both wheelchairs. We
were also told that when multiple inmates with physical disabilities are
housed in the same unit their wait time for the limited number of accessible
showers and bathrooms increases. An aging inmate told us that his unit
houses approximately 160 inmates, with only one handicapped-accessible
toilet. A second inmate in the same unit confirmed that, as a result, he often
sees wheelchair-bound inmates waiting in line for that toilet because the rest
of the toilet stalls are too narrow to accommodate wheelchairs.
41
42 U.S.C. §§ 4151–4157.
27
We found that institutions also have difficulty accommodating the
growing number of aging inmates who need elevators. A Case Manager told
us that many units could not house aging inmates with mobility issues,
particularly those who require a wheelchair, because the units lack elevators.
In these cases, inmates with mobility issues are housed in the same unit,
increasing the use of elevators to that unit. Staff at several institutions said
that as a result, a common problem is frequent elevator outages, which may
take days to be repaired. A Social Worker told us that she observed inmates
walking down stairs with walkers because elevators were broken. We found
that some institutions had handicapped-accessible cells and lower bunks that
could be accessed only by stairs, and therefore aging inmates who may need
the additional space provided in handicapped cells have to climb stairs to
reach the larger cells or be placed in a regular-size cell within the general
housing unit. At one institution we visited, staff and inmates told us that
aging inmates with mobility issues sometimes have to walk up stairs to the
second floor to access their lower bunk. One inmate told us that sometimes
inmates with walkers remain assigned to an upstairs housing unit for weeks
until space becomes available on the bottom floor. Staff from another
institution told us that their institution was not handicapped accessible
because inmates have to navigate steps in order to reach their cells.
Inmates who cannot climb stairs cannot be housed at the institution and
must be transferred to a nearby BOP institution.
Institutions have the authority to pay for their own maintenance and
small renovation projects. We found that one institution had to retrofit
education space to create a wheelchair repair shop due to the number of
wheelchair-bound inmates. However, an institution cannot spend more than
$10,000 of its own funding on renovations and larger projects have to be
coordinated with their regional office or the BOP’s Central Office. The Chief
of the BOP’s Facilities Programs told us that institutions rarely submit
proposals to the BOP’s Central Office for major renovations to make housing
units more accessible.
We also found that from 1994 to 1996 the BOP inspected all
institutions to evaluate their accessibility for inmates with mobility
impairments and funded recommended renovations based on those
inspections. For example, an inspection in one institution found that the
medical and dental areas were accessible only by stairs. As a result, the
institution had an elevator installed in that area to make it accessible for
inmates with mobility issues. The Chief of the BOP’s Facilities Program
stated that all high-priority and some of the medium-priority renovations
were completed but that renovations funded by the Central Office stopped
prior to addressing the lowest priorities. We were also told that the BOP has
not conducted another BOP-wide review of the accessibility of all institutions
since 1996.
28

External infrastructure, including narrow sidewalks and uneven terrain,
present difficult and sometimes unsafe conditions for aging inmates to
navigate
We found that the conditions of the external infrastructure of some
institutions, such as uneven terrain or narrow sidewalks, makes it difficult
and sometimes unsafe for aging inmates, particularly those with mobility
issues, to move within the premises. A Clinical Director said some housing
units are far from the cafeteria, on uneven terrain, and become dangerous in
snow or inclement weather. In addition, a Counselor told us that the visiting
room at his institution is at the top of a hill and wheelchair-bound inmates
have to use a service road to access the visiting room, rather than the stairs
the other inmates can use. Further, many of the handicapped inmates at
this institution are located at the bottom of a hill because that is where the
only handicapped-accessible units are located. An inmate at this institution
also told us that the sidewalks are narrow and do not allow enough space to
accommodate inmates in a wheelchair.
42
Additionally, a Warden at another
institution told us that the housing units at his institution are on a hill, which
makes it harder for aging inmates in wheelchairs and walkers to move about.
He said that while the institution was built less than 20 years ago, it was not
built to accommodate the number of aging inmates in wheelchairs and
walkers currently housed there. To address challenges associated with an
institution’s external infrastructure, we found that in some cases institution
staff would move aging inmates to housing units that are closer to common
areas to shorten walking distances. However, as described above, bed space
and accessible areas are often limited and not all aging inmates can be
placed in accessible areas.
According to BOP staff and officials, separate units, or entire institutions,
would be more appropriate to house aging inmates
The BOP does not provide specialized housing units based on age.
Some staff told us that the current system of having housing units contain a
mix of ages enables aging inmates to mentor younger inmates and that the
presence of aging inmates in general improves the behavior of the entire
inmate population. The BOP operates a number of segregated or specialized
housing units, including units for inmates under administrative detention or
disciplinary segregation and units to provide programming and treatment for
sex offenders, drug offenders, and inmates diagnosed with mental health
conditions. The BOP’s Assistant Director for Health Services and Medical
Director told us that BOP officials have discussed the possibility of similarly
housing aging inmates together. However, he said that doing so would
42
During our visit to this institution, staff showed us how wheelchairs take up nearly
the entire width of sidewalk and explained that not only was this unsafe for inmates in
wheelchairs, it was also problematic for other inmates since they are not permitted to walk on
the grass.
29

require “a real trade-off” because it would require the BOP to house many
aging inmates farther away from their families.
43
However, other staff and inmates provided several reasons why
separate units, or entire institutions, would be more appropriate to
accommodate the increasing population of aging inmates. For example, and
as described above, the internal and external infrastructures of institutions
often limits the BOP’s ability to safely confine its aging inmate population. A
Unit Manager suggested that given the number of aging inmates at his
institution, the BOP should retrofit an entire building dedicated to
accommodating aging inmates who need lower bunks that are strategically
located in areas easily accessible to certain institution services, such as
healthcare. A Clinical Director told us that the BOP should create a separate
institution for aging inmates with an “aging-friendly infrastructure” in a
location that has flat terrain. Additionally, a Counselor told us that having
aging-inmate units with dedicated, round-the-clock nursing support could cut
down on medical costs because a nurse could consistently help with their
chronic health issues. The Assistant Director for the Administration Division
said that requests for geriatric units and institutions have been made before,
and that he would “love” to have these units if it did not require costly
construction.
In addition, BOP officials and staff told us that separate housing units
or institutions would provide safer housing for aging inmates who may be
more susceptible to being victimized by younger inmates. While we were
told that younger inmates often respect aging inmates, we were also told
that younger inmates sometimes victimize aging inmates.
44
For example, a
Unit Manager in a Care Level 3 institution told us that his institution receives
aging inmates directly from a BOP medical center and houses them in the
general population. He said this is an unsafe practice because they are
vulnerable to being victimized when surrounded by younger inmates.
The BOP does not provide programming opportunities specifically
addressing the needs of aging inmates
All BOP institutions offer programs and activities for inmates to further
their education, obtain vocational and occupational training, practice their
religion, enhance interpersonal and life skills, and participate in recreation
43
The BOP considers incarceration close to family members an important aspect of an
inmate’s rehabilitation and therefore attempts to place inmates in institutions that are within
500 miles of the release area, especially when an inmate is within 36 months of release.
44
We requested data from the BOP on incidents where aging inmates were victimized
by younger inmates, but we were informed that the BOP does not keep statistics in this
manner.
30

and leisure activities.
45
However, there are no programs, and limited
activities, that specifically address the needs of aging inmates, many of
whom have already obtained an education or do not plan to seek further
employment once released. Aging inmates who want to participate in
programs face obstacles, including having already completed all the
programs available at an institution. Institution officials and staff told us that
the lack of programming and activities specifically designed for aging inmates
makes them more likely to be idle and not participate in any activities or
programs at all. Finally, general release preparation programs do not
address the unique release programming needs of aging inmates.
There are no programs, and limited activities, specifically designed or
appropriate for aging inmates
All BOP institutions are required to provide GED classes, as well as
English as a Second Language, Adult Continuing Education, and parenting
classes, and to have a library.
46
The BOP also offers programs with
standardized curricula in multiple institutions for residential and
nonresidential drug treatment, psychological treatment, occupational
education classes that teach trade skills, and work through Federal Prison
Industries, or UNICOR.
47
In addition, institutions have the flexibility to
develop local programs.
At the outset of our review, the BOP told us that there are no
programs specifically designed for the needs of aging inmates but that aging
inmates participate in standardized programs and local programs. The
Assistant Director of Correctional Programs said there are no programs set
aside for inmates of a particular age and that everything is based on inmate
need rather than age. A Supervisor of Education also told us there are no
age-specific programs but there are activities such as music appreciation and
45
Programs are formal educational opportunities, with start and end dates, required
attendance, a curriculum, and measurable achievement standards. Activities are less formal
events, including one-time events and sports or game tournaments, in which inmates can
participate for recreation.
46
Detention centers, metropolitan correctional centers, and the Oklahoma City
Federal Transfer Center are exempted from providing programs beyond these minimal
requirements. Additionally, satellite camps (minimum-security camps next to a larger,
higher-security institution) are exempt but more programs are available at the higher-security
institutions to which the camps are attached.
47
Federal Prison Industries, commonly referred to by its trade name UNICOR, is a
wholly owned government corporation whose mission is to employ and provide job skills
training to the greatest practicable number of BOP inmates and produce market-priced quality
goods and services for sale to the federal government with minimal impact on private business
and labor. See http://www.bop.gov/inmates/custody_and_care/unicor.jsp
. See also DOJ,
OIG, Audit of the Management of Federal Prison Industries and Efforts To Create Work
Opportunities for Federal Inmates, Audit Report 13-35 (September 2013),
http://www.justice.gov/oig/reports/2013/a1335.pdf (accessed April 9, 2015).
31
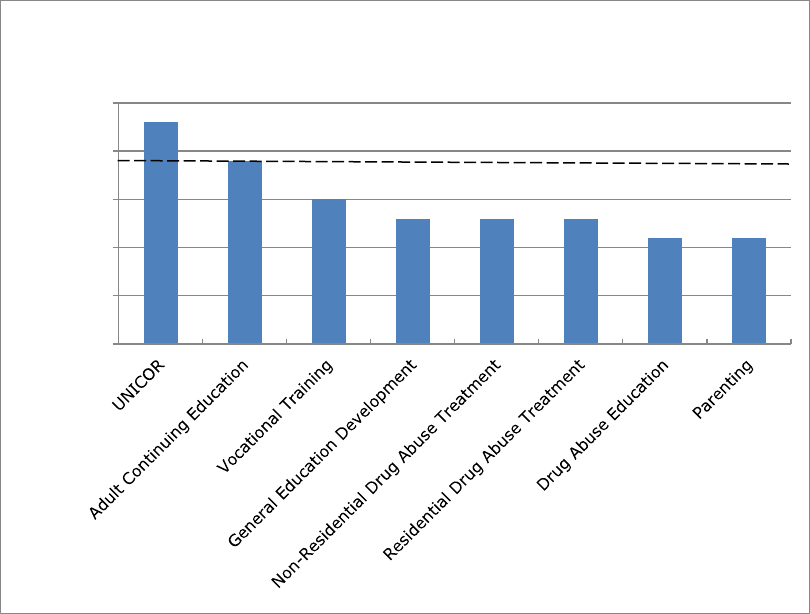
exercise courses that aging inmates gravitate toward. We reviewed the
BOP’s Directory of National Programs and found that the BOP has
18 standardized programs but none specifically addressing the needs of
aging inmates. Finally, when we asked BOP officials and staff whether aging
inmates had different needs than younger inmates, they cited different
physical needs but did not cite different programming needs related to age.
Institution staff told us that they frequently recommend the BOP’s
standard parenting class to aging inmates because many of them have adult
children and grandchildren. However, we found that this program had one of
the lowest rates of aging inmate participation. According to BOP data, only
11 percent of inmates who participated in the parenting program in FY 2013
were aging inmates. Overall, we found that aging inmates participated in
only two of the BOP’s eight largest standardized programs at rates equal to
or higher than their percentage of the overall BOP population. (See Figure 4
below.)
Figure 4
Aging Inmate Participation in the BOP’s Largest Programs, FY 2013
0%
5%
10%
15%
20%
25%
Percentage of Participation
Program
--- BOP Aging Population
Note: The figure includes only those programs that had more than 10,000 inmate
participants in FY 2013. Adult Continuing Education was the largest program, with
71,235 participants, including 13,693 aging inmates.
Source: BOP program participation data.
32

BOP officials and institution staff also suggested local health and
wellness programs for their aging inmates because aging inmates often have
health concerns. We were unable to evaluate aging inmate participation in
these programs because inmate participation in local programs is tracked
only at the local level and we were told that the programs offered vary by
institution.
Although BOP officials and staff told us that programs do not focus on
inmate age, we found one that the BOP created exclusively for younger
inmates. The Bureau Rehabilitation and Values Enhancement (BRAVE)
program is designed for medium-security male inmates who are 32 or
younger, have a sentence of at least 60 months, and are beginning their first
federal sentence. The BOP describes the program as helping inmates adjust
to incarceration and reducing their incidents of misconduct. In FY 2013, not
more than 2,580 inmates met the criteria for the BRAVE program.
48
Meanwhile, in FY 2013, there were 30,962 aging inmates for whom no
specific programs existed.
While institutions have the flexibility to create programs that could address
aging inmates’ needs, few have such programs
According to the BOP, each institution can assess where its inmates’
interests lie and offer programs and activities that appeal to the interests and
needs of its population. However, despite having the flexibility to develop
and offer local institution programs, we found that even institutions with a
high percentage of aging inmates did little to identify the unique
programming needs of aging inmates who already have an education or job
skills and to provide programs to address their unique needs. A Supervisor
of Education said that age has a big impact on the types of programs inmates
participate in because aging inmates are less likely to participate in physically
demanding activities. Staff at the institutions we visited told us that their
institutions could do more for the aging inmates and that if programs for
aging inmates were offered, those inmates would be more interested in
participating. For example, a Reentry Coordinator told us his institution held
a health fair for inmates of all ages and found it was popular with aging
inmates because it gave them the opportunity to learn about age-related
diseases. A Case Manager suggested to us that the BOP should survey its
aging inmates to determine what additional programming they would like to
see. Other staff said the BOP should implement programs similar to those
offered at nursing homes or community senior centers, such as disease
awareness and therapy. Aging inmates described to us a number of
additional programs that would meet their needs, including a wider variety of
48
We could not determine from BOP data how many inmates were serving their first
federal sentence, but we could determine that there were 2,580 medium-security male
inmates age 32 or younger who began serving sentences of 60 months or more during
FY 2013. BRAVE is offered at two institutions.
33
computer classes, wellness classes on prolonging physical and mental health,
foreign languages, college preparation or similar academic courses to keep
their minds sharp, singing, and quilting.
Aging inmates who want to participate in programs face obstacles
We found that even when aging inmates are interested in participating
in programs, their ability to participate can be hindered by a lack of programs
that are new to them. Aging inmates at institutions we visited told us that
the number of programs available was limited and rarely changed. Inmates
at different institutions said that they participated in more programs at the
beginning of their incarceration but had completed everything of interest to
them after a few years, or that their institutions never offered programs that
interested them.
We also found that aging inmates might not participate in programs to
avoid revealing their vulnerabilities or limitations to younger inmates. One
Warden told us that some aging inmates ask to be exempt from GED classes
because they do not want other inmates to discover they cannot read. An
aging inmate at a different institution agreed, saying that she had seen
inmates become discouraged and embarrassed in the GED classes because
they were so far behind academically.
Further, the Assistant Director for the Industries, Education and
Vocational Training Division told us that the BOP has the responsibility to
accommodate aging inmates’ physical needs so that their participation in
programs is not limited. Some aging inmates have physical limitations that
make program participation more difficult, and so some institutions have
devised alternatives to facilitate program participation. For example, an
Assistant Supervisor of Education told us that her institution had begun
providing books from a local library as a substitute to attending classes for
aging inmates who cannot physically leave their units.
Activities designed specifically for aging inmates are limited
BOP institutions are required to provide recreational activities for
inmates to pursue in their free time. Institution staff told us they often
recommended art, music, and hobby classes for aging inmates. Some of the
aging inmates we spoke with participated in these and other low-impact
activities such as reading in the library, playing cards or other games, and
exercise such as walking on the track. However, in other cases, aging
inmates who may want to participate in more physical activities cannot keep
up with younger inmates. Overall, we found that a few of the institutions we
visited considered age when designing activities, mainly by creating athletic
leagues with varying age cutoffs to increase opportunities for aging inmates
to participate. One institution we visited established a basketball league for
inmates age 35 and older, while a second institution has a league for inmates
34

age 40 and older, and a third institution has a league for inmates age 50 and
older. However, not all institutions offered age-specific athletic leagues.
Beyond athletic leagues, only 1 of 13 institutions we visited offered an
activity designed specifically for aging inmates: an aerobics and nutrition
class for inmates age 65 and older, which was held at a BOP institution with
one of the highest percentages of aging inmates.
Due in part to the lack of programming and activities designed
specifically for aging inmates, idling is a common sight in BOP institutions,
according to institution officials and staff. However, one inmate told us that
aging inmates do not idle by choice, but rather because there is nothing for
them to do. Another inmate said that the aging inmates who idle seem to
deteriorate mentally and become depressed.
The BOP does not address the specific release needs of aging inmates
Aging inmates often have different release needs than do younger
inmates. We found that the BOP’s release preparation program focuses on
workforce reentry and does not address the unique circumstances, such as
finding new healthcare providers or collecting Social Security benefits, which
apply to aging inmates. We also found that aging inmates’ increased
healthcare needs can make transitioning into home confinement difficult.
49
Pre-release programs do not address the unique needs of aging
inmates
The BOP implements a release preparation program in all institutions
to prepare inmates to reenter the community and the workforce in
particular.
50
Each institution designates a staff member to determine the
release needs of the institution’s population and coordinate a release
preparation program. The program consists of six core topics: health and
nutrition, employment, personal finance, community resources, release
procedures, and personal development, with each institution developing its
own program to address each core topic.
We found that institutions we visited provide release preparation
information to every inmate on the same six core topics rather than tailoring
the information to individual inmates or categories of inmates. For example,
one of the six core topics in the release preparation program focuses on
employment. However, release preparation programs do not consistently
49
The BOP’s Home Confinement Program allows federal inmates to live at home and
work at gainful employment while remaining in official detention status. To participate,
inmates must be within the last 6 months or 10 percent of their sentence.
50
BOP, Release Preparation Program, Program Statement 5325.07 (December 31,
2007). The OIG is currently reviewing the BOP’s implementation of this program. See
http://www.justice.gov/oig/ongoing/bop.htm (accessed April 9, 2015).
35

include assistance for those aging inmates who will not be employed after
release. We found that programs that did include assistance for those aging
inmates briefly discussed accessing Social Security or Veterans benefits, but
did not include community reintegration. A Supervisor of Education told us
that institutions have the responsibility to prepare inmates to rejoin their
communities; but if an inmate’s role in that community will be as a retired
person, his or her needs will greatly differ from someone reentering the
workforce.
Aging inmates told us that the information provided in release
preparation programs was not helpful for them and that topics that would be
helpful for their release were not discussed. For example, one inmate told
us, “You have what they call core programs, such as learning to save money,
learning to buy a house, and learning to bring up a family. I’m 67 and I have
two houses. And I still have to [take these] programs? . . . [Aging inmates]
don’t need to take that. We’ve already accomplished that.” Another inmate
said that he worries about being released after retirement age and would like
to have programs that prepare him for that future. “What’s going to happen
when I step out at 70? Because if I live to be 70, I’m going to reenter
society when I’m past the working age. So how will I survive? . . . What do I
do with my medical issues? How am I going to provide for myself if there’s
no family support?”
Institution staff described to us several ways in which they believed
BOP release preparation programs could be adapted to address aging
inmates’ needs. For example, a Social Worker suggested that the BOP tailor
life skills programs for different age cohorts so that younger inmates could
learn how to search for jobs and live independently while aging inmates could
learn how to apply for Social Security benefits and find assisted living
communities. Institution staff also suggested that aging inmates be provided
with updated information on life skills, such as online banking, and on health
situations that people encounter as they age, such as managing blood
pressure.
Insufficient support and access to medical care may limit the
placement of aging inmates on home confinement
The BOP has the authority to assign inmates to home confinement for
up to the final 6 months of their sentences.
51
Although the population of
aging inmates placed on home confinement is relatively small, aging inmates
placed on home confinement increased 258 percent, from 161 to
577 inmates, from FY 2009 through FY 2013.
52
Institution staff told us that
51
BOP, Home Confinement, Program Statement 7320.01 (September 6, 1995).
52
During this time, the total number of inmates placed on home confinement
increased 323 percent, from 382 inmates in FY 2009 to 1,616 inmates in FY 2013.
36

home confinement is a good option for many aging inmates. Specifically,
institution staff said that as long as an inmate has the resources to pay for
medical care, home confinement offers more flexibility in addressing his or
her medical needs.
53
However, we were told that there are a number of obstacles,
particularly concerning access to medical care, that limit the BOP’s ability to
place aging inmates on home confinement. A Social Worker told us of an
aging inmate with dementia who was released from a medical center into
home confinement. The inmate returned just days later because he did not
have sufficient support to live in his home. Subsequently, the inmate had to
serve the remainder of his sentence in the medical center’s inpatient unit
because his dementia could not be managed in the general population.
Institution staff also expressed liability concerns because the BOP remains
ultimately responsible for an inmate’s medical care while the inmate is on
home confinement. The Assistant Director for Health Services and Medical
Director said that the BOP has an obligation to link inmates being released to
home confinement with healthcare providers in their communities but after
that connection is made it is ultimately up to the inmate to visit the provider
for care. He further said that inmates on home confinement are eligible to
enroll in Medicaid, Medicare, or private insurance and that BOP Social
Workers can help facilitate this enrollment.
54
Aging inmates commit less misconduct while incarcerated and have a
lower rate of re-arrest once released
Based on BOP data and feedback from officials and staff, we
determined that aging inmates engage in fewer disciplinary problems during
their incarceration. For example, aging inmates have been sanctioned for
disproportionately fewer misconduct incidents compared to younger inmates
during their incarceration. Also, in considering the impact that releasing
aging inmates has on public safety, aging inmates have a lower rate of
re-arrest in comparison to younger inmates and the rate of re-arrest
decreases with age. Those aging inmates who are re-arrested often have a
53
Unlike inmates in institutions, inmates on home confinement do not have to wait
for an institution to schedule a trip for an outside medical appointment. Additionally, inmates
on home confinement do not have to adhere to halfway house rules on employment and
check-in hours, making their schedules more flexible for arranging medical appointments.
Finally, home confinement may be more appropriate than halfway houses for aging inmates
who will be retired since the primary purpose of halfway houses is to support inmates seeking
employment.
54
The Assistant Director of the Reentry Division said that institution staff focuses on
enrollment in benefits programs, in lieu of employment skills, for aging inmates who may not
be seeking employment. She further said that Medicaid enrollment is particularly challenging
because, although no one can receive Medicaid benefits while in an institution, the rules vary
from state to state regarding eligibility for benefits and whether inmates can submit their
Medicaid applications while they are still in an institution or only after release.
37

history of criminal behavior and are most commonly arrested for drug
offenses.
Aging inmates engage in fewer misconduct incidents while incarcerated
compared to younger inmates
According to BOP data, 53,885 inmates engaged in misconduct
incidents consisting of violations of institution rules at least once during
FY 2013. We found that aging inmates represented about 10 percent
(5,621) of these misconduct incidents, while accounting for 19 percent of the
BOP’s total population during that period. Further, the misconduct of aging
inmates was typically of lower severity. According to BOP data, 67 percent
of aging inmates’ misconduct was of moderate or low severity compared to
60 percent of younger inmates’ misconduct.
55
This data is consistent with what we were told by BOP officials and
institution staff. In general, they said that aging inmates are less likely than
younger inmates to violate institution rules. The Director of the BOP’s Office
of Research and Evaluation stated that age is one of the biggest predictors of
misconduct, and that inmates tend to “age out” of misconduct as they get
older. Further, if aging inmates engaged in misconduct incidents, it was
usually for less serious infractions that did not demonstrate violent or
aggressive behavior. For example, a Social Worker told us that an aging
inmate with dementia engaged in a misconduct incident by not standing up
during the daily inmate count. Another Case Manager said that if aging
inmates engage in misconduct incidents it is more likely to be for refusing to
participate in programs, often because they are not motivated. As discussed
below, we found similar trends in our analysis of aging inmates who were
re-arrested after release from BOP custody.
Aging inmates have a lower rate of recidivism compared to younger inmates
At the outset of this review, the BOP told us they were unaware of any
entity with comprehensive data on recidivism, including data on the
recidivism of inmates age 50 and older. BOP research from over 20 years
ago found that aging inmates have a lower rate of re-arrest than younger
inmates do. Specifically, a 1994 BOP study of inmates released in 1987
found that 15 percent of inmates age 55 and older released from its custody
were re-arrested for either a new crime or a probation violation within
3 years of release, as compared to 57 percent of inmates age 25 and
younger who were re-arrested. This study also found that 41 percent of
federal inmates of all ages were re-arrested for either a new crime or a
55
Moderate-severity misconduct incidents, which include incidents of refusing to obey
an order, refusing to work, or refusing to accept a program assignment, were the most
common level of violation for inmates of all ages.
38
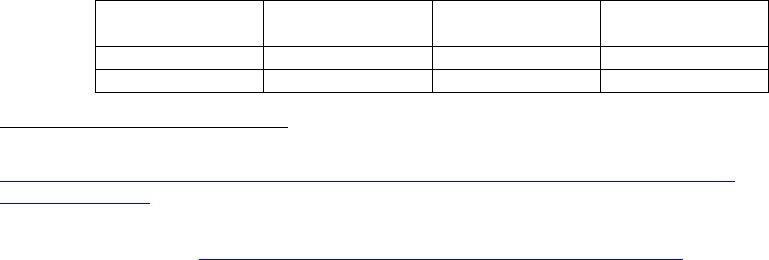

probation violation within 3 years.
56
The Department’s Bureau of Justice
Statistics (BJS) released a study in 2014 about recidivism rates for state
inmates which also showed that recidivism rates were lower for older inmates
than for younger inmates; but the study did not specifically break out
recidivism rates for inmates over age 50. The BJS studied inmates released
from 30 state correctional systems in 2005 and reported that 60 percent of
inmates age 40 and older were re-arrested for a new crime or probation
violation within 3 years, while inmates under age 30 had recidivism rates
exceeding 70 percent within 3 years (with 76 percent of released inmates
age 24 or younger re-arrested within 3 years). The BJS includes both re-
arrests for new crimes and re-arrests for probation violations, and we could
not separate the two categories.
57
In light of this absence of data on recidivism rates for aging inmates,
the OIG undertook its own analysis. The Federal Bureau of Investigation’s
(FBI) Criminal Justice Information Services Division provided us with criminal
history records of all 37,271 aging inmates who were released from BOP
custody between FY 2006 and FY 2010.
58
We based our analysis on a
randomly selected sample of 381 inmates released during this period.
We reviewed the criminal history of these 381 aging inmates and
found that 58 (15 percent) were re-arrested for new crimes within 3 years of
their release. We also found that the re-arrest of aging inmates within our
sample generally declined with age. For example, 34 of 181 released
inmates (19 percent) age 50 to 54 were re-arrested for a new crime
compared to no re-arrests for released inmates age 70 and older. See
Table 7.
Table 7
Re-Arrest Rate of Aging Inmates Released Between FY 2006 and
FY 2010
Age Cohort Total
Re-Arrested for
New Crime
Percentage
50–54
181
34
19%
55–59
99
16
16%
56
BOP, Recidivism Among Federal Prisoners Released in 1987 (August 4, 1994), p. 3,
http://www.bop.gov/resources/ research_projects/published_reports/recidivism/
oreprrecid87.pdf (accessed April 9, 2015).
57
See BJS, Recidivism of Prisoners Released in 30 States in 2005: Patterns from 2005
to 2010 (April 2014), http://www.bjs.gov/index.cfm?ty=pbdetail&iid=4987 (accessed April 9,
2015). In its report, BJS cautions against making direct comparisons between recidivism
statistics published at different times for a number of reasons, including that criminal record
histories have become more comprehensive and reliable in recent years.
58
We analyzed aging inmates released between FY 2006 and FY 2010 to ensure that
every inmate in our sample had been released for at least 3 years. See Appendix 1 for more
details.
39
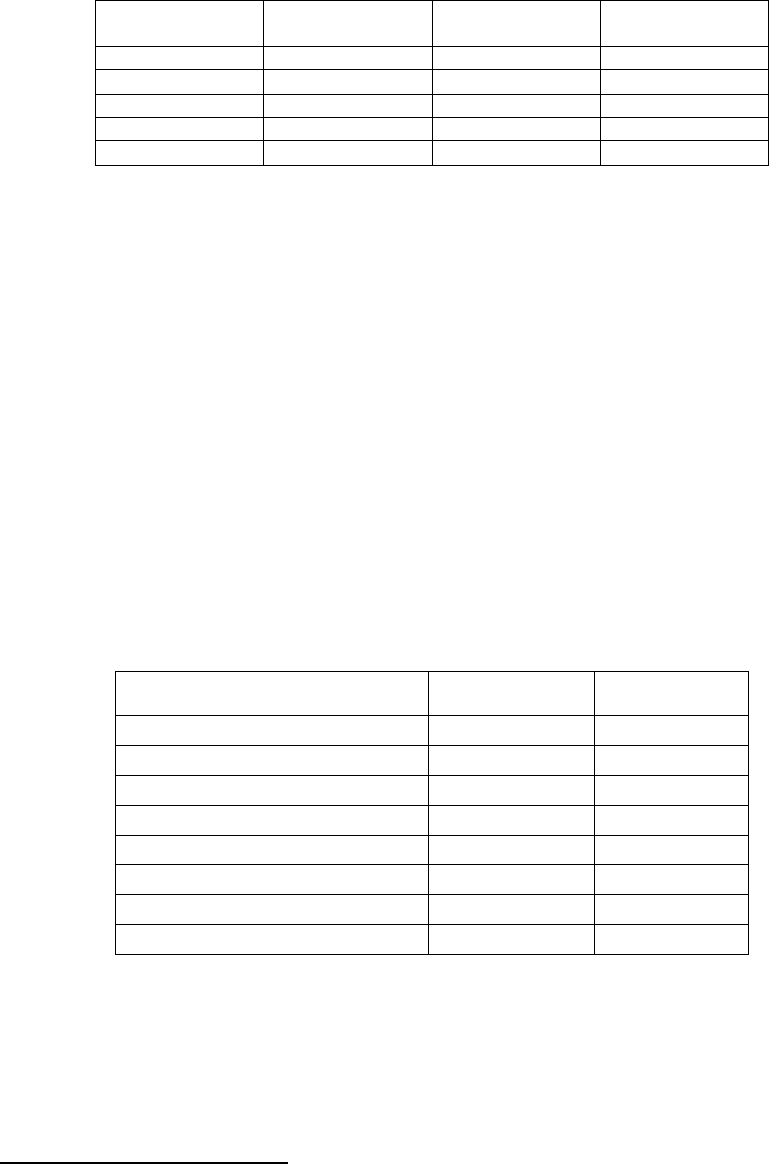

Age Cohort Total
Re-Arrested for
New Crime
Percentage
60–64
64
5
8%
65–69
27
3
11%
70–74
9
0
0%
75+
1
0
0%
Total
381
58
15%
Source: FBI data.
In addition to those who were re-arrested for new crimes, we found
that 28 of 381 aging inmates (7 percent) in our sample were re-arrested for
probation violations. In total, 23 percent of inmates age 50 and older were
re-arrested within 3 years of their release from BOP custody for either new
crimes or probation violations.
Aging inmates were most frequently re-arrested for drug offenses and for
offenses similar to those that resulted in their prior incarceration
Aging inmates who were re-arrested were most commonly charged
with drug offenses (41 percent), followed by violent offenses (17 percent)
and immigration offenses (16 percent).
59
See Table 8.
Table 8
Re-Arrest Offense of Aging Inmates
Type of Offense
Number
Re-Arrested
Percentage
Drugs
24 41%
Violent Offense
10 17%
Immigration
9 16%
Burglary/Larceny
5 9%
Miscellaneous
4 7%
Court
3 5%
Counterfeiting/Embezzlement
2 3%
Sex Offenses
1
2%
Note: Miscellaneous offenses are those that do not fit into any of the
other categories and include driving under the influence and driving
with a suspended license.
Source: FBI data.
59
Violent offenses include offenses defined in BOP, Categorization of Offenses,
Program Statement 5162.05 (March 16, 2009). Violent offenses also include simple assault,
battery, corporal injury, and robbery that are not included in Program Statement 5162.05.
See the Appendix for more details about how we categorized offenses.
40

We also found similarities between aging inmates’ criminal history and
the offenses for which they were re-arrested. On average, 45 percent of
aging inmates were re-arrested for crimes similar to those that led to their
previous incarceration. For example, 58 percent of aging inmates who were
re-arrested for drug offenses and 78 percent who were re-arrested for
immigration violations were previously incarcerated for similar crimes.
Finally, we found that only 8 of the 58 (14 percent) aging inmates in
our sample who were re-arrested had been first-time offenders at the time
they were released from the BOP. The remaining 50 aging inmates in our
sample who were re-arrested were already recidivists at the time they were
released from the BOP. Therefore, 86 percent of aging inmates in our
sample who recidivated were already known recidivists.
Aging inmates could be viable candidates for early release, resulting
in significant cost savings; but new BOP policy strictly limits those
who can be considered and as a result, few have been released
In April 2013, the OIG released a report that found significant
problems with the management of the BOP’s compassionate release
program, and that an effectively managed program would help the BOP
better manage its inmate population and result in cost savings. Among other
issues, the OIG found that the policy was being applied only to inmates with
terminal medical illnesses who had less than 12 months to live. On
August 12, 2013, the Attorney General announced expanded provisions for
inmates age 65 and older to seek compassionate release as part of the
Department’s “Smart on Crime” initiative, which was implemented to, among
other things, address concerns about unfair sentencing disparities, and
reduce overcrowded institutions.
60
That same day, the BOP revised its
compassionate release policy to expand the eligibility provisions for elderly
inmates for medical and nonmedical reasons.
61
In announcing the revised
policy, the Department said that the BOP would generally consider for
compassionate release inmates age 65 and older who had not committed
violent crimes and had served significant portions of their sentences.
60
In the Sentencing Reform Act of 1984, Congress authorized the BOP Director to
request that a federal judge reduce an inmate’s sentence for “extraordinary and compelling”
circumstances. The statute permits requests based on either medical or nonmedical reasons
that could not reasonably have been foreseen by the judge at the time of sentencing. The
BOP issued regulations and a Program Statement entitled Compassionate Release/Reduction in
Sentence: Procedures for Implementation of 18 U.S.C. § 3582(c)(1)(A) and 4205(g), Program
Statement 5050.49 (August 12, 2013), to implement this authority.
61
The program statement establishes eligibility provisions for “elderly” inmates. For
the purposes of our review, we refer to inmates who requested compassionate release under
these provisions as “aging inmates” because each provision falls within our definition of an
aging inmate.
41

Few aging inmates are eligible for early release consideration under the new
BOP policy
Following the release of our compassionate release report in 2013,
Department and BOP officials formed a working group to expand the use of
compassionate release by identifying inmates who do not present a threat to
the community and who present a minimal risk of recidivism.
62
The working
group determined that inmates age 65 and older could be appropriate
candidates for compassionate release, and the BOP revised its program
statement to include three new provisions under which these inmates could
request compassionate release. The BOP based its revisions to the
compassionate release program on provisions that had already been
established by the Violent Crime Control and Law Enforcement Act of 1994,
the United States Sentencing Guidelines, and the Second Chance Act of
2007. These provisions, however, already existed at the time of the BOP’s
earlier compassionate release policy, and none had resulted in the release of
many BOP inmates.
The first new eligibility provision applies to inmates who are age 70
and older and have served 30 years or more of their sentence for an offense
that was committed on or after November 1, 1987 (referred to as “new law”
elderly inmates).
63
Therefore, no inmate will be eligible for compassionate
release consideration under these provisions until at least November 1,
2017.
64
As a result, no inmate has yet to be released under this provision.
Moreover, we determined that just 18 inmates would likely be eligible for
consideration under this provision in the first year after November 1, 2017.
The second new eligibility provision applies to inmates:
62
DOJ, OIG, The Federal Bureau of Prisons’ Compassionate Release Program,
Evaluation and Investigations Division Report I-2013-006 (April 2013). The working group
consisted of representatives from the Office of the Attorney General, the Office of the Deputy
Attorney General, the Executive Office for United States Attorneys, the Office of Legal Policy,
three U.S. Attorneys’ Offices, and the BOP.
63
18 U.S.C. 3582(c)(1)(A)(ii) states that upon motion of the BOP Director, a federal
judge may reduce an inmate’s sentence if the inmate is age 70 or older; has served at least
30 years in prison, pursuant to a sentence imposed under 18 U.S.C. § 3559(c), for the offense
or offenses for which the defendant is currently imprisoned; and the BOP Director has
determined that the defendant is not a danger to the safety of any other person or the
community, as provided under 18 U.S.C. § 3142(g). The BOP’s provisions do not require
inmates to be serving a sentence imposed under 18 U.S.C. § 3559(c), which mandates a life
sentence for a defendant convicted of a third serious violent felony or a second serious violent
felony plus a serious drug felony. Because 18 U.S.C. § 3559(c) was passed in 1994, inmates
would not have served the minimum 30 years until 2024.
64
The BOP General Counsel said that, even though the provision would not be
effective for several years, the BOP included it when revising the program statement in 2013
so that it would not need to resubmit the program statement to the union for negotiation
shortly after it had been revised.
42

1. age 65 and older,
2. suffering from chronic or serious medical conditions related to the
aging process,
3. experiencing deteriorating mental or physical health that substantially
diminishes their ability to function in a correctional facility,
4. for whom conventional treatment promises no substantial
improvement to their mental or physical condition, and
5. who have served at least 50 percent of their sentence.
Officials with the BOP’s Office of General Counsel told us that the
Department’s working group chose 65 as the eligibility age after considering
several factors, such as when inmates become eligible for federal benefits
and how their health compares to aging individuals who are not in prison.
The working group also decided that inmates should serve a minimum of
50 percent of the sentence to justify the resources that the Department
spent to prosecute the inmate. The BOP’s General Counsel said that the
medical provisions were based on the United States Sentencing
Guidelines (USSG) definition of the term “extraordinary and compelling
reasons.”
65
However, we note that, unlike the new BOP policy, the USSG
policy statement applies to inmates of all ages, not just those age 65 and
older, and it does not require inmates to have served a minimum percentage
of their sentence. According to BOP data, as of September 2013, there were
2,204 inmates age 65 and older who had served at least 50 percent of their
sentence.
Finally, the third new eligibility provision applies to inmates without
medical conditions who are age 65 and older and who have served the
greater of 10 years or 75 percent of their sentences. The BOP’s General
Counsel told us that the provisions were based on the Elderly and Family
Reunification for Certain Non-Violent Offenders Pilot Program (pilot program)
created as part of the Second Chance Act of 2007.
66
In a report to Congress
65
The USSG defines “extraordinary and compelling reasons” to include: (1) a
terminal illness; (2) a permanent physical or medical condition, or deteriorating physical or
mental health because of the aging process, that substantially diminishes the inmate’s ability
to provide self-care and for which conventional treatment promises no substantial
improvement; (3) the death or incapacitation of the only relative capable of caring for the
inmate’s minor child; and (4) any other circumstance that the BOP Director finds to be
extraordinary and compelling. USSG § 1B1.13 (Policy Statement), Application Notes, Note 1.
66
The Second Chance Act directed the BOP to conduct the pilot program during
FYs 2009 and 2010 to determine the effectiveness of placing eligible elderly inmates on home
detention until the end of their sentences. The Act excluded inmates with a life sentence; a
history of violence, espionage, sex offenses, or acts in connection with terrorism; or a history
of escape or attempted escape. The statute also required the BOP to determine that eligible
inmates were not at substantial risk of recidivating or endangering the public.
43

after the conclusion of the pilot program in September 2010, the BOP
recommended that the pilot program not be made permanent for a number
of reasons, including that few inmates were eligible under the provisions.
67
Specifically, the BOP reported that there were relatively few inmates over the
age of 65 in its population (approximately 4,000 at that time) and that many
were already at an advanced age when they committed the crime for which
they were incarcerated. As a result, the eligibility provisions precluded
consideration of the vast majority of these inmates. The BOP reported that
71 of 855 inmates (8 percent) who requested to participate in the pilot
program were ultimately placed on home detention, while 750 inmates of the
855 inmates (88 percent) were ineligible because they did not meet the
provisions.
68
The BOP’s Central Office did not approve the transfer of the
remaining 32 inmates to home detention because the BOP determined the
inmates were a risk for recidivism or endangering the public. According to
BOP data, as of September 2013, there were 529 inmates age 65 and older
who had served the greater of 10 years or 75 percent of their sentence.
Few inmates age 65 and older were released under the new compassionate
release policy
In our 2013 review of the BOP’s compassionate release program, we
found that from 2006 through 2011, 24 inmates on average were released
from BOP custody each year.
69
Since the BOP expanded the compassionate
release program in August 2013 to include inmates age 65 and older as part
of the Department’s Smart on Crime initiative, only two inmates were
released under the new age 65 and older eligibility provisions (see Table 9).
By contrast, 83 inmates were released under the provisions in the new policy
not tied to age.
67
The report to Congress also concluded that the pilot program did not result in any
cost savings. However, the Government Accountability Office questioned the BOP’s cost
estimates, concluding that the BOP could not determine the actual cost of monitoring inmates
who were on home detention. See U.S. Government Accountability Office, Federal Bureau of
Prisons: Methods for Estimating Incarceration and Community Corrections Costs and Results
of the Elderly Offender Pilot, GAO-12-807R (July 27, 2012), pp. 2, 15–16. The BOP told us
that as of February 2013 it requires all entities bidding on contracts for halfway houses and
home detention to separate the costs of those two services.
68
Seventy-three inmates were deemed eligible for the pilot program, but two were
not placed on home detention. One inmate died before he could be placed on home detention.
The second inmate’s placement was denied because staff from community corrections and
U.S. Probation and Pre-trial Services were unable to perform the necessary home visits and
therefore unable to provide adequate supervision.
69
DOJ, OIG, The Federal Bureau of Prisons’ Compassionate Release Program.
44
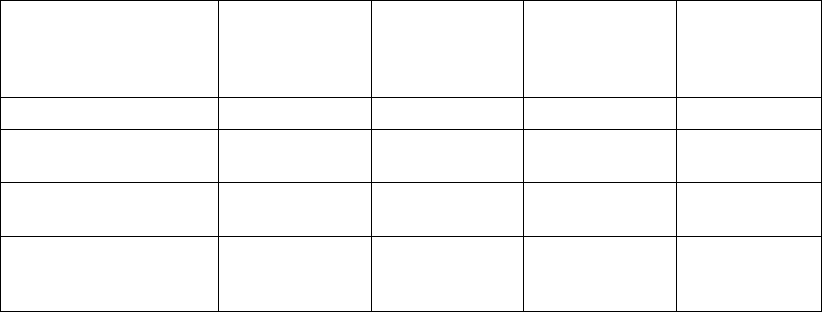
Table 9
Compassionate Release Requests,
August 12, 2013, through September 12, 2014
Requests by
Inmates
Requests
Approved by
Institutions
Requests
Approved by
the BOP
Director
Released
All Provisions
2,621
320
111
85
“New Law” Elderly
Inmates
52
12
0
0
Elderly Inmates with
Medical Conditions
203
33
0
0
Elderly Inmates
without Medical
Conditions
93
19
3
2
Notes: Included in the “All Provisions” row are requests for compassionate release
made under the three provisions available to inmates age 65 and older, as well as the
provisions available to inmates of all ages such as the provision for inmates with a
terminal or debilitating medical condition.
Some requests by inmates were still pending a decision by institutions as of
September 12, 2014. Additionally, some requests approved by institutions were still
pending a decision by the BOP’s Central Office as of September 12, 2014. Finally,
although the BOP Director can approve the requests, the sentencing court makes the
ultimate decision as to whether an inmate is released.
Source: BOP.
As shown in Table 9, since the new provisions went into effect,
inmates made 2,621 requests for compassionate release, but only
348 requests (13 percent) were made under the new eligibility provisions for
inmates age 65 and older. The remaining 2,273 requests (87 percent) were
made under eligibility provisions available to inmates of all ages, including
those with a terminal illness.
The new eligibility provisions for inmates age 65 and older are unclear
In our 2013 review of the BOP’s compassionate release program, we
found that the BOP failed to provide institution staff with adequate guidance
regarding appropriate requests for compassionate release. As part of this
review, BOP officials and staff told us that the eligibility provisions for
inmates age 65 and older are unclear. For example, the BOP’s revised
program statement includes eligibility for an inmate age 65 and older under
the medical or nonmedical provisions. However, institution staff said that
determining whether an inmate age 65 and older qualifies under the medical
or nonmedical provisions is difficult. The BOP’s Assistant Director for Health
Services and Medical Director, who told us he was not consulted on the
development of the provisions, including the medical provisions, described
45
the provisions as “vague.” The BOP’s General Counsel told us that the BOP is
aware of the need to include more clarification regarding the different
medical provisions. The BOP held in-person training for all institution-level
compassionate release coordinators in December 2014 to answer the
coordinators’ questions and better ensure consistent implementation of the
program statement across institutions. The BOP also issued an Operations
Memorandum in March 2015 that provided more-specific examples of medical
conditions and problems with activities of daily living that make an aging
inmate eligible for compassionate release under the medical provisions.
Institution staff also found the nonmedical eligibility provision
confusing. The program statement says that inmates age 65 and older
without medical conditions must serve the greater of 10 years or 75 percent
of their sentence to be eligible to apply for compassionate release. A Case
Manager told us that when he contacted the BOP’s Office of General Counsel
to clarify the provision, he was told that the Office of General Counsel
interprets the provision to mean an inmate must serve both a minimum of 10
years and 75 percent of the sentence. As a result, only elderly inmates who
receive sentences in excess of 10 years are eligible to seek early release
under this provision. The BOP’s General Counsel confirmed that this is the
BOP’s interpretation of the provision and told us that while the BOP received
a lot of questions regarding this provision when the program statement was
first released and that it does need to be clarified, the BOP has not discussed
making any changes to the program statement itself.
In general, BOP officials and staff we interviewed did not believe that
the existing aging inmate provisions would significantly reduce the size of the
BOP’s aging inmate population. For example, a Warden told us that laws and
policies are sometimes written with good intentions; but if policymakers do
not do the homework in advance, the result will be a policy that sounds good
but does not accomplish much. He added, “I think that’s what this [the
aging inmate provisions] is going to pan out to be too. There is always a thin
line between being compassionate to the elderly and protecting society.
When you have that thin line, you normally write in provisions that start
excluding a lot of people from consideration.”
The BOP’s compassionate release program could be more effective in
assisting the BOP in managing its aging inmates, which would result in
significant cost savings
In announcing the Smart on Crime initiative, the Attorney General
stated that revisions to the BOP’s compassionate release policy would help
the Department use its limited resources to incarcerate those who pose the
greatest threat. As we outlined previously, aging inmates commit fewer and
less-severe misconduct incidents while incarcerated than do younger inmates
and have a lower rate of re-arrest once released. The BOP General Counsel
told us that the Department’s working group to expand the use of
46

compassionate release concluded that aging inmates do not pose a
significant public safety threat.
We found that the BOP’s compassionate release program could have a
greater impact on overcrowding and incarceration costs if the BOP revised
the inmate age provisions to align with the NIC’s recommended definition of
an “aging” inmate as age 50 or above. We found that the BOP does not
define the term “aging” or “elderly” inmate.
70
Rather, as stated above, the
BOP requires inmates to be at least 65 years old to request compassionate
release under the new provisions. However, the NIC, a Department agency
within the BOP, has recommended since 1992 that correctional agencies
nationwide define aging inmates as starting at age 50.
71
The NIC based its
recommendation on aging inmates’ pre-incarceration lifestyles and limited
pre-incarceration access to medical care, two factors BOP institution staff
commonly cited to us when they described their own views of aging inmates.
The NIC continued to recommend that correctional agencies define aging
inmates starting at age 50 in a 2010 online training seminar concerning the
management of aging inmates.
72
Our analysis of BOP data shows that if the BOP revised the age
provisions in its compassionate release policy from age 65 and older to age
50 and older, consistent with the NIC’s recommendation, the potential pool
of candidates for compassionate release would increase more than sevenfold,
from 4,384 inmates age 65 and older to 30,962 inmates age 50 and older,
based on FY 2013 population data. Our analysis also shows that the current
age provision of 65 and older will not enable the BOP to effectively address
its overcrowding issues in BOP institutions because that age group, while
growing, constitutes only 3 percent of the BOP’s total inmate population.
We found that lowering the eligibility provision to age 50 and older
could assist the BOP in addressing its overcrowding issues, particularly in its
minimum- and low-security institutions where more aging inmates are
incarcerated. For example, at the end of FY 2013, BOP minimum- and low-
security institutions had a population of 71,679 inmates and were operating
at 27 percent over capacity. In order to eliminate over-capacity in these
70
When we asked BOP staff how they defined these terms, their responses ranged
from age 40 to age 78.
71
DOJ, NIC, An Administrative Overview of the Older Inmate (1992). The NIC
provides training, technical assistance, information services, and policy and program
development assistance to federal, state, and local correctional agencies. The NIC also
provides leadership to influence correctional policies, practices, and operations nationwide in
areas of emerging interest and concern to correctional executives and practitioners as well as
public policymakers.
72
See DOJ, NIC, Effectively Managing Aging and Geriatric Offenders,
Satellite/Internet Broadcast, March 11, 2010, http://nicic.gov/library/024363 (accessed
April 9, 2015). However, we note that, while the NIC is part of the BOP, no BOP employees
participated in the broadcast.
47

institutions, the BOP would have to reduce its minimum- and low-security
population by about 15,000 inmates. We found that inmates age 65 and
older represented only 4 percent (2,755 inmates) of the BOP’s minimum- and
low-security inmate population, whereas inmates age 50 and older represent
24 percent (17,482 inmates) of the BOP’s total minimum- and low-security
inmate population. If a modest 5 percent (874 of 17,482 inmates) of this
larger group of aging inmates was determined to be appropriate for
compassionate release and were released from BOP custody, the BOP could
reduce overcrowding in its minimum- and low-security institutions by
2 percent.
73
In comparison, the BOP would have to release 32 percent of
minimum- and low-security inmates age 65 and older (874 of 2,755) to
reduce overcrowding in its minimum- and low-security institutions by the
same amount.
Based on BOP cost data, we estimate that the BOP spent
approximately $881 million, or 19 percent of its total budget, to incarcerate
aging inmates in FY 2013.
74
We found that lowering the threshold age from
age 65 to age 50 in the revised compassionate release program, coupled
with a modest 5 percent release rate for only those aging inmates in
minimum- or low-security institutions or medical centers, could reduce
incarceration costs by approximately $28 million per year. Specifically, we
estimate that it cost the BOP approximately $438 million to incarcerate
inmates age 50 and older in minimum- and low-security institutions in
FY 2013. The early release of 5 percent (874) of these inmates could save
the BOP over $21 million in incarceration costs per year. Also, as previously
noted, aging inmates represent one-third of the population at the BOP’s six
medical centers, which, at $59,000 per inmate per year, are the BOP’s
highest-cost institutions. If 5 percent of aging inmates housed in the BOP’s
medical centers (112 of 2,246 inmates) were released, the BOP could
potentially save an additional $7 million in 1 year.
75
Finally, we found that revising the time-served provision in the new
compassionate release program statement for inmates age 65 and older
without medical conditions would also increase the potential pool of
candidates for compassionate release. The BOP’s eligibility provisions for
these inmates require them to serve the greater of 10 years or 75 percent of
their sentence. As noted above, the BOP’s Office of General Counsel
73
For this analysis, we considered only the age of the inmates, not the percentage of
sentence served.
74
Using BOP population snapshots and per capita costs, we calculated the costs of
BOP’s aging inmates based on the number of days served within a fiscal year and designated
institution security level. For more information, see Appendix 1.
75
We did not consider the cost impact of compassionate release for aging inmates at
medium- and high-security institutions because aging inmates represent a smaller portion of
the population at those security levels and their potential release would have less of an impact
on overcrowding.
48

interprets these provisions to mean that an inmate must have served both
10 years and at least 75 percent of his or her sentence. We found this
provision excludes almost half of the BOP’s aging inmate population because
many sentences are too short for the inmate to be eligible for compassionate
release. In FY 2013, this policy excluded from consideration 45 percent of
the 4,384 BOP inmates who were age 65 and older because they were
serving sentences of 10 years or less.
76
We have concerns because
Department leadership says the compassionate release policy is designed to
address prison overcrowding by providing for early release of aging inmates
who did not commit violent crimes and who pose no threat to public safety.
Yet this policy as written prohibits early release consideration for nearly half
of the BOP’s aging inmate population who are likely to be the best candidates
for early release. These ineligible inmates who received a shorter sentence
are more likely to have committed a less serious offense, and present less
danger to the public, than those inmates who are eligible because they
received sentences of imprisonment in excess of 10 years.
We believe the BOP should consider whether to revise this provision to
eliminate the 10-year minimum time served requirement so that all of the
BOP’s aging inmates could be eligible for compassionate release
consideration once they had served 75 percent of their sentences, including
those aging inmates who committed less serious crimes and received shorter
sentences and therefore may be most worthy of early release consideration.
The BOP’s General Counsel told us that these provisions might be “really
limiting” and that it may be better if inmates just met one of the time served
requirements.
77
We note that not all aging inmates age 50 and older will be
appropriate for compassionate release. For each compassionate release
request, the BOP evaluates many other factors, including the nature and
circumstances of the inmate’s offense, criminal history, the inmate’s release
plans, and whether release would minimize the severity of the punishment.
Nonetheless, the BOP has already determined that aging inmates are a low
public safety risk. We believe that reevaluating the compassionate release
eligibility provisions for aging inmates could substantially increase the pool of
eligible inmates. Within that larger pool of eligible aging inmates, we believe
the BOP could further identify more aging inmates whose offenses, criminal
histories, and release plans also make them suitable candidates for
76
Moreover, because inmates are eligible to earn good conduct time credit under
18 U.S.C. § 3624(b), which equates to about 87 percent of their sentences under BOP policy,
elderly inmates who earned all of their good conduct time credit (and therefore would likely be
the best candidates for early release) would need to be serving a sentence in excess of
11 years in order to actually serve at least 10 years in prison. Due to good time credit, we
found that 48 percent of BOP inmates age 65 and older were likely to be released before they
had served 10 years in prison.
77
The BOP’s General Counsel also said that any changes to the eligibility criteria
would require coordination with the Department and then negotiations with the BOP’s union.
49

compassionate release, resulting in reduced overcrowding and additional cost
savings to the BOP.
50
CONCLUSION AND RECOMMENDATIONS
We concluded that a growing aging inmate population has an adverse
impact on the BOP’s ability to provide a safe, humane, cost-efficient, and
appropriately secure environment for aging inmates and to assist aging
inmates reentering the community. Although the BOP has revised its
compassionate release policy to expand consideration for early release to
aging inmates, which could help mitigate the effects of a growing aging
inmate population, few aging inmates have been released under it. Several
aspects of the BOP’s inmate management, including costs, housing, and
programming, are affected by an aging inmate population that is growing
more quickly than the rest of the BOP’s inmate population.
First, aging inmates are more costly to incarcerate than their younger
counterparts. According to our analysis of BOP data, an aging inmate costs
8 percent more to incarcerate than a younger inmate due in large part to
increased medical needs. Further, aging inmates represent one-third of the
population at the BOP’s six medical centers, which at $59,000 per inmate per
year are the BOP’s highest-cost institutions. In FY 2013, the BOP spent
$1.1 billion of its $6.5 billion budget (17 percent) on health services. In that
same year, institutions with the highest percentage of aging inmates spent
an average of $10,114 per inmate on medical costs, while institutions with
the lowest percentage of aging inmates spent an average of $1,916 per
inmate. The continuing increase in the aging inmate population will drive
even greater increases in medical spending, especially at institutions with the
highest percentages of aging inmates.
Second, BOP institutions lack appropriate staffing levels and offer
limited training to address the needs of an aging inmate population. Some
institutions have established local inmate companion programs to assist
aging inmates with the activities of daily living. However, we found that
these programs lack consistent oversight and that implementation varies by
institution. We believe the BOP should develop a standardized program to
ensure consistency in the implementation of the companion program, as well
as set clear program expectations for companions in order to reduce the risk
of victimization of aging inmates. We also believe the BOP should implement
more training to help staff recognize and respond to the signs of aging. If
institution staff is appropriately trained, the inmates’ underlying medical
needs could be met with care instead of disciplinary action.
Third, the BOP cannot sufficiently house aging inmates at all
institutions because of limitations in physical infrastructure. Specifically,
overcrowding of BOP institutions results in an inadequate number of lower
bunks needed to accommodate aging inmates with limited mobility.
Overcrowding also restricts the BOP’s ability to move aging inmates to
institutions, including its medical centers, that can best address aging
inmates’ medical needs. Institutions, including those with higher care levels
or a high percentage of aging inmates, lack sufficient handicapped-accessible
51
cells and bathrooms and have difficulty accommodating the number of
inmates who need elevators. As a result, aging inmates may be placed in
compromising and sometimes unsafe situations due to limitations in
institutions’ physical infrastructure. The BOP has not evaluated all
institutions’ accessibility for inmates with mobility impairments since 1996.
We believe that, due to the growing aging inmate population, the BOP should
reexamine the accessibility of all of its institutions to accommodate the large
number of aging inmates with mobility needs. BOP staff and officials told us
that separate units, or entire institutions, might be more appropriate to
house aging inmates. Units designated specifically for aging inmates,
supplemented with medical staff, could help the BOP provide aging inmates
more efficient medical care, as well as identify unique programming needs.
Fourth, the programming opportunities to help aging inmates reenter
the community are inadequate. There are no standardized programs
specifically designed for aging inmates. While institutions have the flexibility
to create local programs or activities to address the needs of their
population, few have such programs or activities for aging inmates, including
those institutions with high percentages of such inmates. As a result, aging
inmates either participate in programs that may not meet their needs or are
left idle, not participating in any activities. The BOP’s release preparation
program does not address the unique release needs of aging inmates,
including those aging inmates who do not plan to seek employment after
release or require assistance with continuity of medical care. The BOP should
consider developing programs specifically tailored for aging inmates and
enhance its release preparation program to address the unique needs
commonly associated with the release of aging inmates.
Fifth, many aging inmates could be viable candidates for early release.
We found that aging inmates have fewer misconduct incidents while
incarcerated and a lower rate of re-arrest after release. Our analysis
concluded that aging inmates comprised 10 percent of all BOP misconduct
incidents in FY 2013, while accounting for 19 percent of the entire
population. Based on our research and discussions with BOP officials and
staff, we consider the rate of misconduct by aging inmates during
incarceration to be relatively low compared to younger inmates. In addition,
we found that only 15 percent of a sample of aging inmates released from
BOP custody was re-arrested for a new crime within 3 years. Based on
studies by the BOP and the BJS, we also consider the rate of re-arrest for
aging inmates to be relatively low compared to the re-arrest rates of younger
inmates. Therefore, while individual cases will vary, aging inmates are
generally less of a threat during incarceration and less likely to be a threat to
society once released.
Finally, we found that the BOP’s revised eligibility provisions for
inmates age 65 and older to request compassionate release have not been
effective in achieving the Department’s goals. In August 2013, the Attorney
General announced expanded provisions for inmates age 65 and older to
52
seek compassionate release as part of the Department’s Smart on Crime
initiative. While a Department working group determined that inmates age
65 and older could be appropriate candidates for compassionate release, and
the BOP revised its program statement to include three new provisions under
which these inmates could apply, these provisions are based on existing
statutes, which previously resulted in few inmates released from BOP
custody. Because of the limitations in the revised provisions, we found that
only two aging inmates have been released since the BOP revised the
compassionate release policy. While we found that the BOP’s eligibility
provisions for aging inmates to request compassionate release are currently
ineffective, our analysis shows that the BOP could more fully achieve the
outcomes the Department seeks by using its existing authority to further
revise its eligibility provisions. Expanding the eligibility provisions, such as
lowering the age requirement to age 50 and revising the time served
provisions for those aging inmates without a medical condition, would
increase the pool of potential candidates for compassionate release and
further assist the BOP in reducing overcrowding and could save the
Department millions of dollars.
Recommendations
To ensure the BOP continues to provide safe, humane, and cost-
efficient care within its institutions and to further assist the BOP in managing
its aging inmate population, reducing overcrowding, and reducing
incarceration costs, we recommend that the BOP:
1. Develop national guidelines for the availability and purpose of inmate
companion programs.
2. Consider the feasibility of placing additional Social Workers in more
institutions, particularly those with larger populations of aging
inmates.
3. Provide all staff training to identify signs of aging and assist in
communicating with aging inmates.
4. Reexamine the accessibility and the physical infrastructure of all of its
institutions to accommodate the large number of aging inmates with
mobility needs.
5. Study the feasibility of creating units, institutions, or other structures
specifically for aging inmates in those institutions with high
concentrations of aging inmates.
6. Systematically identify programming needs of aging inmates and
develop programs and activities to meet those needs.
53
7. Develop sections in release preparation courses that address the post-
incarceration medical care and retirement needs of aging inmates.
8. Consider revising its compassionate release policy to facilitate the
release of appropriate aging inmates, including by lowering the age
requirement and eliminating the minimum 10 years served
requirement.
54

APPENDIX 1: EXPANDED METHODOLOGY
Data Analysis
Medical Spending by Institution
The BOP provided total medical obligations for all BOP-operated
institutions from fiscal year (FY) 2009 to 2013. To calculate each institution’s
medical rate per inmate, we used the population data obtained from the
BOP’s SENTRY case management system.
78
We then divided the medical
obligations by the total population at each institution to determine the
average annual medical rate per inmate.
We compared the medical rates per inmate of institutions with the
highest and lowest percentage of aging inmates. Medical centers were
excluded from our analysis because their populations tend to have higher
medical rates for inmates of all ages. Detention centers were excluded
because the population data sets do not include pre-trial inmates. Last, we
also excluded correctional complexes because medical spending was only
reported for the complex as a whole, not for each institution within it.
Therefore, we could not determine which institution within a complex was
influencing overall medical costs.
Medical Spending Inside and Outside the Institution
The BOP provided data on medical obligations inside and outside the
institutions, including medical airlifts, public health service obligations, and
unforeseen medical services that, when combined, totaled the BOP’s entire
medical obligations. The OIG analyzed only medical obligations for expenses
incurred inside and outside the institutions. We sorted the sub-object codes
based on expenses inside or outside the institution to determine which codes
had the highest rates of spending. We excluded sub-object codes such as
administrative pay, Federal Health Benefits, and Retirement, and analyzed
codes such as contract services, pharmaceuticals, medical hospital services,
overtime, and night differential.
79
We analyzed the sub-object codes with
high rates of spending at the institutions with the highest and lowest
78
SENTRY is the BOP’s primary mission support database. The system collects,
maintains, and tracks critical inmate information, including inmate location, medical history,
behavior history, and release data. Inmate deaths are also entered into SENTRY, but there is
no code to determine whether deceased inmates were awaiting compassionate release
consideration.
79
A night differential is compensated payment above the basic rate for regularly
scheduled night work as a non-wage employee. These costs were incurred outside the
institution for matters such as escorting inmates to medical appointments and guarding
inmates at local hospitals.
55

percentage of aging inmates. When comparing institutions based on its
percentage of aging inmates, as explained above, we excluded detention
centers, medical centers, and all federal correctional complexes.
The BOP’s Catastrophic Cases
The BOP provided national data on catastrophic care costs incurred by
each of the six regions from FY 2009 to 2013. We received data for all six
regions, however data from five of the regions was too inconsistent to
analyze. Three regions did not consistently provide the BOP register number
of inmates who received care from FY 2009 to FY 2013. Without a register
number, inmate age could not be determined. One region did not
consistently report data from medical centers, and the other region did not
report data until FY 2012, with the most consistent data in FY 2013. The
data we received was also incomplete until FY 2012 and could not be
analyzed for trends. Therefore, we isolated one region to determine the
impact of catastrophic cases on the BOP’s medical obligations and there was
no margin for comparison.
Using the BOP register number provided in each inmate’s catastrophic
case and the population snapshots provided by the BOP, we determined each
inmate’s age. If age was not available in the snapshot, we used the register
number to search for the inmate in the BOP’s inmate locator and calculated
age depending on the fiscal year during which the inmate received care.
80
Once inmates were categorized by age, we grouped the data in 5-year age
increments (under 24, 25–29, . . . 80+), and then into the two broader
categories “under 50” and “50 and above.” Using these categories, we
calculated the costs of catastrophic cases for each fiscal year.
Total Costs and Average Cost by Age Cohort
The BOP provided snapshots of its populations near the end of each
fiscal year from 2009 to 2013: FY 2009 – September 28, 2009; FY 2010 –
September 25, 2010; FY 2011 – September 23, 2011; FY 2012 –
September 28, 2012; and FY 2013 – September 28, 2013. The population
for each fiscal year represents the number of inmates incarcerated at the
time of the snapshot dates. The snapshots included an inmate’s register
number, name, age, sex, date of birth, citizenship, nature of offense,
criminal history points, sentence start date, sentence length, pre-release
date, security level, institution location, institution start date, public safety
variables, and management variables.
81
The BOP also provided daily and
annual costs for each security classification for each fiscal year. The
80
The BOP’s Inmate Locator can be found here: http://www.bop.gov/inmateloc/.
81
When we discuss inmates with no criminal history in the Background section of this
report, we are referring to inmates who have zero criminal history points.
56
documents provided the average cost of an inmate at each security
classification, which we used to calculate our cost estimates.
Since the snapshots represented the population only as of that date, it
did not include inmates who were either released prior to or incarcerated
after the snapshot date. For example, the FY 2010 snapshot would not have
included an inmate who was released prior to September 25, 2010, or an
inmate who had entered the BOP after September 25, 2010. To improve our
estimates by including those who have served before and after the snapshot
dates, we combined inmates from the snapshots of other fiscal years into the
snapshot we were analyzing. For example, for FY 2010, we used the prior
fiscal year snapshot (FY 2009) to add all inmates released prior to
September 25, 2010, into our FY 2010 estimates. Also, we used the
preceding fiscal year snapshot (FY 2011) to include inmates with a sentence
start date after September 25, 2010, but before October 1, 2010, for our
FY 2010 estimates. We included both of these additions to include all
inmates who served at least portion of their sentence in FY 2010 but were
not included in the original FY 2010 snapshot. All duplicates in a snapshot
were deleted. However, since we did not request snapshots from FY 2008
and FY 2014, we could not include inmates who may have been incarcerated
prior to or after the snapshots for FY 2009 and FY 2013.
To determine the total cost and average cost based on age and
institution security classification, we used the eight per capita cost categories
reported by the BOP each year: high, medium, low, minimum,
administrative, complex, detention center, and medical center. Each inmate
was assigned the cost category for the institution where he or she was
incarcerated at the time of the snapshot. Further, we designated minimum-
security inmates incarcerated in the minimum security camps attached to
standalone institutions (not part of a complex) as minimum security. We
then calculated the number of days served for each inmate within each fiscal
year using the institution start date and the last day of the fiscal year. If an
inmate is projected to be released prior to the end of the fiscal year, we used
the projected release date instead. Because a small percentage (less than
2 percent) did not include an institution start date but were designated to an
institution, we used the sentence start date as a substitute. We multiplied
the number of days served for each inmate by the average daily cost based
on security classifications provided by the BOP to find the cost of each
inmate.
To calculate average cost by age, we grouped inmates based on age
cohorts: under 24, 25–29, 30–34 . . . 75–79, and 80 and older. We then
added the cost for each inmate within each age cohort to find the total cost.
We divided the total cost in each age cohort by the total number of inmates
in each age cohort to find the average cost. We followed similar procedures
to find total and average cost at each security classification.
57

Recidivism of Aging Inmates
We received data from the FBI of all 36,682 federal inmates age 50
and older released from BOP institutions from FY 2006 through FY 2010. The
data included any reported arrest from any jurisdiction until the end of
FY 2013. From the 36,682 inmates in the data set, we chose a random
sample of 381 inmates. The sample size was selected by using a confidence
level of 95 percent and a margin of error of 5 percent. For each inmate in
our sample, we reviewed the criminal history and considered a recidivist any
inmate who was re-arrested for a new crime within 3 years after release. We
separately counted the number of these inmates who were re-arrested for a
probation or parole violation.
For inmates re-arrested for a new crime, we categorized their re-arrest
offense based on the description provided in the criminal history. With the
exception of the violent offense category, we used the offense categories in
SENTRY. Our violent offense category includes offenses that fit under the
BOP’s homicide/aggravated assault category, as well as offenses like simple
assault, battery, robbery, and corporal injury due to the use of force on a
victim.
Interviews
We conducted 169 interviews during this review. We interviewed
Central Office officials, including the Assistant Directors responsible for eight
Central Office Divisions; the Director of the Office of Research and
Evaluation; a Senior Counsel in the Office of General Counsel; five staff
responsible for overseeing construction and maintenance of BOP institutions;
seven staff responsible for the BOP budget; the Chief of the Designation and
Sentence Computation Center; a Medical Designator in the Office of Medical
Designations and Transportation; and a Deputy Chief in the Industries,
Education, and Vocational Training Division.
82
We visited eight institutions in person, and another five via video
teleconference, for a total of 13 institutions. During those visits, we
interviewed 10 Wardens, 5 Associate Wardens, 7 Health Services
Administrators, 4 Assistant Health Services Administrators, 4 Clinical
Directors, 1 Director of Nursing, 1 Chief of Psychology, 1 Chief Social Worker,
6 Social Workers, 7 Supervisors of Education, 2 Assistant Supervisors of
Education, 1 Reentry Affairs Coordinator, 4 Case Management Coordinators,
1 Deputy Case Management Coordinator, 5 Unit Managers, 23 Case
82
We interviewed the Assistant Directors of the Administration; Human Resource
Management; Health Services; Information, Policy, and Public Affairs; Reentry Services;
Correctional Programs; and Industries, Education and Vocational Training Divisions, as well as
the General Counsel. We did not interview the Assistant Director of the Program Review
Division or the Acting Assistant Director of the National Institute of Corrections.
58
Managers, and 23 Counselors. We also interviewed 6 inmates per institution
at the 8 institutions we visited in person, totaling 48 inmates.
Site Visits
The team conducted site visits to eight institutions: Federal
Correctional Institution (FCI) Butner Low, FCI Butner Medium I and Camp,
Federal Medical Center (FMC) Butner, United States Penitentiary (USP)
Hazelton, FCI Morgantown, FCI Cumberland, Federal Detention Center (FDC)
Philadelphia, and Metropolitan Correctional Center (MCC) New York. We
selected the Butner institutions because they had the highest percentage of
aging inmates in the BOP. We selected USP Hazelton, FCI Morgantown, and
FCI Cumberland because the institutions follow the same growing aging
inmate trend and to interview officials, staff, and inmates at every security
level. Last, the team visited two detention centers, FDC Philadelphia and
MCC New York, to assess the effects the aging inmate trend has on the BOP’s
detention centers.
Inmate Interview Selection
During our site visits, the team interviewed inmates who were
randomly selected based only on our definition of aging inmates as age 50
and older. The BOP provided a snapshot of all inmates age 50 and older at
the end of FY 2013, which the team used to randomly select inmates. If an
inmate was not available at the time of the interview, the team substituted a
different inmate from a backup list that was also randomly selected.
Video Teleconferences
The team conducted video teleconferencing with five institutions:
FCI Fort Worth, FMC Lexington, FMC Carswell, Federal Correctional Complex
Forrest City, and FCI Seagoville. We selected these five institutions because
they had a combination of a high number and a high percentage of aging
inmates in their populations, excluding FCI Butner Low and FMC Butner, in
FY 2013.
59

APPENDIX 2:
THE BOP’S RESPONSE TO THE DRAFT REPORT
60
U.S.
Deparhnent of
Justice
Federal
Bureau
of
Prisons
Washington,
DC
20534
Apri]-
27,
2015
Office o/tlle Director
MEMORANDUM
FOR
NINA
S.
PELLETIER
ASSISTANT
INSPECTOR
GENERAL
EVALUATION
AND
INSPECTION
FROM:
Direct
lJiJ<b1S~
or
Federal
Bureau
of
Prisons
SUBJECT:
Response
to
the
Office
of
Inspector
General's
(OIG)
Draft
Audi
t
Report:
Review
of
the
Impact
of
an
Aging
Inmate
Population
on
the
Federal
Bureau
of
Prisons,
Assignment
Number
A-2013-008
The
Bureau
of
p!,isons
(Bureau)
appreciates
the
opportunity
to
respond
to
the
open
recommendations
from
the
draft
report
entitled,
Review
of
the
Impact
of
an
Aging
Inmate
.
Population
on
the
Federal
Bureau
of
Prisons.
Please
find
the
Bureau's
response
to
the
recommendations
below:
Recommendation
#1:
Develop
national
guidelines
for
the
availability
and
purpose
of
inmate
companion
programs.
Initial
Response:
The
Bureau
agrees
with
the
recommendation
and
will
establish
national
inmate
companion
guidelines
.
Recommendation
#2:
Consider
the
feasibility
of
placing
additional
Social
Workers
in
more
institutions,
particularly
those
with
larger
populations
of
aging
inmates.

Initial
Response:
The
Bureau
agrees
with
the
recommendation
and
has
requested
funding
and
will
initiate
the
action
once
funding
is
received
.
We
request
this
recommendation
be
closed.
Recommendation
#3:
Provide
all
staff
training
to
identify
signs
of
aging
and
assist
in
communicating
w~th
aging
inmates.
Initial
Response
: The
Bureau
agrees
with
the
recommendation.
'I'he
Bureau's
Learning
and
Career
Development
Branch
will
work
with
the
Health
Services
Division
to
deve
l
op
curriculum
to
te~ch
employees
to
identify
signs
of
aging
and
assist
in
communica-t.
ing
with
aging
inmates.
Recommendation
*4 :
Reexamine
the
a~cessibility
and
the
physical
inf~astructure
of
all
of
its
i
nstitutions
to
accommodate
the
large
number
of
aging
inmates
with
mobility
needs.
Initial
Response:
The
Bureau
agrees
with
the
recommendation
to
examine
the
accessibility
and
physical
infrastructure
of
its
institutions
to
gather
baseline
information
to
help
inform
the
goals
of
the
multi
division
task
force
as
discussed
below
in
the
Bu~eau's
response
to
recommendation
#5.
The
Bureau
will
survey
a
ll
institutions
to
gather
information
on
current
accessibility
such
as
:
the
numbers
of
handicap
accessible
cells,
showers,
toi
l
ets,
and
other
infrastructure
issues
affecting
inmates
with
mobi
li
ty
needs.
Recommendation
IS:
Study
the
feasibi
li
ty
of
creating
units,
institutions,
or
other
structures
specifical
l y
for
aging
inmates
in
those
institutions
with
high
concentrations
of
aging
inmates.
Initial
Response:
The
Bureau
agrees
with
the
recommendation.
The
Bureau
will
create
a
mUlti-
d
ivision
tas
k
force
to
study
the
feasibility
of
creating
units
specifically
for
aging
inmates
in
those
institutions
with
high
concentrations
of
agi
ng
inmates.
Recommendation
#6:
Systematica
l
ly
ide
nt
ify
programming
needs
of
aging
inmates
and
develop
programs
and
activities
to
meet
those
needs.
Initial
Response
: The
Bureau
agrees
with
t he
recommendation
and
will
identify
programming
needs
of
aging
inmates
and
deve
l
op
programs
and
activities
to
meet
those
needs
.
As
prog
ra
m
needs
are
identified
and
new
programs
developed,
these
programs
will
be
i
ncorporated
into
the
Bureau
' s
Inmate
Mode
l
Programs
Catalog
or
nationa
l
policy.
2
61

ReCommendation
17
: Dev:elop
sections
in
release
preparation
courses
that
address
the
post-incarceration
m
ed
ic
al
care
and
retirement
needs
of
aging
inmates.
Znitial
Response
:
The
Bureau
agrees
with
the
recommendation.
The
Bureau
will
identify
and
develop
programs
which
will
assist
a
ging
inmates
as
they
transition
back
to
the
community
.
Recommendation
18;
Consider
revising
its
compassionate
rele
a
se
policy
to
facilitate
the
release
of
appropriate
aging
inmates,
including
by
lowering
the
age
requirement
and
eliminating
the
minimwn
10
years
served
requirement.
Initial
Response:
The.
Bureau
agrees
that
the
criteria
concerning
elderly
offenders
should
be
further
considered
and
eva
l
uated
before
any
final
determinations
are
made.
The
Bureau
intends
to
raise
the
issue
with
relevant
stakeholders
for
further
discussion,
and
in
relation
to
any
fut
u
re
updates
made
to
the
r e
levant
policy
statement.
As
the
recommendation
only
calls
for
the
consideration
of
new
cr
i
teria
(rath
er
than
the
adoption
of
new
standards),
we
request
this
recommendation
be
closed
.
If
you
have
any
questions
regarding
this
response,
please
contact
Sara
M.
Revell,
Assistant
Director
,
Program
Review
Division,
at
(202)
353
-
2302
.
3
62

APPENDIX 3: OIG ANALYSIS OF THE BOP’S RESPONSE
The Office of the Inspector General (OIG) provided a draft of this
report to the Federal Bureau of Prisons (BOP) for comment. The BOP’s
response is included in Appendix 2. The OIG analysis of the BOP’s response
and actions necessary to close the recommendations are discussed below.
Recommendation 1: Develop national guidelines for the availability and
purpose of inmate companion programs.
Status: Resolved.
BOP Response: The BOP concurred with the recommendation,
stating that it will develop national inmate companion guidelines.
OIG Analysis: The BOP’s actions are responsive to the
recommendation. Please provide a copy of the national inmate companion
guidelines, including guidance describing how inmate companions will be
selected, trained, paid, and overseen by institution staff, by July 31, 2015.
Recommendation 2: Consider the feasibility of placing additional Social
Workers in more institutions, particularly those with larger populations of
aging inmates.
Status: Resolved.
BOP Response: The BOP concurred with the recommendation,
stating that it had requested additional funding and would initiate further
action upon receipt of that funding.
OIG Analysis: The BOP’s actions are responsive to the
recommendation. Please provide information about the number of Social
Workers to be hired, their institution placement, and information about how
the BOP factored the aging inmate population into its decisions about which
institutions should receive additional Social Workers, by July 31, 2015.
Recommendation 3: Provide all staff training to identify signs of aging and
assist in communicating with aging inmates.
Status: Resolved.
BOP Response: The BOP concurred with the recommendation,
stating that the Health Services Division and the Learning and Career
Development Branch would jointly develop a training curriculum to teach
employees to identify signs of aging and assist in communicating with aging
inmates.
63

OIG Analysis: The BOP’s actions are responsive to the
recommendation. Please provide a copy of the training materials provided to
BOP staff and a description of how training was implemented by July 31,
2015.
Recommendation 4: Reexamine the accessibility and the physical
infrastructure of all of its institutions to accommodate the large number of
aging inmates with mobility needs.
Status: Resolved.
BOP Response: The BOP concurred with the recommendation,
stating that it would survey all institutions to gather information on current
accessibility, such as the number of handicapped-accessible cells, showers,
toilets, and other infrastructure issues affecting inmates with mobility needs.
The BOP further stated that it will use the baseline information gathered in
the survey to inform the goals of a multi-division task force that will study
the feasibility of creating units for aging inmates (see the BOP’s response to
Recommendation 5).
OIG Analysis: The BOP’s actions are responsive to the
recommendation. Please provide the results of the BOP’s study, to include
its assessment of the accessibility of lower bunks, external infrastructure,
and handicapped-accessible cells, showers, and toilets, by July 31, 2015.
Recommendation 5: Study the feasibility of creating units, institutions, or
other structures specifically for aging inmates in those institutions with high
concentrations of aging inmates.
Status: Resolved.
BOP Response: The BOP concurred with the recommendation,
stating that it would create a multi-division task force to study the feasibility
of creating units specifically for aging inmates in those institutions with high
concentrations of aging inmates.
OIG Analysis: The BOP’s actions are responsive to the
recommendation. Please provide meeting minutes and the results of the task
force’s deliberation, including the institutions that the task force studied, by
July 31, 2015.
Recommendation 6: Systematically identify programming needs of aging
inmates and develop programs and activities to meet those needs.
Status: Resolved.
BOP Response: The BOP concurred with the recommendation,
stating that it would identify programming needs of aging inmates, develop
64

programs and activities to meet those needs, and incorporate those
programs into the BOP’s Inmate Model Programs Catalog or national policy.
OIG Analysis: The BOP’s actions are responsive to the
recommendation. Please describe the programming needs identified and
provide copies of program curricula and activities developed in response to
those needs, as well as copies of any national policies updated as a result, by
July 31, 2015.
Recommendation 7: Develop sections in release preparation courses that
address the post-incarceration medical care and retirement needs of aging
inmates.
Status: Resolved.
BOP Response: The BOP concurred with the recommendation,
stating that it would identify and develop programs to assist aging inmates in
transitioning back into the community.
OIG Analysis: The BOP’s actions are responsive to the
recommendation. As noted in the report, the BOP’s current release
preparation does not address the needs of aging inmates who are retired or
not seeking employment upon release. Further, aging inmates’ increased
medical needs makes continuity of medical care upon release a pressing
concern. Please provide copies of program curricula developed to address
aging inmates’ release needs, specifically including programs for inmates not
reentering the workforce and addressing continuity of medical care, by
July 31, 2015.
Recommendation 8: Consider revising its compassionate release policy to
facilitate the release of appropriate aging inmates, including by lowering the
age requirement and eliminating the minimum 10 years served requirement.
Status: Resolved.
BOP Response: The BOP concurred with the recommendation,
stating that the criteria concerning aging inmates should be further
evaluated. The BOP stated that it plans to raise the issue with relevant
stakeholders for further discussion and in relation to future policy updates.
OIG Analysis: The BOP’s actions are partially responsive to the
recommendation. As noted in the report, the existing provisions for aging
inmates are ineffective in part because the minimum age provision restricts
eligibility to only a small portion of the aging inmate population and the
minimum time served provisions restrict eligibility even further. Please
provide minutes of meetings between the BOP and other relevant
stakeholders to discuss this topic, copies of BOP data or other BOP
65

information reviewed by the BOP and the other stakeholders in the course of
their deliberations, and the results of the deliberations, by July 31, 2015.
66

The Department of Justice Office of the Inspector General
(DOJ OIG) is a statutorily created independent entity
whose mission is to detect and deter waste, fraud,
abuse, and misconduct in the Department of Justice, and
to promote economy and efficiency in the Department’s
operations. Information may be reported to the DOJ
OIG’s hotline at www.justice.gov/oig/hotline or
(800) 869-4499.
Office of the Inspector General
U.S. Department of Justice
www.justice.gov/oig
