
COMMERCIAL NUISANCE WILD ANIMAL CONTROL OPERATOR
CERTIFICATION MANUAL
january 2024
PUB 5510 R1223

2
Ready to take the test?
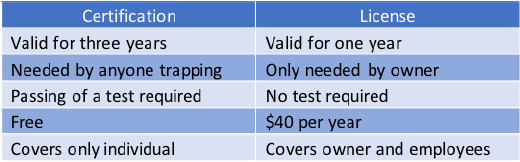
The Commercial Nuisance Wild Animal Control Operator license is considered
a specialty license. Information regarding this license, including the test,
study materials, and application can be found at wildohio.gov.
3
TABLE OF CONTENTS PAGE
CHAPTER 1 – Introduction ............................................................................4
CHAPTER 2 – General Nuisance Wild Animal Laws .............................. 5
CHAPTER 3 – Species Specic Limitations .............................................. 7
• Bats ..................................................................................... 7
• Black Bear ........................................................................7
• Crows .................................................................................7
• Deer ....................................................................................7
• Ducks ................................................................................. 7
• Geese ................................................................................. 7
• Migratory Birds ...............................................................7
• Swans.................................................................................7
• Wild Turkey ...................................................................... 7
• Woodchuck .....................................................................7
• Endangered & Threatened Species .........................7
CHAPTER 4 – Species Information and Control Techniques .............8
• Bats ..................................................................................... 9
• Beaver ................................................................................11
• Canada Goose ................................................................12
• Chipmunks and Small Mammals ............................13
(Moles, Shrews, Mice, Rats, and Voles)
• Coyote ............................................................................... 14
• Fox ......................................................................................15
• Muskrat ............................................................................. 16
• Opossum .......................................................................... 17
• Rabbits ..............................................................................18
• Raccoon ............................................................................ 19
• Skunk ................................................................................. 20
• Snakes ...............................................................................21
• Squirrels ............................................................................22
• Woodchuck .....................................................................23
CHAPTER 5 – Wildlife Diseases ................................................................... 24
CHAPTER 6 – Ethics ........................................................................................30
COMMERCIAL NUISANCE WILD ANIMAL CONTROL OPERATOR
CERTIFICATION MANUAL
4
Chapter 1 – Introduction
This manual is designed to provide general guidance for commercial nuisance wild animal control opera-
tors in Ohio. The intent of the manual is not to provide comprehensive coverage of all laws, methods, and
techniques for nuisance animal control. However, the manual provides relevant information regarding
laws, legal methods of take, species’ life histories, ethical considerations, and wildlife diseases.
DEFINITIONS
Commercial nuisance wild animal control operator: An individual or business that provides nuisance wild
animal removal or control services for hire to the owner, the operator, or an authorized agent of a prop-
erty or a structure.
Nuisance wild animal: A wild animal that interferes with the use or enjoyment of property, is causing a
threat to public safety, or may cause damage or harm to a structure, property, or person.
On-site supervision: Staying near the person being supervised to allow for uninterrupted, unaided visual
and auditory communications.
LICENSING
No person shall provide nuisance wild animal removal or control services for hire without obtaining a
license from the chief of the Division of Wildlife (Ohio Revised Code [O.R.C.] § 1531.40).
If you are providing nuisance wild animal removal or control services and you are charging a fee or an-
other form of compensation, you must have a valid commercial nuisance wild animal control operator
License (here forward, license), or work for someone possessing a license.
An individual who is employed by the state, a county, or a municipal corporation and who performs nui-
sance wild animal removal or control services on land that is owned by the state, county, federal govern-
ment, or municipal corporation as part of the individual’s employment is exempt from obtaining a license.
The fee for obtaining a commercial nuisance wild animal control operator license is $40.00 per year. The
license expires annually on the last day of February and may be renewed.
CERTIFICATION
Certication is required for a commercial nuisance wild animal control operator and any individual who is
working on behalf of an operator who is engaged in activities that are part of or related to the removal or
control of nuisance wild animals, including setting or maintaining traps. However, employees under the
direct on-site supervision of a licensed operator are exempt from certication.
Certication requires passing an online test (80 percent or greater) and is valid for three years from the
date of a passing grade.
PENALTIES
A violation of a nuisance wild animal control law or rule in Ohio may result in criminal charges. Violations
are classied as misdemeanors, depending on the oense, which may result in a ne or jail time. The
ODNR Division of Wildlife may suspend or revoke any nuisance control license if the operator is convicted
of a violation.
OTHER LAWS AND PERMITS
Other state, local, and federal laws, permits, or rules may be applicable to nuisance wild animal control
operators. Therefore, it is the operator’s responsibility to be aware of and become familiar with all perti-
nent laws (such as pesticide application, migratory bird control, Migratory Bird Treaty Act, federal Endan-
gered Species Act.)
Pursuant to O.R.C. § 1533.171, all nuisance wild animal control operators, trappers, and hunters are liable
if injury to a person or property results from a negligent, careless, or reckless act of that person while in
the process of killing or taking a wild animal.
5
Chapter 2 – General Nuisance Wild Animal Laws
This chapter outlines laws and regulations that may be relevant to nuisance wild animal control operators. For relevant statuto-
ry language refer to O.R.C. § 1531.40 and Ohio Administrative Code (O.A.C) 1501.31-15-03 (http://codes.ohio.gov).
MARKING TRAPS, SNARES, OR OTHER DEVICES
All traps, snares, or other unattended devices must always be tagged with one of the following:
Your name and address of the user
OR
Your commercial nuisance wild animal control operator license number
OR
Your Wild Ohio customer ID number
Tags must be legible, in the English language, and must be waterproof.
Traps or devices used for the following animals are not required to be marked:
CHECKING TRAPS
Traps, snares, or other devices used to take or capture nuisance wild animals may be monitored with an operational electronic
device or by personal observation by the person setting the trap or a designated agent. Traps must be checked according to
the following:
Exempt from checking Every 72 hours Every calendar day
Traps set for: Traps set under ice or water for: Traps, snares or other devices set for:
Mice Beaver
All other wild animals not listed in this chart
Nuisance rats River otter
Moles Muskrat
Shrews
Voles
ALLOWABLE TRAPS AND SIZES
Commercial nuisance wild animal control operators shall adhere to the following trap size restrictions:
Trap Type
For use
on land:
submerged or set to function in a lethal
manner in water:
Bodygripping
6 inches or smaller (ex-
cept with woodchuck)
7 inches or smaller (except when com-
pletely submerged)
Foothold (both dogless and with dog) 6 inches or smaller* Not applicable
No spring-assisted snare 15 inches or smaller 15 inches or smaller
Spring-assisted snare 5 inches or smaller 8 inches or smaller
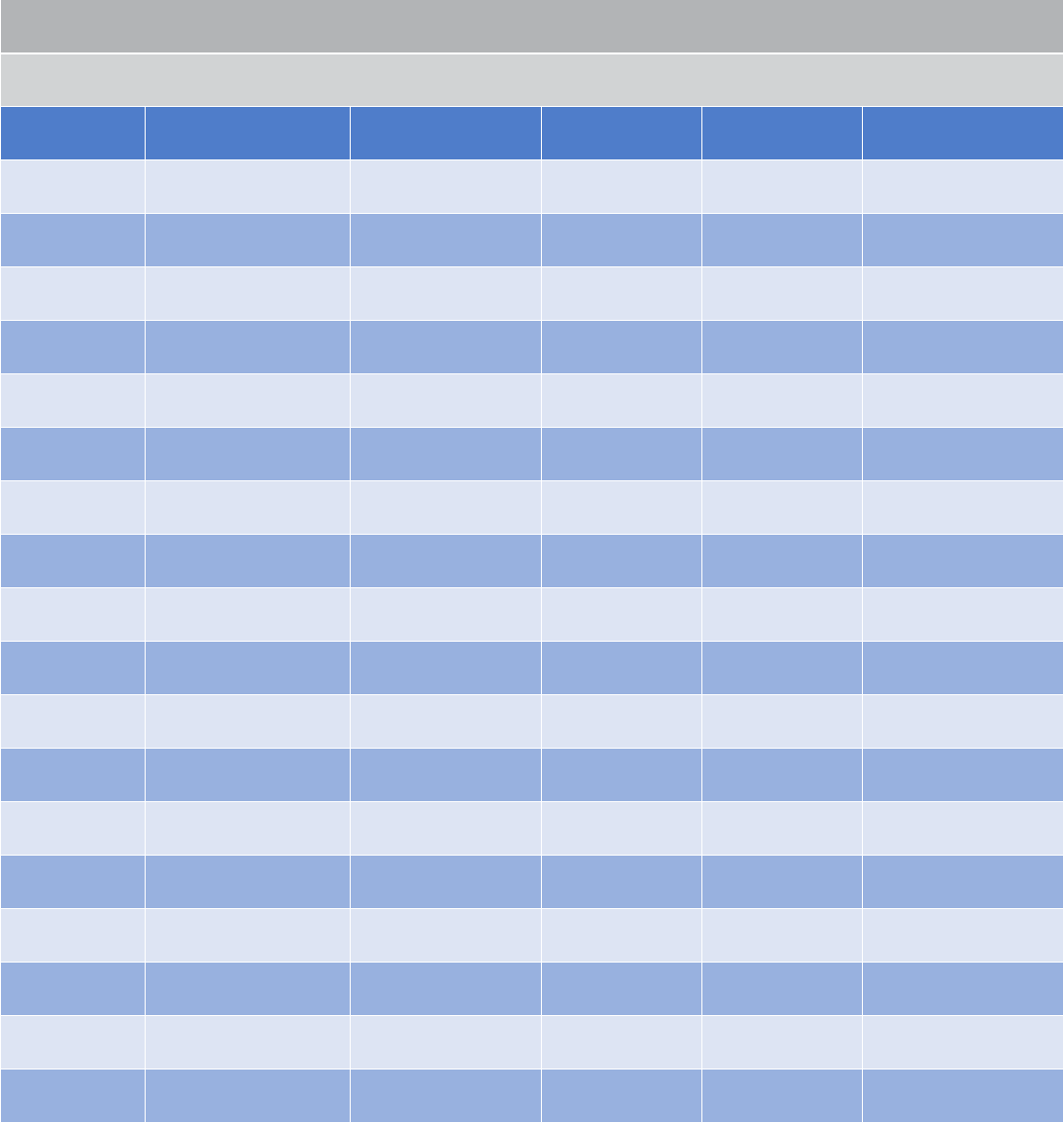
HOW TO MEASURE A TRAP
For the purposes commercial nuisance wild animal control operator license, all traps shall be measured in the open set position,
and measured from the inside of the main trap jaws as manufactured, thus shall not include jaw modications or add-ons.
• MOLES
• SHREWS
• VOLES
• HOUSE MOUSE
MUS MUSCULUS
• NORWAY RAT
RATTUS NORVEGICUS
• ROOF RAT
RAT TUS RATTUS
Bodygripping traps are measured from the
inside of the main jaw at the trigger assem-
bly to the inside of the opposing jaw across
the entrance window.
Foothold traps are measured perpendicular to
the frame at the widest location parallel with
the dog. Dogless foothold traps are measured
perpendicular to the frame at the widest loca-
tion and parallel with the pan shank.
Snares are measured at the diameter of the
loop.
* 5 5/8 inch or smaller- not more than 6 inches if they fall within the following criteria:
• minimum of 5/16 inch gripping surface
• minimum of 3 swiveling points
6
POSSESSION OF NUISANCE WILD ANIMALS
It is unlawful to possess any live wild animal for more than four days
trapped or taken under the authority of a commercial nuisance wild
animal control operator’s license.
SELLING NUISANCE WILD ANIMALS
It is unlawful to sell any nuisance wild animals trapped or taken under
the authority of a commercial nuisance wild animal control operator
license except:
Carcasses or parts, except hides, of:
Hides and tails of red, gray, and fox squirrels trapped or taken under
the authority of a commercial nuisance wild animal control operator
license may be sold at any time.
Hides of furbearing animals taken during the open season under the
authority of a commercial nuisance wild animal control operator li-
cense may be held and sold from the rst day of the respective open
season through June 15 of the following year.
DISPOSITION OF NUISANCE WILD ANIMALS
It is important to check local regulations for acceptable methods of car-
cass disposal.
A commercial nuisance wild animal control operator License requires
the following species to be euthanized or released on-site (if live
trapped) to reduce the issue of moving specic problem individual
animals from one location to another, and to minimize the spread of
disease:
Live trapped animals which may be released outside of city limits (with
permission of the landowner where the release takes place), or may be
euthanized include:
Unless listed above, live-trapped nuisance wild animals must be re-
leased outside of city limits and with the permission of the landown-
er where the release takes place. Refer to Chapter 3 for information on
bats. Under some conditions however, it is impossible to live trap some
animals. In these situations, written permission from the ODNR Division
of Wildlife to use lethal means of capture or taking is required. No such
written permission is required to kill or use lethal means of control for
the following nuisance wild animals:
INJURED NUISANCE WILD ANIMALS
It shall be unlawful to fail to euthanize nuisance wild animals trapped
or taken whose injuries aect normal biological or physiological func-
tions. This does not apply to migratory birds, bats, or threatened or en-
dangered species. An example would be an animal with a badly broken
or severed leg, broken jaw, severe injury to an eye, etc. Call your local
wildlife ocer or the wildlife district oce with questions.
ADDITIONAL TRAPPING RESTRICTIONS
Traps with teeth are illegal for taking a nuisance wild animal, except
traps designed by the manufacturer for mice, moles, or rats.
Snares shall be constructed with only multi-or single- strand steel cable.
All snares, except those set for woodchucks, must have a relaxing lock
and a stop to prevent the opening of the snare from closing to a diam-
eter of less than 2½ inches or a relaxing lock system with a breaking
point of not greater than 350 pounds. Snares shall not be attached to a
drag. Spring-loaded snares, spring-assisted snares, or a snare with a me-
chanical device to assist the snare in capturing or closing around a nui-
sance wild animal may only be used by a licensed commercial nuisance
wild animal control operator and only to take nuisance wild animals.
Flesh bait shall not be used unless it is completely covered and con-
cealed, or unless the bait is encapsulated by the trap.
Dogs shall not be used to take a raccoon, opossum, skunk or fox outside
of a structure during the closed season. The use of dogs to control all
other nuisance wild animals does require a commercial nuisance wild
animal control operator license.
Toxicants and chemical substances may be used for control of nuisance
wild animals. It is unlawful to use contraceptive chemicals except to
control the population of common pigeons. It shall be unlawful to use
a toxicant or chemical substance for the taking or control of a nuisance
wild animal contrary to or in violation of instructions on the label or
manufacturer recommendations (The label is the law). A licensed com-
mercial nuisance wild animal control operator must possess the appro-
priate pesticide applicators license in the appropriate category to use
a toxicant or chemical substance for the taking or control of a nuisance
wild animal. The Ohio Department of Agriculture issues a pesticide ap-
plicator’s license. Additional information on toxicants can be found in
Chapter 4.
Firearms or air guns may be used to take nuisance wild animals in some
situations. It is lawful for a licensed commercial nuisance wild animal
control operator to use a gun equipped with a silencer or muer for the
control of nuisance wild animals. Any applicable federal, state, or local
statutes or restrictions must also be followed.
It is the responsibility of the operator to be knowledgeable of and ad-
here to all applicable rearms laws, and to use them in a safe manner.
As mentioned in Chapter 1, commercial nuisance wild animal control
operators may be liable for the negligent use of a rearm or other im-
plement to take a nuisance wild animal that results in damage to per-
sons or property.
• RACCOON
• OPOSSUM
• BEAVER
• MUSKRAT
• RED OR GRAY FOX
• COYOTE
• SKUNK
• WOODCHUCK
• MINK
• RACCOON
• SKUNK
• BEAVER
• COYOTE
• RED FOX OPOSSUM
• SQUIRRELS
RED, GRAY, FOX,
AND FLYING
• CHIPMUNK
• WOODCHUCK
• MOLES
• VOLES
• SHREWS
• MICE
• RATS
EXCEPT WOOD RATS
• RABBIT
• MINK
• MUSKRAT
• BEAVER
• CHIPMUNK
• MICE EXCEPT
EASTERN HARVEST
MOUSE
• SHREWS
• VOLES
• MOLES
• MUSKRAT
• OPOSSUM
• RACCOON
• RATS
EXCEPT
WOOD RATS
• SQUIRRELS
RED,
GRAY, FOX, AND
FLYING
• SKUNK
• WOODCHUCK
• COYOTE
• RED
• FOX
• MINK
• THIRTEEN
LINED GROUND
SQUIRREL
• FERAL SWINE
• RABBIT
• WEASEL

7
BATS
It shall be unlawful to euthanize or kill any bat, except in situations
where there is a direct human health risk such as a bite or potential
exposure to rabies. Any bat euthanized must be reported to the lo-
cal health department by the aected landowner or their designated
agent by the end of the next business day. If a person has been bit by a
bat or if exposure is possible, the health department must be contacted
for guidance on the disposition of the animal.
Precautions must be taken to ensure that no federally protected spe-
cies are harmed or harassed unless potential exposure to rabies has
occurred. Therefore, it is recommended to follow guidance provided in
Chapter 4.
BLACK BEAR
Black bear which are causing damage or have become a nuisance may
be captured or killed by a licensed commercial nuisance wild animal
control operator, only after the landowner or agent of the landowner
has received a permit from the chief of the ODNR Division of Wildlife.
Stipulations may apply.
CROWS
It is lawful for any person to take crows during the closed season if the
crows are found committing or about to commit depredations upon
ornamental or shade trees, agricultural crops, livestock, or wildlife, or
when concentrated in such numbers and manner as to constitute a
health hazard or other nuisance.
However, it is unlawful to take or attempt to take nuisance crows out-
side of the open season with the aid or assistance of any calls, articially
placed bait, or decoys.
WHITE-TAILED DEER
White-tailed deer which are causing damage or have become a nui-
sance may be captured or killed by a licensed commercial nuisance
wild animal control operator , only after the landowner or agent of the
landowner has received a permit from the chief of the ODNR Division
of Wildlife.
The ODNR Division of Wildlife has an online application and permitting
system for deer damage permits. Landowners with current, ongoing
damage issues can submit an application for a deer damage permit at
wildohio.gov. Stipulations may apply.
All nuisance white-tailed deer immobilized with chemicals or drugs
shall be euthanized.
DUCKS
Ducks, including their nest and eggs, are protected under the Migra-
tory Bird Treaty Act. For removal of nests, eggs, or ducks, the landowner
must contact USDA Wildlife Services for a permit at 1-866-4USDAWS (1-
866-487-3297).
FERAL SWINE
It shall be unlawful to fail to euthanize a trapped nuisance feral swine at
the trap location. Feral swine are a non-native Ohio species. It is illegal
to transport a trapped feral swine in Ohio. It is legal to live trap feral
swine at any time, provided the animal is immediately euthanized at
the trap location.
GEESE
From March 11 through August 31, Canada geese which are causing
damage or have become a nuisance may be captured or taken by li-
censed commercial wild animal control operators, landowners, or
agents of the landowner, only after the landowner has received a per-
mit from the chief of the ODNR Division of Wildlife. Stipulations may
apply.
The ODNR Division of Wildlife has an online complaint and permitting
system for Canada goose damage permits. Landowners can le goose
complaints at wildohio.gov.
From September 1 through March 10, Canada geese which are caus-
ing damage or have become a nuisance may be captured or taken by
licensed commercial wild animal control operators, landowners, or
agents of the landowner, only after the landowner has received a per-
mit from the U.S. Fish and Wildlife Service (USFWS). Information on ob-
taining this permit can be found below.
MIGRATORY BIRDS
There are times when migratory birds are responsible for damage to
property or become a nuisance. European starlings, English sparrows,
and common pigeons (other than homing pigeons) are not considered
migratory birds and may be killed at any time and their nests or eggs
may also be destroyed at any time. They may not however, be pos-
sessed except under a collection permit.
Unless specied below, migratory birds are protected under the Mi-
gratory Bird Treaty Act. The Migratory Bird Treaty Act is a treaty signed
between the United States, Japan, Canada, Russia, and Mexico that es-
tablishes protection for migratory birds, their eggs, and nests.
Removal of migratory birds, such as woodpeckers that are causing
damage, requires a depredation permit from the U.S. Fish and Wildlife
Services. USDA Wildlife Services facilitates the application of the depre-
dation permits. The landowner must contact the USDA Wildlife Services
at 1-866-4USDAWS (1-866-487-3297) to speak to a representative to de-
termine if a permit is needed.
Inactive nests of non-colonial migratory birds may be removed without
a federal permit.
MUTE SWANS
Mute swans may be captured or taken by licensed commercial nuisance
wild animal control operators, landowners, or agents of the landowner,
only after such landowner has received a permit from the chief of the
ODNR Division of Wildlife. Stipulations may apply.
WILD TURKEY
Wild turkey, which are causing damage or have become a nuisance may
be captured or killed by licensed commercial nuisance wild animal con-
trol operators or other persons, only after such landowner or agent of
the landowner has received a permit from the chief of the ODNR Divi-
sion of Wildlife. Stipulations may apply.
GROUNDHOGS (WOODCHUCKS)
Restrictions for nuisance groundhog trapping include:
ENDANGERED & THREATENED SPECIES
It is unlawful to capture or kill nuisance wild animals listed as state en-
dangered or threatened without a permit to do so issued by the chief
of the ODNR Division of Wildlife. For the most up-to-date list, go to wil-
dohio.gov. Caution must be taken so as not to injure or destroy any of
these species, including with pesticides or other lethal means of con-
trol.
Some species of wildlife listed as state endangered or threatened are
also federally listed, and all federal laws regarding those species must be
followed. Please contact the U.S. Fish and Wildlife Service for guidance.
Chapter 3 – Species Specific Limitations
• It is unlawful to use a bodygripping trap with a jaw spread greater than 7 inches across.
It is unlawful to set, use, or maintain a bodygripping trap to take groundhogs which is
set more than 3 feet from the hole, or structure the animal inhabits.
• It is unlawful to set, use, or maintain a bodygripping trap greater than 5 inches to take
a groundhog that does not have an enclosure or structure around the trap which pro-
hibits other animals from getting into the trap from the outside.
• It is unlawful for any person except licensed commercial nuisance wild animal control
operators to use snares without a relaxing lock for taking groundhogs.
8
Chapter 4 –Species Information and Control Techniques
This chapter will explain some of the methods for controlling common nuisance wild animals as well as provide information on their life history,
diseases, and laws pertaining to that species. It does not discuss all methods or all nuisance wild animals that may be encountered.
SPECIESSPECIFIC RECOMMENDED TRAP AND SNARE SIZES
Commonly encountered species of wild animals for nuisance animal control operators and the recommended trap sizes for those species. In
some cases, other sizes or trap types may prove to be more ecient.
Species/ taxa
Foothold
(inches)
Bodygripping (inches) Snare loop (inches) Live/cage Trap Encapsulated (dog proof)
Bats Not legal Not legal Not legal Not recommended Not legal
Beaver 5 - 6 (land), 8¼ (submerged)
1
7-12
2
9 – 10, 2 - 3
3
39 x 43 Suitcase
4
Not recommended
Canada Goose Not legal Not legal Not legal Not legal Not legal
Chipmunks/Rats Not recommended Rat sized snap traps Not recommended 16 x 5 x 5
4
Not recommended
Mice/shrews Not recommended Mouse snap trap Not recommended 10 x 3 x 3
4
Not recommended
Moles Not recommended
“NoMol, Out of Sight, Nash
Loop, spears, or similar”
3
Not recommended 11 x 3 ½ x 3 ½
4
Not recommended
Coyote 4 ½ - 6
2
Not recommended 10-12, 10 – 12
3
high 48 x 26 x 20
4
Not recommended
Red Fox 4 ½ -5 ½
2
Not recommended 6 - 8, 6 - 8
3
high 42 x 15 x 15
4
Not recommended
Gray Fox 4 5/16 - 4 ½
2
Not recommended 6 - 8, 6 – 8
3
high 32 x 10 x 13
2
Not recommended
Muskrat 3 ½ + (submerged)
2
4 ½ -5
2
3 ¾, 1 ½
4
high 24 x 6 x 6
4
Not recommended
Opossum 3 15/16 - 4 ½
2
4 ½ - 6
4
6, 2 - 3
4
high 32 x 10 x 13
2
1 ½- in. diameter, 2 1/8 - 2
7/8 in. trigger depth
Rabbits Not recommended Not legal Not recommended 24 x 7 x 7
4
Not recommended
Raccoon 3 ½ -4 5/8
2
6 (land), 7 (part sub-
merged)
2
6 – 8, 3 – 4
3
high 32 x 10 x 13
2
1 ½- in. diameter, 2 1/8 - 2
7/8 trigger depth
Skunk 3 ½ - 4 ½
5
6 (2) 4 - 6
4
24 x 7 x 7 up to 32 x
10 x 13
2
Not recommended
Squirrel (gray or
fox)
Not recommended 3 ½ - 4 ½
4
Not recommended 19 x 6 x 6
4
Not recommended
Squirrel (red) Not recommended Rat sized snap traps Not recommended 16 x 5 x 5
4
Not recommended
Squirrel (ying) Not recommended Rat sized snap traps Not recommended 16 x 5 x 5
4
Not recommended
Woodchuck No greater than 6 5-7
4
4 – 6, 2 -3
4
high 32x x10 x 13
2
Not recommended
1
OAC 1503:31-05-03
2
Association of Fish and Wildlife Agencies Best Management Practices
3
Recommended by the Ohio State Trappers Association Snare Guide
4
Specic manufacturer’s recommendations
5
U.S. Geological Survey Northern Prairie Wildlife Research Group
9
OHIO NATIVE BAT SPECIES
There are 10 bat species commonly found in Ohio and they are all in-
sectivores, meaning they eat insects. Four species of bats found in Ohio
are state-endangered, including the federally endangered Indiana bat
and the northern long-eared bat. Since the appearance of white-nose
syndrome, bat populations have experienced declines of over 90%.
Population declines of some species that roost in buildings may be as
high as 96% to 99%. Bats are the only major predator of night-ying in-
sects, and they help farmers by saving them billions of dollars a year on
pest control. Bats are usually able to exist near human homes without
making their presence known.
LAWS PERTAINING TO BATS
While all of Ohio’s bat species are protected by law, the Division recog-
nizes there may be times when human health or safety is at risk. For
example, it is illegal to kill a bat for any reason unless a bite or poten-
tial exposure to rabies has occurred. Ohio Administrative Code (OAC)
1501:31-15-03 provides additional opportunities to address human/
wildlife coexistence issues, including the exclusion or eviction of un-
wanted bats from a man-made structure.
It is illegal: To use traps (including glue traps) to catch or kill bats; to use
chemicals, toxicants, or foggers to exclude or kill bats; to seal all entry/
exit points while bats are inside the structure; and to otherwise kill bats.
DISEASES OF CONCERN
WHEN HANDLING BATS
(See Chapter 5 for more
specic information regard-
ing diseases)
• Rabies
• Histoplasmosis
• White-nose syndrome
COMMON SITUATIONS EN-
COUNTERED
• Roosting in chimneys
• Flying around inside
home
• Roosting or colonizing
in attic
TECHNIQUES FOR
DEALING WITH BATS
Living Space: When trying to remove a bat in a living space, open a win-
dow or exterior door, and close interior doors, conning it to one room if
possible. The bat will leave as soon as it locates the exit. If the bat contin
-
ues to stay in the house, you may use a box, bucket or small jar over the
bat to capture. You should never handle the bat with bare hands, so wear
the thickest gloves you can nd, preferably leather gloves to use when
attempting to remove. Put on gloves. Use capture container and place it
over the bat when it lands, whether on the oor or wall. Then, slip a lid or
piece of cardboard under the box. Tape the cardboard to the container
to secure the bat inside. If the bat is unharmed and it is April 1- May 15 or
August 1- October 14 , take the capture container outside and place it up
against a tree so that the bat can crawl out onto the tree as bats cannot
y from the ground.
Exclusion: Removal of bat colonies or individuals roosting in buildings
may be dealt with a bat exclusion. A bat exclusion is dened as the act
of installing a device or materials to remove bats from a structure. If
• RED BAT LASIURUS BOREALIS)
• INDIANA BAT MYOTIS SODALIS)
• HOARY BAT (LASIURUS CINEREUS)
• BIG BROWN BAT EPTESICUS FUSCUS)
• EASTERN SMALLFOOTED BAT MYOTIS LEIBII)
• LITTLE BROWN BAT MYOTIS LUCIFUGUS)
• EVENING BAT (NYCTICEIUS HUMERALIS)
• TRICOLORED BAT PIPISTRELLUS SUBFLAVUS)
• NORTHERN LONGEARED BAT (MYOTIS SEPTENTRIONALIS)
• SILVERHAIRED BAT (LASIONYCTERIS NOCTIVAGANS)
• RAFINESQUE’S BIGEARED BAT CORYNOHINUS RAFINESQUII)
LIFE HISTORY NOTES
Mating: Polygamous.
Peak Breeding Activity: August to October;
some will breed again in the spring.
Gestation: 40-90 days depending on species,
weather conditions, and nutritional availabil-
ity (delayed implantation).
Young are Born: Late May through July .
Litter Size: 1, but there can be large numbers
of young in a colony.
Number of Litters per Year: 1
Seasonal Patterns: While some migrate in
the winter, they can also be year around
residents; Some species will use dierent
roosting, hibernacula, and maternity sites.
Typical Foods: Insects
BATS

10
bats are entering the living space inside of a home (i.e., from attic ac-
cess into a bedroom), these interior routes may be sealed or blocked
at any time without a permit. However, unless otherwise approved by
the Division, exterior routes may not be sealed without rst installing
an exclusion device. The ideal periods for bat exclusion are between
April 1st through May 15th and August 1st through October 15th. The
only allowable method of bat removal is bat exclusion. Exclusion de-
vices or materials allow the one-way passage of bats out of a home or
structure. Installing materials that close secondary access points while
still allowing bats to enter and exit the structure through a main access
point is not considered bat exclusion. Exclusion devices must be left
in place for at least a week to be eective. Once all of the bats have
been excluded from the structure, the device may be removed, and the
entrance sealed within the same day to prevent bats from reentering.
Bats may not be intentionally killed or harmed unless human rabies ex-
posure is suspected.
Requesting Written Permission During Restricted Periods: Before apply-
ing for bat exclusion authorization from May 16th through July 31st,
the property owner or designee must:
• Inspect the structure for bats;
• Perform two bat watches at the structure from ½ hour before un-
til 1 hour after sunrise or from ½ hour before until ½ hour after
sunset within seven days.
• If ve or more bats are observed during the inspection or rst
bat watch, additional watches are not required. Exclusion is not
permitted without the Division’s authorization.
• If four or fewer bats are present or observed, bat exclusion can be
performed without the Division’s authorization.
The Division will consider immediate exclusion when human health
and safety are at risk or when nighttime temperatures exceed 40°F for
the full 10-day forecast during the October restricted dates. Applicants
will typically receive a response to their request within a few days but
no later than ten days after the Division receives it.
Property owners or their agents and Division licensed/certied nui-
sance wild animal control operators may apply for bat exclusion au-
thorization during the restricted periods. It is illegal for anyone who
is not a licensed commercial nuisance wild animal control operator to
receive compensation for wild animal control activities, including bat
exclusions.
Bats may not be killed or euthanized unless a bite or potential exposure
to rabies has occurred. Contact your doctor if rabies is suspected in a
bat or if a bite cannot be ruled out. There are two restricted periods for
bat exclusion in Ohio:
• From May 16th through July 31st, when 5 or more bats are present;
• From October 15th through March 31st, if any bats are present.
During these restricted periods, bats may only be excluded by rst ob-
taining written permission from the chief of the Division of Wildlife or
their designee. Written authorization will be considered when human
health and safety are at risk or when nighttime temperatures exceed
40°F for the full 10-day forecast during the October restricted dates
(see Requesting Written Permission During Restricted Periods below
for additional information). The spring/summer restricted period is in
place to protect bats and their ightless pups during the maternity pe-
riod. Exclusions performed during this time may cause undue deaths of
bats until pups can y (August). Not only could the exclusion result in
the death of pups, but frantic mothers attempting to get back to their
young often nd their way into living spaces. The fall/winter restricted
period is put in place to protect hibernating bats. Bats that exit struc-
tures when temperatures drop below freezing may die if they cannot
return to the same hibernaculum or shelter due to an exclusion device.
To apply for exclusion authorization, please complete and return a Bat
Exclusion Authorization Application (Please contact ODNR Division of
Wildlife customer service at 1-800-WILDLIFE (945-3543) or wildlife.bat-
exclusion@dnr.state.oh.us for more information).
When locating entry and exit areas, consider potential as well as active
points of access. It may also be possible to locate entry and exit areas by
standing in various locations of a darkened attic during daylight hours
and looking for light at the extreme parts of eaves, in layers of subroof-
ing, and below chimney ashings. Seal all gaps of ¼ x 1½ inches (0.6
x 3.8 cm) and openings 5/8 of an inch (1.6 cm) or larger. Often, there
are secondary access points that are not always used. These secondary
access points may be sealed in advance of sealing the primary access
point if you are waiting for pups to be ighted.
There are many commercially available one-way door devices that you
can install to allow the bats to leave the following night that will ex-
clude them from being able to get back in. You can also use screen and
tape to create your own one-way door. Put a square section of screen
just slightly larger than the hole they are using over it, and then tape
three sides leaving the bottom side open to allow the bats to squeeze
out. Be sure the screen is tight enough so that there is not a gap for
them to climb back in, but not too tight to keep them from being able
to get out. It is recommended that exclusion of colonies take place after
September 1, but before bats begin hibernation. Excluding bats during
the wrong time of year can lead to far greater problems for the home-
owner, including bats dying and creating an odor problem, or more
bats getting inside the living quarters seeking a way out.
Habitat modication: Installation of bat houses may help deter bats
from using a structure, but it must also be considered that it may attract
bats to the area as well. In dark areas such as attics, leaving lights on or
install lights to help repel bats. In areas where bats are roosting, such
as under sots and above doors, using a 45-degree piece of wood can
deter the bats from using that area.
11
LAWS PERTAINING TO BEAVER
Can be trapped or shot at any time if causing a nuisance. If trapped, can
NOT be relocated and must be euthanized.
DISEASES OF CONCERN WHEN HANDLING
(See Chapter 5 for more specic information regarding diseases)
• Tularemia
• Giardia
RECOMMENDED TRAP SIZES (all sizes in inches)
FOOTHOLD
BODY-
GRIPPING
SNARE LOOP
with HEIGHT
LIVE or
CAGE TRAP
5 - 6 (land)
5 – 8 1/4 (submerged)
7-12 9-10, 2-3
39 x 43
Suitcase
COMMON SITUATIONS ENCOUNTERED
• Cutting trees
• Plugging pipes
• Flooding an area
TECHNIQUES FOR DEALING WITH BEAVER
Trapping: It is recommended that traps set for beaver be used in a
lethal manner in either deeper water or with the aid of a drowning
set. The most eective sets are those placed in runs, places where the
beaver enters and exits the water, or at the entrance to a beaver lodge.
Place the trap as close to the den entrance as possible without restrict-
ing trap movement. Snares can be set for beavers on land and in water.
Shooting: Beavers are generally nocturnal. Shooting a beaver can be ef-
fective at night with proper lighting. Check local regulations before dis-
charging a rearm within a city or village. Extreme care must be taken
when shooting beaver to diminish the likelihood of ricocheting bullets
o the water surface.
Exclusion: It is dicult as well as cost prohibitive to exclude beavers
from ponds, lakes, or impoundments. Fencing of culverts, drain pipes,
or other structures can sometimes prevent damage, but fencing can
also promote damage, since it provides beavers with construction ma-
terial for dams. Protect valuable trees adjacent to waterways by encir-
cling them with hardware cloth, woven wire, or other metal barriers.
Construction of concrete spillways or other permanent structures may
reduce the impact of beavers.
Habitat modication:
Where feasible, elim-
inate food, trees, and
woody vegetation
that is adjacent to bea-
ver habitat. Continual
destruction of dams
and removal of dam
construction materials
daily will sometimes
cause a colony or in-
dividual beavers to
move to another site.
The use of a three-log
drain or a structural de-
vice such as wire mesh
culverts or T-culvert
guards will occasion-
ally cause beavers to
move to other areas.
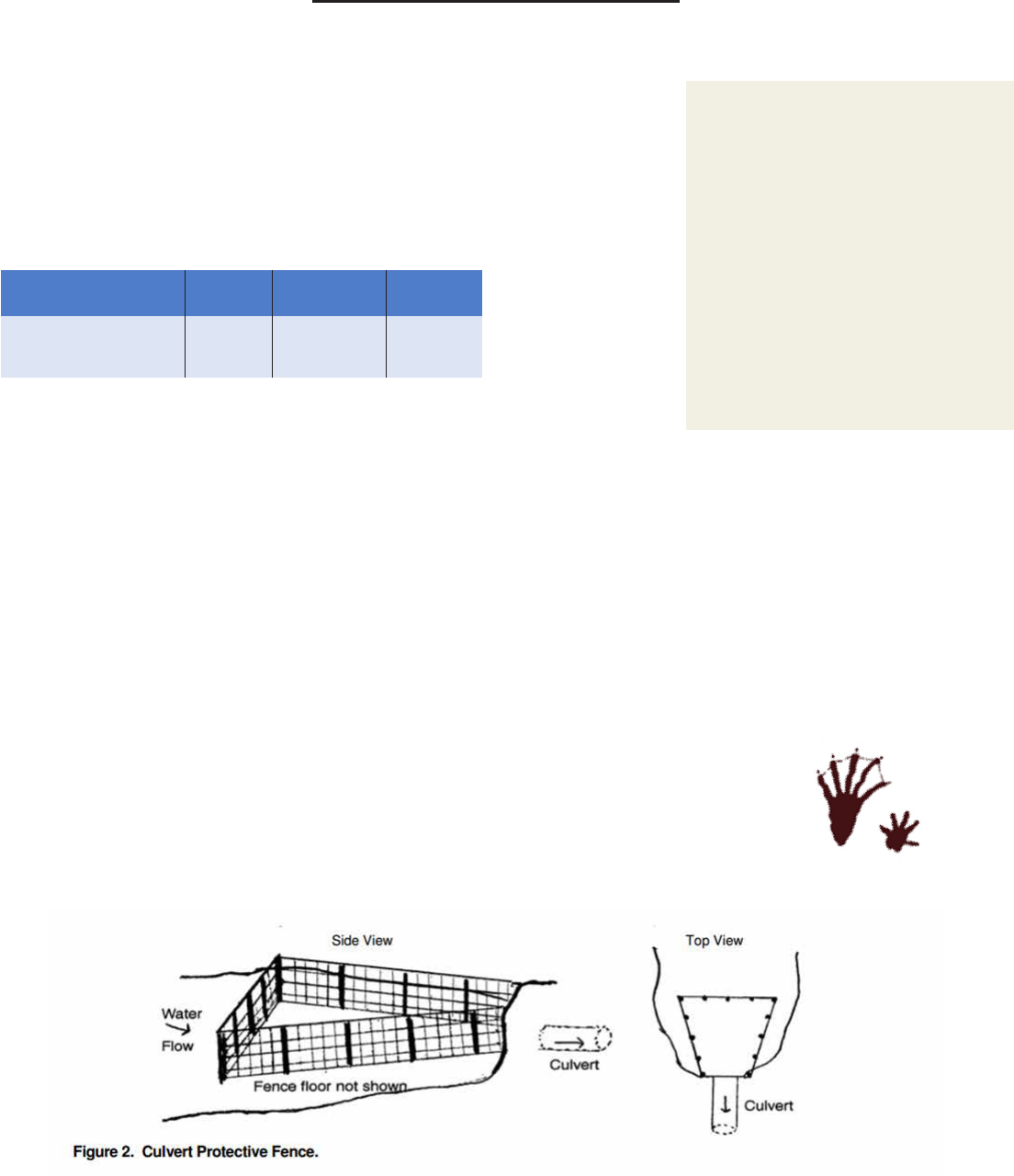
Fencing around culvert
heads can also be constructed to allow beavers to build but still allow
water ow. The length of each side of the fence is normally at least twice
the diameter of the culvert. Installing this device can be the best solu-
tion for a large owage where the water ow is too great for a pipe sys-
tem or smaller owages where roads were built in oodplains. A oor
of fencing is usually laid rst to deter beaver burrowing.. A device for
controlling beaver impoundments and keeping blocked culverts open
is the Clemson beaver pond leveler. It is eective because the beavers
cannot detect the sound of falling or owing water as the pond or cul-
vert drains; therefore, they do not try to plug the pipe. Periodic reinva-
sions of suitable habitat can be expected to occur.
Frightening: Shooting of individuals or continued destruction of lodg-
es, bank dens, and dams, where legal, will occasionally move young
colonies out of an area.
Toxicants and fumigants: None registered.
Repellents: None registered.
LIFE HISTORY NOTES
Mating: Monogamous.
Peak Breeding Activity: January-February.
Gestation: 3-4 months.
Young are Born: April-June .
Litter Size: 1-8; average 3.
Number of Litters per Year: 1.
Seasonal Patterns: Year-around resident;
Active primarily at night however will be
out during the day as well.
Typical Foods: While they will eat or chew
almost any tree, they prefer poplar, aspen,
willow, birch, and maple.
BEAVER
(CASTOR CANADENSIS)
12
LAWS PERTAINING TO CANADA GEESE
There are no permits needed to harass Canada geese, as long as they
are not nesting. Permits for nests, eggs, shooting, or rounding up the
geese from March 15-August 31 require a permit from the ODNR Di-
vision of Wildlife. Permits for shooting from September 1-March 14 re-
quire a permit facilitated by the U.S. Department of Agriculture Wildlife
Services.
*The ODNR Division of Wildlife utilizes an online goose complaint and permitting system.
Landowners can le complaints at wildohio.gov or call the nearest district oce. A com-
plaint must be led before any permits can be issued.
DISEASES OF CONCERN WHEN HANDLING
(See Chapter 5 for more specic information regarding diseases)
• Avian inuenza
• E. Coli
• Botulism
• Avian cholera
RECOMMENDED TRAP SIZES
A permit is required to trap Canada geese.
COMMON SITUATIONS ENCOUNTERED
• Defecating on lawn
• Aggression towards people and pets
• Nesting location (by doors, walkways, landscaping, roofs, parking
lots, etc.)
• Destroying grass, yards, or golf courses
TECHNIQUES FOR DEALING WITH CANADA GEESE
Trapping: A nuisance goose capture permit is required from the ODNR
Division of Wildlife to trap geese. Capture permits are reserved as last
resort tactics, used only after complainants have attempted nonlethal
harassment tactics without satisfactory results. Roundups are conduct-
ed in June and July when the goslings cannot y and the adult geese
are molting, or replacing, their feathers. This permit can also be used in
a situation where an aggressive goose needs to be removed. When an
attack goose situation occurs and an ODNR Division of Wildlife employ-
ee determines the best course of action is removal of one or both geese,
this permit allows for hand-capturing the goose and euthanizing it.
Shooting: As with trapping, shooting permits are reserved as last resort
tactics. Shooting geese should be used to reinforce nonlethal tactics
which must continue after the permit is issued. Shooting permits are
typically issued in agricultural situations. In general, shooting permits
are issued early in the nesting season and are used to discourage birds
from feeding on emerging crops or to discourage birds from utilizing
a site. Flightless geese, including molting birds and goslings, are not
allowed to be shot. Check local regulations before discharging a rearm
within a city or village.
Exclusion: Installing perimeter fencing around a pond or using an over-
head grid system can help to prevent access to geese. Physical barriers
should be installed prior to March, before goose territories are estab-
lished, and the barriers should be left intact year-round. When prop-
erly installed and maintained, physical barriers will prevent geese from
walking from the pond into your yard.
Habitat modication: Geese are grazers and rely on grass for most of
their diet. Geese can be discouraged from using these grass areas by
the following methods: 1) Reduce or eliminate fertilizer applications to
the surrounding grass area to make the grass less desirable and nutri-
tious to the geese; 2) Plant grass species that are less desirable, such as
tall fescue (has a bitter taste); 3) Seed surrounding areas to natural prai-
rie grasses or other tall vegetation; 4) Dense plantings around feeding
areas and tall trees in ight paths will deter geese from using these ar-
eas; 5) Turn o pond aerators in the winter to allow the pond to freeze;
and 6) Do not feed the geese.
Frightening: Almost
any obedient breed
of dog, when trained
properly, can be used
to discourage Cana-
da geese. However,
border collies seem
to be the breed of
choice. A border col-
lie’s natural herding
instinct, along with
some command
training, make it par-
ticularly useful for
discouraging Cana-
da geese from areas
with ponds including
golf courses, apart-
ment complexes,
and industrial parks. It is best to use dogs to discourage geese before
and after the nesting season (before March 15th and after eggs have
hatched). Once geese are actively nesting, it is dicult to drive them o
your property. Noise makers, including screamers, bangers, and shell
crackers are eective. For best results, begin harassment early in the
season (February and March) and during dusk or early evening when
the birds congregate in numbers. Harassment at this time will disperse
the birds before they roost for the night and become accustomed to
the area. Care should be given to not overuse noise makers because
geese can become accustomed to the persistent noise. Often, congre-
gated birds must be harassed for several days before any results will be
seen. Be persistent and you will succeed. It is advised to contact local
law enforcement ocials before using noise makers in a city or village.
Toxicants and fumigants: None registered.
Repellents: Two types of chemicals are registered with the U.S. Envi-
ronmental Protection Agency as goose repellents: methyl anthranilate
(MA) and anthraquinone (AQ). Both chemicals were originally designed
to be sprayed on grass, thus making the grass unpalatable to geese. In
recent years, however, MA has also been used as an aerosol to chase
geese away. MA is a naturally occurring nontoxic, biodegradable food
ingredient found in concord grapes and orange blossoms. Two MA-
based repellents found in the marketplace are ReJeXiT and Repel. AQ
is a naturally occurring compound found in many plants and is virtually
odorless. The compound is harmless to wildlife and humans, and it per-
sists in all weather conditions (rain, snow, ice). Flight Control is the only
AQ-based repellent currently on the market.
Handling Geese: When operating under either a nuisance goose cap-
ture permit or dealing with an attack goose, it is important that all
geese are handled properly. The photos below will instruct you on how
to properly handle geese when working under these permits.
STEP 1
Gently hold the goose down to the ground
STEP 2
Grasp both wings where they meet the body
STEP 3
Grasp both legs with the other hand
STEP 4
Gently lift the goose and hold it against your body
• Do NOT grab geese by the neck or head
• Do NOT grab goslings with down feathers by the wings. Gently hold
them around their body and cradle them like a football against your
body.
• Watch the head so that the goose does not turn around and bite
you
LIFE HISTORY NOTES
Mating: Monogamous
Peak Breeding Activity: February-March
Gestation: 26-28 days
Young are Born: May
Clutch Size: 2-9; Average 5
Number of Broods per Year: 1
Seasonal Patterns: Some geese will be
around all year; Ohio also gets migrant
geese
Typical Foods: Grass and aquatic
vegetation
CANADA GOOSE
(Branta canadensis)

13
LAWS PERTAINING TO SMALL RODENTS
Can be trapped or shot at any time if causing a nuisance. If trapped,
they can be euthanized OR relocated after receiving permission from
the landowner where it will be released.
DISEASES OF CONCERN WHEN HANDLING SMALL RODENTS
(See chapter 5 for more specic information regarding diseases)
• Hantavirus
RECOMMENDED TRAP SIZES (All sizes in inches)
COMMON SITUATIONS ENCOUNTERED
• Holes and tunnels in yard
• Chewing holes in home, garage, or barn
• Eating landscape plants
TECHNIQUES FOR DEALING WITH SMALL RODENTS
Trapping: Trapping is the most practical method of eliminating small ro-
dents in most situations. Live-catch wire-mesh traps or common snap traps
can be used to catch most small rodents. Baits used to lure them into live
traps include peanut butter, nutmeats, pumpkin or sunower seeds, raisins,
prune slices, or common breakfast cereal grains. A helpful tip is to pre-bait
the trap for 2 to 3 days by wiring the trap doors open. This will condition
the animal to associate the new metal object in its territory with the new
free food source. Bodygripping or spear traps can be eective for dealing
with moles. The traps are usually set in-line with the tunnel the moles are
creating in the yard. Traps must be checked each calendar day.
Shooting: The use of an air rie or a .22-caliber rie with bird shot or
C.B. cap loads can be an eective method to kill small rodents. Check
local regulations before discharging a rearm within a city or village.
Exclusion: Rodents can t through small holes. Use hardware cloth
with 1/4-inch mesh, caulking, or other appropriate materials to close
openings where they could gain entry. In many cases, seeds and bulbs
can be covered by 1/4-inch hardware cloth and covered with soil to
protect the seeds and bulbs from being eaten but allow them to grow
through the hardware cloth. The cloth should extend at least 1 foot past
each margin of the planting. Exclusion is less expensive in the long run
than trapping.
Habitat modica-
tion: Landscaping
features, such as
ground cover, trees,
and shrubs, should
not be planted in
continuous fashion
connecting wooded
areas with the foun-
dations of homes.
They provide protec-
tion for small rodents
that may attempt
to gain access into
the home. Place bird
feeders at least 15
to 30 feet away from
buildings so spilled
bird seed does not
attract and support
rodents near them.
Spilled bird seed
should be removed
daily.
Frightening: En-
couraging a rodent’s
natural enemies will
greatly help in reduc-
ing their presence.
Hawks, owls, foxes,
coyotes, and snakes
all help control ro-
dent populations.
While decoys may
temporarily help,
encouraging live
hawks, owls, fox,
coyotes, and snakes will have a much larger benet.
Toxicants and fumigants: None registered.
Repellents: None registered.
Other Comments: Many small rodents, especially white-footed mice, are
important reservoirs for the bacterium for Lyme disease. While they can’t
pass Lyme disease to humans they can be an important management
component to dealing with the other animals that ticks use as hosts.
BODYGRIPPING LIVE or CAGE TRAP
Chipmunks
and rats
Rat-sized snap trap 16 x 5 x 5
Mice and
shrews
Mouse sized snap trap 10 x 3 x 3
Moles
Several commercially avail-
able traps; spear type trap
11 x 3 ½ x 3 ½
LIFE HISTORY NOTES
Mating: Polygamous
Peak Breeding Activity: Can be through-
out the year, but usually during the spring
and fall
Gestation:
Voles and Shrews - 19 days
Chipmunks - 31 days
Moles - 42 days
Mice - 25 days
Rats - 22 days
Young are Born: Can be throughout the
year, but usually during the spring and fall
Litter Size: Average 4-5
Number of Litters per Year: Shrews and
moles - 1 litter
Chipmunks - 2 litters
All others – More than 2 litters
Seasonal Patterns: Year-around resi-
dent. Active both during day and night
throughout the entire year
Typical Foods: Vegetation, seeds, nuts,
fruits, insects, and grubs. Moles feed on
earthworms as well.
Make sure you know which small rodent you are dealing with before control activities.
Many small mammals are similar in appearance and habitat.
MOLES, VOLES, SHREWS, MICE, RATS, AND CHIPMUNKS

14
LAWS PERTAINING TO COYOTES
Can be trapped or shot at any time if causing a nuisance. If trapped, can
NOT be relocated and must be euthanized. CANNOT be rehabilitated if
injured or orphaned.
DISEASES OF CONCERN WHEN HANDLING
(See chapter 5 for more specic information regarding diseases)
• Rabies
• Canine distemper
• Parvovirus
RECOMMENDED TRAP SIZES (All sizes in inches)
COMMON SITUATIONS ENCOUNTERED
• Conicts with domestic pets
• Killing livestock and poultry
TECHNIQUES FOR DEALING WITH COYOTES
Trapping: The use of a snare usually aords the best option especial-
ly in an urban setting. Sites where snares are set should be carefully
selected to avoid capturing non-target animals. Avoid setting snares
on any trails being used by non-target animals or domestic dogs. Use
a short snare cables to reduce injuries for accidentally-captured dogs.
Shooting: A rie or other rearm is an eective method to kill a coy-
ote. There is no closed season for hunting coyotes (although there are
some time restrictions during deer gun seasons) and the use of hunt-
ing is an eective maintenance tool for controlling coyote problems.
Coyotes may even be shot at night (check Ohio hunting and trapping
regulations for any additional laws about shooting coyotes at night),
however care should be taken to ensure all shots are done safely. If
coyotes are killing sheep or other livestock in the daytime, construct a
comfortable blind at a vantage point in the pasture where the killing
has occurred. Check local regulations before discharging a rearm
within a city or village.
Exclusion: While total exclusion of all coyotes by fencing is highly un-
likely, good fences can be important in reducing livestock predation or
incidents with domestic animals, as well as increasing the eectiveness
of other damage control methods (such as snares, traps, or guarding
animals). Coyotes that climb fences can be prevented by adding a
charged wire at the top of the fence or installing a wire overhang. With
any fencing, regular maintenance checks to repair damage is essential.
Most situations with dogs involves the dog chasing after the coyote be-
fore the actual conict occurs.
Habitat modication:
Removal and prop-
er disposal of dead
livestock are import-
ant in rural nuisance
situations. Livestock
producers should use
a fall lambing or calv-
ing program. Coyotes
tend to kill sheep at
night, so conning
sheep is one of the
most eective means
of reducing losses to
predation. Pets in ur-
ban areas, especially
from January through
April, should not be let out between sunset and sunrise without either
being on a lead, within a fenced in area, or with the owner who is con-
dent that the pet will not chase after a coyote or other wild animal.
Frightening: Frightening techniques are not usually eective in urban
areas. However, frightening devices can be useful for reducing losses
during short periods or until coyotes are able to be shot or trapped in
rural areas. The devices should not be used for long periods of time.
Lights above corrals at night have been shown to help reduce losses
by coyotes
Toxicants and fumigants: Toxicants are eective when used according
to the label and with proper licensing from the Ohio Department of
Agriculture. Check with USDA Wildlife Services before purchasing or
using toxicants.
Repellents: The use of guard animals such as llamas, donkeys, and
guard dogs can greatly help to reduce coyote predation on livestock.
Other Comments: Coyotes are common inhabitants of urban areas
and in most cases removal is not necessary. The most common issue
in urban areas is coyotes attacking domestic cats. This issue can almost
entirely be solved by not allowing cats to free-range or ensuring the cat
is indoors from sunset to sunrise.
COYOTE
(CANIS LATRANS)
LIFE HISTORY NOTES
Mating: Monogamous
Peak Breeding Activity: February and
March
Gestation: 58-63 days
Young are Born: Late April or May
Litter Size: 5-7
Number of Litters per Year: 1
Seasonal Patterns: Year-round resident;
active primarily at night and sometimes
during the day.
Typical Foods: Small mammals (voles,
shrews, mice, rabbits), carrion, poultry,
sheep
FOOTHOLD SNARE LOOP/HEIGHT LIVE/CAGE TRAP
4 1/2 - 6 10 - 12, 10 - 12 48 x 26 x 20

15
FOOTHOLD SNARE LOOP/HEIGHT LIVE/CAGE TRAP
Red Fox 4 ½-5 ½
Gray Fox 4 5/16 – 4 ½
6-8
6-8
Red Fox 42 x 15 x 15
Gray Fox 32 x 10 x 13
LIFE HISTORY NOTES
Mating: Monogamous
Peak Breeding Activity: March-May
Gestation: 22-30 days
Young are Born: Throughout the year
Litter Size: 4-7
Number of Litters per Year: 2-3
Seasonal Patterns: Year-round resident;
active primarily at night, and sometimes
during the day
Typical Foods: Aquatic vegetation, clams,
frogs, craysh, and small sh
LAWS PERTAINING TO FOXES
Red fox can be trapped or shot at any time if causing a nuisance. If
trapped, red fox CANNOT be relocated and must be euthanized or re-
leased on site. Gray fox can be trapped if causing a nuisance. Prior writ-
ten approval from the ODNR Division of Wildlife must be obtained to
euthanize a gray fox. Otherwise, gray fox must be released on site.
DISEASES OF CONCERN WHEN HANDLING
(See chapter 5 for more specic information regarding diseases)
• Rabies
• Canine distemper
• Leptospirosis
• Echinococcus Infection
• Sarcoptic Mange
RECOMMENDED TRAP SIZES (All sizes in inches)
COMMON SITUATIONS ENCOUNTERED
• Killing poultry
TECHNIQUES FOR DEALING WITH FOX
Trapping: A great deal of expertise is required to eectively trap foxes.
Trapping by inexperienced people may serve to educate foxes, making
them dicult to catch, even by experienced trappers. Traps with oset
and padded jaws cause less injury to conned animals and facilitate the
release of nontarget captures. In addition to foothold traps, snares are
also an eective method for trapping foxes. Cage traps are sometimes
eective for capturing juvenile red foxes living in urban areas.
Shooting: It is lawful to take nuisance red fox which cannot be live
trapped because of certain conditions by shooting. A rie or other re-
arm can be an eective method. Foxes, especially in damage situations,
are usually not seen during the day because of their nocturnal habits.
Shooting them can be eective at night with proper lighting. A rie of
most calibers or a shotgun will eectively kill a fox. If a fox is killing poul-
try, construct a blind at a vantage point close to where poultry has been
killed. Check local regulations before discharging a rearm within a city
or village. Prior written approval from the ODNR Division of Wildlife is
required prior to killing a nuisance gray fox.
Exclusion: Construct net wire fences with openings of 3 inches or less
to exclude red foxes. Bury the bottom of the fence 1 to 2 feet with an
apron of net wire extending at least 12 inches outward from the bot-
tom. A top or roof of net wire may also be necessary to exclude all foxes,
since some will read-
ily climb a fence. A
three-wire electric
fence with wires
spaced 6 inches, 12
inches, and 18 inch-
es above the ground
around a poultry
yard can help repel
foxes.
Habitat modica-
tion: The protection
of livestock and
poultry from fox
depredation is most
important during the
spring denning peri-
od when adults are
actively acquiring
prey for their young, especially if there is a history of fox depredation.
Foxes frequently den near humans, such as under decks or barns. A usu-
al attractant for a fox in an area are large numbers of small mammals.
Reducing the number of small mammals (see the small mammal sec-
tion) can help deter foxes from frequenting an area.
Frightening: Frightening techniques are not usually eective in urban
areas. However, frightening devices can be useful for reducing losses
during short periods or until foxes are able to be shot or trapped in rural
areas. The devices should not be used for long periods of time. Lights
over poultry yards or coops at night can help to reduce losses by a fox.
Another advantage of lighting is that foxes are more vulnerable to be-
ing shot. Flashing lights, such as a rotating beacon or strobe light, may
also provide temporary protection.
Toxicants and fumigants: Pesticides use is restricted by federal and
state laws. Toxicants can be eective when used according to the label
and with proper licensing from the Ohio Department of Agriculture.
Check with USDA Wildlife Services before purchasing or using toxicants.
Repellents: The use of guard animals such as llamas, donkeys, and
dogs (Great Pyrenees, Komondor, Anatolian Shepherd, and Akbash va-
rieties are commonly used) can greatly help to reduce fox predation on
poultry or livestock.
Other Comments: None.
RED FOX AND GRAY FOX

16
LAWS PERTAINING TO MUSKRATS
Can be trapped or shot at any time if causing a nuisance. If trapped,
they can be euthanized OR relocated after receiving permission from
the landowner where it will be released.
DISEASES OF CONCERN WHEN HANDLING
(See chapter 5 for more specic information regarding diseases)
• Tularemia
RECOMMENDED TRAP SIZES (All sizes in inches)
COMMON SITUATIONS ENCOUNTERED
• Den holes along pond edge
TECHNIQUES FOR DEALING WITH MUSKRATS
Trapping: It is recommended that traps set for muskrats be used in
a lethal manner in either deeper water or with the aid of a drowning
set. The most eective sets are those placed in runs or trails where the
muskrat’s hind feet scour out a path into the bottom from repeated
trips into and out of the den. Place the trap as close to the den entrance
as possible without restricting trap movement.
Snares can be set for muskrats on land and in water. The use of the cage
or colony type trap is permissible and is an appropriate trap if the musk-
rats are to be relocated. A box or live trap may be eective, but are not
typically used.
Shooting: A rie or other rearm can be an eective method to kill a
muskrat. Check local regulations before discharging a rearm within
a city or village. Extreme care must be taken when shooting muskrats
with a rie to diminish the likelihood of ricocheting bullets o the wa-
ter’s surface. For this reason, it is recommended that muskrats are only
shot when on land when using a rie. If shooting the muskrats on the
water is the only option, a shotgun is the best choice.
Exclusion: Exclusion through buried fencing (usually chain-link) 4 feet
above and 4 feet below the waterline on dikes or dams especially when
done during the con-
struction phase can
be helpful in stopping
muskrats from creating
holes on the dike or
dam. Using short fenc-
ing can also be helpful
where muskrats may
be leaving a pond or
lake to cut valuable
garden plants or crops.
It is easiest to fence
the plants you want to
protect since muskrats
could dig under fenc-
ing along the pond edge. Various compa-
nies, including Agridrain, sell animal or bar guards to install on the end
of the pipe which help to exclude muskrats from blocking water ow
into the pipe.
Habitat modication: Serious damage often can be prevented by con-
structing dams to the following specications: the inside face of the
dam should be built at a 6-to-1 slope; the outer face of the dam at a
2-to-1 slope with a top width of not less than 8 feet, preferably 10 to
12 feet. The normal water level in the pond should be at least 3 feet
below the top of the dam. Muskrats in some situations can be excluded
or prevented from digging into pond edges or other shoreline areas
through stone rip-rapping. Limestone rip rap sizes No. 1 or No. 2, or D
rock placed 3-4 inches thick from bottom of the levee to several feet
above the normal waterline is needed. Also, drawing the pond or wet-
land down in the winter months helps prevent muskrats that use bank
dens.
Frightening: No conventional frightening devices are eective.
Toxicants and fumigants: Zinc phosphide can be an eective toxicant
when used according to the label and with proper licensing from the
Ohio Department of Agriculture.
MUSKRAT
(ONDATRA ZIBETHICUS)
FOOTHOLD BODYGRIPPING
SNARE LOOP
WITH HEIGHT
LIVE OR CAGE
TRAP
3
1/2
or larger
(submerged)
4
1/2
- 5 3
3/4
1
1/2
24 x 6 x 6
LIFE HISTORY NOTES
Mating: Monogamous
Peak Breeding Activity: March-May
Gestation: 22-30 days
Young are Born: Throughout the year
Litter Size: 4-7
Number of Litters per Year: 2-3
Seasonal Patterns: Year-round resident;
active primarily at night, and sometimes
during the day
Typical Foods: Aquatic vegetation, clams,
frogs, craysh, and small sh

17
LAWS PERTAINING TO OPOSSUMS
Can be trapped or shot at any time if causing a nuisance. If trapped, can
NOT be relocated and must be euthanized.
DISEASES OF CONCERN WHEN HANDLING OPOSSUM
(See chapter 5 for more specic information regarding diseases)
• Rabies
• Leptospirosis
RECOMMENDED TRAP SIZES (All sizes in inches)
COMMON SITUATIONS ENCOUNTERED
• Denning under a porch, deck, or shed
• Denning in a chimney
• Getting into trash
• Eating food left outside for pet
TECHNIQUES FOR DEALING WITH OPOSSUM
Trapping: Opossums are not wary of traps and may be easily caught
with suitable sized box or cage traps. Foothold traps in a dirt hole set or
cubby set are eective. Bodygripping traps can also be eective. Using
fruit for bait such as apples, cherries, peaches, or grapes instead of meat
as this practice will reduce the chance of catching cats, dogs, or skunks.
Also, traps set on a running pole, on a picnic table, or o the ground to
further reduce the chance of catching a skunk.
Shooting: A rie of almost any caliber, or a shotgun loaded with No.
6 shot or larger, will eectively kill opossums. Check local regulations
before discharging a
rearm within a city
or village.
Exclusion: Keep
opossums from den-
ning under build-
ings by sealing o
all foundation open-
ings with wire mesh,
sheet metal, or con-
crete. Opossums
can be prevented
from climbing over
wire mesh fencing
by installing a tight-
ly stretched electric
fence wire near the
top of fence 3 inches
out from the mesh.
A properly installed
chimney cap will pre-
vent opossums from
entering a chimney.
Make sure trash is in containers and lids are secured.
Habitat modication: Opossums are opportunistic and will readily take
advantage of most any food source. They can be discouraged from an
area by eliminating food sources such as pet food, bird seed, fallen fruit,
compost piles, and household trash. Remove cover such as brush piles,
wood piles, and other piled debris. Properly dispose of garbage and re-
move other food sources such as pet food. Areas around cooking grills
should be cleaned regularly.
FOOTHOLD BODYGRIPPING
SNARE LOOP
with HEIGHT
LIVE or
CAGE TRAP
Encapsulated
(dog proof)
3 15/16 - 4
1/2
4 1/2 - 6 6/2-3 32 x 10 x 13
1 1/2 diameter,
2 1/8 – 2 7/8
trigger depth
LIFE HISTORY NOTES
Mating: Polygamous
Peak Breeding Activity: February-March
but can run from January-October
Gestation: 12-13 days
Young are Born: Peak is March-April, but
can be February-November
Litter Size: 5-25; average is 9
Number of Litters per Year: 1-3; 1 is typi-
cal in Ohio
Migration Patterns: Year-round resident;
individuals wander widely with a home
range of 15-40 acres
Typical Foods: Omnivorous. Will eat
carrion, insects, sh, reptiles, eggs, fruits,
vegetables, and nuts
OPOSSUM
(DIDELPHIS VIRGINIANA)

18
LAWS PERTAINING TO RABBITS
Can be trapped at any time if causing a nuisance. If trapped, they may
be euthanized or released with landowner permission.
DISEASES OF CONCERN WHEN HANDLING RABBITS
(See chapter 5 for more specic information regarding diseases)
• Tularemia
• Staphylococcosis
RECOMMENDED TRAP SIZES (All sizes in inches)
COMMON SITUATIONS ENCOUNTERED
• Garden damage
• Damaging trees
• Eating landscape plants
TECHNIQUES FOR DEALING WITH RABBITS
Trapping: Trapping with live or cage traps is the best way to remove
rabbits in cities, parks, and suburban areas. Place traps where you know
rabbits feed or rest and near cover so that rabbits won’t have to cross
large open areas to get to them. Traps must be checked each calendar
day. Move traps if they fail to make a catch within a week. For best re-
sults, use baits that are similar to what the target rabbits are feeding
on. A commercial wire trap can be made more eective (especially in
winter) by covering it with canvas or some other dark material. Be sure
the cover does not interfere with the trap’s mechanism.
Shooting: Check local regulations before discharging a rearm within
a city or village.
Exclusion: One of the best ways to protect a backyard garden or berry
patch is to put up a fence. A 2-foot fence with the bottom tight to the
ground or buried a few inches is sucient. However, a fence to address
multiple species such as groundhogs and raccoons will help address
other potential situations. Cylinders of 1/4-inch wire hardware cloth will
protect young orchard trees or landscape trees. The cylinders should
extend higher than a rabbit’s reach while standing on the expected
snow depth and stand 1 to 2 inches out from the tree trunk. Commer-
cial tree guards or tree wrap are another alternative.
Habitat modication:
Remove cover such as
brush piles, wood piles,
and other piled debris.
Feeding rabbits during
the winter in much the
same way as feeding
wild birds might divert
their attention from
trees and shrubs and
thus reduce damage
in some areas. There
is always the risk that
this tactic can draw
in greater numbers of
rabbits or increasing
the survival of those
present.
Frightening: Encour-
aging the rabbit’s nat-
ural enemies may aid
in reducing rabbit damage. Hawks, owls, foxes, coyotes, and snakes all
help control rabbit populations. A piece of rubber hose on the ground
may look enough like a snake to scare rabbits away. While decoys may
temporarily help, encouraging live hawks, owls, foxes, coyotes, and
snakes will have a much larger benet.
Repellents: Taste repellents are usually more eective than odor re-
pellents. Several chemical repellents, usually using thiram, discourage
rabbit browsing. Always follow the directions for application on the
container to maximize eectiveness. Some repellents are poisonous
and require safe storage and use. For best results, use repellents and
other damage control methods at the rst sign of damage. However,
most repellents are not designed to be used on plants or plant parts
destined for human consumption, so they may not be applicable to
garden issues. Taste repellents protect only the parts of the plant
they contact so new growth that emerges after appli-
cation is not protected and periodic reapplication will
be needed. Heavy rains and sprinklers may necessitate
reapplication of some repellents. Non-chemical repel-
lents such as blood meal can provide short term relief.
COTTONTAIL RABBIT
(SYLVILAGUS FLORIDANUS)
LIVE/CAGE TRAP
24 x 7 x 7
LIFE HISTORY NOTES
Mating: Polygamous
Peak Breeding Activity: April-May
Gestation: 26-28 days
Young are Born: March-September
Litter Size: 1-9; average is 5
Number of Litters per Year: Average of 3
litters a year
Seasonal Patterns: Year-round resi-
dent. Active both during day and night
throughout the entire year
Typical Foods: Clover, dandelion, plantain,
and ragweed in summer. In winter they
eat seeds, brambles, and bark of tree
saplings.

19
LAWS PERTAINING TO RACCOONS
Can be trapped or shot at any time if causing a nuisance. If trapped, can
NOT be relocated and must be released onsite or euthanized. Can NOT
be rehabilitated if injured or orphaned in specic counties.
DISEASES OF CONCERN WHEN HANDLING RACCOON
(See chapter 5 for more specic information regarding diseases)
• Rabies
• Canine distemper
• Parvovirus
• Leptospirosis
• Ascarid Roundworm
RECOMMENDED TRAP SIZES (All sizes in inches)
COMMON SITUATIONS ENCOUNTERED
• Denning under a porch, deck, or shed
• Denning in a chimney
• Denning in an attic
• Garden damage
• Eating sh in pond
• Eating chickens or other poultry
• Sod damage
• Getting into trash
• Eating food left outside for pet
• Trapped in dumpsters
TECHNIQUES FOR DEALING WITH RACCOONS
(Refer to Chapter 2 for specic information regarding these techniques)
Trapping: Raccoons are relatively easy to catch in traps, but it takes a
sturdy trap to hold one. They can be baited with marshmallows, canned
sh avored cat food, sardines, sh, or chicken. The back portion of the
trap should be tightly screened with one-half inch or smaller mesh wire
to prevent raccoons from reaching through the wire to pull out the bait.
Body-gripping traps are eective for raccoons and can be used in nat-
ural or articial cubbies or boxes and should be used in areas where
risk of non-target capture is low. Raccoons also can be captured with
foothold traps. The foot-encapsulating trap can be highly eective and
are highly-selective for raccoons. Once captured, raccoons may be re-
leased immediately at the capture site or euthanized. Trapped raccoons
cannot be relocated.
Shooting: Raccoons are seldom seen during the day because of their
nocturnal habits.
Shooting raccoons can
be eective at night
with proper lighting. A
rie of almost any cali-
ber, or a shotgun load-
ed with No. 6 shot or
larger, will eectively
kill raccoons. Check lo-
cal regulations before
discharging a rearm
within a city or village.
Exclusion: A wire
at the top of a fence
from an electric fence
charger will greatly
increase the eective-
ness for excluding rac-
coons. Where raccoons are entering homes or poultry coops ensure all
fascia and sot wood is adequately attached and that doors, vents, and
windows are properly sealed. Damage to sweet corn, watermelons, or
other garden plants can most eectively be stopped by excluding rac-
coons with a single or double hot-wire arrangement. Make sure trash is
in containers and lids are secured. Because raccoons are able to use their
front paws well, it may be necessary to wire, weight, or clamp trash can
lids down. It may also be necessary to secure cans to a rack or tie them
to a support to prevent raccoons from tipping them over. A properly
installed chimney cap will prevent raccoons from entering a chimney.
If raccoons are climbing the downspouts for access, use vegetable oil
or other slick materials to keep them from climbing. Do not complete
exclusion procedures until you are certain that all raccoons, including
young, have been removed from or have left the exclusion area.
Habitat modication: Raccoon access to rooftops can be limited by re-
moving overhanging branches and by wrapping or nailing ashing at
least 3 feet up from the base of the tree. Properly dispose of garbage
and remove other food sources such as pet food. Areas around cook-
ing grills should be cleaned regularly. Grub control may be necessary
to eliminate sod damage. Ensuring there is adequate hiding places or
shelter for sh in a pond can greatly reduce raccoons being able to grab
the sh.
Frightening: Lights and loud noise will only provide temporary relief.
Repellents: There are a few repellents commercially available to allevi-
ate chewing on structures.
Other Comments: Raccoons often nd themselves trapped in dump-
sters. Placing a board or stout tree branch in the dumpster at an angle
and giving the raccoon 24 hours to get out will allow the raccoon the
opportunity to get out.
LIFE HISTORY NOTES
Mating: Polygamous
Peak Breeding Activity: February-March
Gestation: 63-65 days
Young are Born: March-May
Litter Size: 3-7; average is 4
Number of Litters per Year: 1
Seasonal Patterns: Year-round resident;
active year-round, primarily at night and
sometimes during the day
Typical Foods: Omnivorous. Prefer ber-
ries, acorns, nestling birds, frogs, and sh
FOOTHEAD
BODYGRIP-
PING
SNARE LOOP
WITH HEIGHT
LIVE OR
CAGE TRAP
Encapsulated
(dog proof)
3 ½ -4 5/8
6 (land),
7 (part-sub-
merged)
6 – 8, 3 - 4 32 x 10 x 13
1 ½ diameter,
2 1/8 – 2 7/8
trigger depth
RACCOON
(PROCYON LOTOR)

20
LAWS PERTAINING TO SKUNKS
Can be trapped or shot at any time if causing a nuisance. If trapped, can
NOT be relocated and must be euthanized or released onsite.
DISEASES OF CONCERN WHEN HANDLING
(See chapter 5 for more specic information regarding diseases)
• Canine distemper
• Rabies
• Leptospirosis
RECOMMENDED TRAP SIZES (All sizes in inches)
COMMON SITUATIONS ENCOUNTERED
• Denning under a porch, deck, or shed
• Sod damage
• Spraying pets
• Getting into trash
• Eating food left outside for pet
TECHNIQUES FOR DEALING WITH SKUNKS
Trapping: Skunks can be caught in live traps set near the entrance to
their den. Several traps may be used when more than one animal is
present to reduce the amount of time of removal. Use canned sh-a-
vored cat food to lure skunks into traps. Other food baits such as peanut
butter, sardines, and chicken entrails are also eective. Foothold traps
should be avoided near houses or other sensitive areas because of po-
tential problem of scent discharge. When removing a trap with a skunk,
cover the trap with a tarp or other plastic and carry gently to reduce the
chance of the skunk spraying.
Shooting: A rie or another rearm may be used to dispatch a skunk.
Shooting in the back, severing the spinal cord, immediately followed by
a shot in the head may prevent the discharge of scent. However, anyone
shooting a skunk should expect a scent discharge.
Exclusion: Keep skunks from denning under buildings by sealing o
all foundation openings with wire mesh, sheet metal or concrete. Bury
fencing 1 ½ - 2 feet
where skunks can
gain access by dig-
ging. Window wells
or similar pits can be
covered with com-
mercially designed
products or with wire
mesh. Skunks nor-
mally do not climb
so even short fencing
can prove an eective
exclusion technique.
Make sure trash is in
containers and lids
are secured.
Habitat modica-
tion:
Remove cover
such as brush piles,
wood piles, and other
piled debris. Properly
dispose of garbage and remove other food sources such as pet food. Ar-
eas around cooking grills should be cleaned regularly. Grub control may
be necessary to eliminate sod damage.
Frightening: Lights and loud noise will likely only provide temporary
relief. Remember, as a natural defense skunks will spray when fright-
ened. Move slowly when around skunks to reduce the chance of them
spraying.
Toxicants and fumigants: Gas cartridges can be used to kill the skunk
in the den when used according to the label.
Other Comments: The skunk odor is persistent and dicult to remove.
Diluted solutions of vinegar, tomato juice or commercially available
products may be used to reduce or eliminate most of the odor from
people, pets or clothing. Another common method used to reduce
skunk smell is a solution of 1 quart of 3% hydrogen peroxide, ¼ cup of
baking soda, and 1 tsp of liquid soap. Clothing may also be soaked in
weak solutions of household chloride bleach or ammonia.
STRIPED SKUNK
(MEPHITIS MEPHITIS)
LIFE HISTORY NOTES
Mating: Polygamous
Peak Breeding Activity: Late February
through March
Gestation: 63 days
Young are Born: Late April through May
Litter Size: 3-10; average is 5
Number of Litters per Year: 1
Seasonal Patterns: Year-round resident;
active year-round; active primarily at night
and sometimes during the day
Typical Foods: Omnivorous. Will eat
carrion, insects, sh, crustaceans, small
mammals, fruits, grasses, buds, grains, and
nuts
FOOTHOLD BODYGRIPPING
SNARE LOOP
with HEIGHT
LIVE or CAGE
TRAP
3 ½ -4 ½ 6 4-6, 1 ½-2
24 x 7 x 7 up to
32 x 10 x 13

21
LAWS PERTAINING TO SNAKES
Only non-lethal methods may be used for the removal of nuisance
snakes. If a snake is caught, it must be released on the same property
where trapped. There are many species of snakes in Ohio and attention
must be made to determine if the snake causing the problem is endan-
gered or threatened (see chapter 3).
DISEASES OF CONCERN WHEN HANDLING SNAKES
(See chapter 5 for more specic information regarding diseases)
• Salmonelosis
RECOMMENDED TRAP SIZES (All sizes in inches)
COMMON SITUATIONS ENCOUNTERED
• In home and other structures
TECHNIQUES FOR DEALING WITH SNAKES
Trapping: Conventional traps are not legal for snakes. However, you
can make a snake funnel trap with drift fences constructed of 1/4- inch
or 1/2-inch mesh hardware cloth erected 2 feet high and 25 feet long.
One type of funnel trap can be made by rolling a 3 x 4-foot piece of 1/4-
inch mesh hardware cloth into a cylinder about 1 foot in diameter and
4 feet long. An entrance funnel can be made similarly and tted into
one end of the cylinder. Close the other end of the cylinder with hard-
ware cloth and attach the drift fence. To catch the animal from either
direction, put another funnel at the other end of the trap and another
drift fence facing the opposite direction. Glue boards have proven to be
useful for trapping snakes in or under buildings. Securely tack several
rodent glue traps to a plywood board approximately 24 x 16 inches to
make a glue patch at least 7 x 12 inches. Place the board against a wall
where snakes are likely to travel. Snakes become stuck when they try
to cross the board. Do not place the board near any object (pipes or
beams) that the snake can use for leverage in attempting to free itself. A
hole drilled through the plywood board will allow removal of the board
and the entrapped snake with a long stick or hooked pole. Animals
trapped in the glue can be removed with the aid of vegetable oil, which
counteracts the adhesive. Do not use glue boards outdoors or in any
location where they are likely to catch pets or non-target wildlife.
Shooting: It is not legal to shoot a snake.
Exclusion: It is usu-
ally best to deal with
snakes in buildings
through exclusion.
Locate the snakes
and their points of
exit or entry through
inspection, usually
around the founda-
tion of the structure.
When locating entry
and exit areas con-
sider potential as well
as active points of
access. Snakes enter
houses, barns and
other buildings when
habitat conditions
are suitable inside
the buildings. They
are particularly attracted to rodents and insects as
well as cool, damp, dark areas often associated with buildings. All open-
ings 1/4 inch (0.6 cm) and larger should be sealed to exclude snakes.
Check the corners of doors and windows, as well as around water pipe
and electrical service entrances. Holes in masonry foundations (poured
concrete and concrete blocks or bricks) should be sealed with to ex-
clude snakes.
Habitat modication: A primary food of many snakes are rodents such
as rats, mice, and chipmunks. Removing rodents and rodent habitats
can help eliminate the desire for snakes to use the area. Put all possible
sources of rodent food in secure containers. Keep all vegetation closely
mowed around buildings. Remove bushes, shrubs, rocks, boards, and
debris of any kind lying close to the ground, as these provide cover for
both rodents and snakes.
Toxicants and fumigants: None are legal.
Repellents: A few commercial repellents
are available. Most use sulphur or naph-
thalene to deter the snakes but usually
have varied results.
LIFE HISTORY NOTES
Mating: Polygamous
Peak Breeding Activity: Most from April
to June, but can vary
Gestation: Varies by species
Young are Born: Varies by species
Litter Size: Varies by species
Number of Litters per Year: One
Seasonal Patterns: Year-round resident;
will hibernate in winter (location and time
depends on species)
Typical Foods: Small rodents, insects, bird
eggs, amphibians
LIVE or CAGE TRAP
Glue traps or snake
cage trap
SNAKES

22
LAWS PERTAINING TO SQUIRRELS
Can be trapped or shot at any time if causing a nuisance. If trapped,
they can be euthanized OR relocated after receiving permission from
the landowner where it will be released. Can be rehabilitated if injured
or orphaned.
DISEASES OF CONCERN WHEN HANDLING
(See chapter 5 for more specic information regarding diseases)
• Rabies
RECOMMENDED TRAP SIZES (All sizes in inches)
COMMON SITUATIONS ENCOUNTERED
• Denning in an attic
• Denning in a chimney
• Chewing on base of small trees or on tree limbs
• Chewing on wood of home, deck, or shed
• Chewing maple sap tubing
TECHNIQUES FOR DEALING WITH SQUIRRELS
Trapping: A variety of traps will catch squirrels. Regular rat-sized snap
traps will catch ying and red squirrels. Typically, wire cage traps and
box traps are used for squirrels. Pre-bait traps and tie trap doors open
for two or three days to get squirrels accustomed to feeding in the
traps. Then set the traps and check them daily. For fox or gray squirrels,
small bodygripping traps may be utilized inside buildings or in certain
locations outside where the risk of capturing non-target species can be
minimized.
Shooting: A rie or other rearm is an eective method to kill a squirrel.
A shotgun with No. 6 shot, an air rie, or a .22-caliber rie is suitable. The
shooting of squirrels is permitted in situations where live trapping is
not practical or when not eective. It is lawful to shoot nuisance squir-
rels which cannot be live trapped because of certain conditions. Check
local regulations before discharging a rearm within a city or village.
Exclusion: Close openings to attics and other parts of buildings but
make sure not to lock squirrels inside or they may cause a great deal
of damage in their eorts to chew out. Place traps inside as a precau-
tion after openings are closed. A squirrel excluder can be improvised by
mounting an 18-inch section of 4-inch plastic pipe over an opening at a
45-degree angle. Close openings to buildings with heavy 1/2-inch wire
mesh or make oth-
er suitable repairs.
Fences topped with
electried wires may
eectively keep squir-
rels out of gardens or
small orchards. Wrap
tree trunks with ash-
ing about 4 feet from
the ground to elim-
inate squirrels from
using it to access
structures. IF squir-
rels are using a chim-
ney, installation or
repair of the chimney
cap is in order.
Habitat modica-
tion: Trim limbs and
trees to 6 to 8 feet
away from buildings
to prevent squirrels
from jumping onto
roofs. In backyards where squirrels are causing problems at bird feed-
ers, consider providing an alternative food source. Wire or nail an ear of
corn to a tree or wooden fence post away from where the squirrels are
causing problems. In high-value crop situations, it may pay to remove
woods or other trees near orchards to block squirrel access points.
Frightening: In some situations, the use of owl decoys may dissuade
the squirrel from an area. Recordings of hawks or owls may also deter
squirrels from an area. However, these are only eective for a short time
and not during nesting season to allow for repairs of holes or entrances
into the structure or installation of a chimney cap.
Repellents: A cat may discourage squirrels and should be kept on a
lead when outside. A few commercially available taste repellents that
can be applied to birdseed, bulbs, owers, trees, and shrubs. Capsaicin
(found in hot peppers such as cayenne) is also a taste repellent and can
be used on wood structures that squirrels are chewing and can even be
added to bird seed to deter squirrels. Polybutenes are sticky materials
that can be applied to buildings, railings, downspouts, and other areas
to keep squirrels from climbing. A pre-application of masking tape can
make clean up much easier.
SQUIRRELS
LIFE HISTORY NOTES
Mating: Polygamous
Peak Breeding Activity: February and
March; June and July
Gestation: 40-45 days
Young are Born: Late April or May
Litter Size: 2-4
Number of Litters per Year: 2
Seasonal Patterns: All are year-around
residents; gray, fox, and red squirrels ac-
tive primarily during the day while ying
squirrels are active at night
Typical Foods: Hickory, oak, and beech
nuts; blackberry, dogwood, cherry, and
wild grape; corn, buds of maple, elm and
willow; insects
BODYGRIPPING LIVE/CAGE TRAP
Gray and Fox Squirrel 3 ½ -4 ½ 19 x 6 x 6
Red Squirrel Rat sized snap trap 16 x 5 x 5
Flying Squirrel Rat sized snap trap 16 x 5 x 5

23
LAWS PERTAINING TO WOODCHUCKS
Can be trapped or shot at any time if causing a nuisance. If trapped,
they can be euthanized OR relocated after receiving permission from
the landowner where it will be released.
DISEASES OF CONCERN WHEN HANDLING
(See chapter 5 for more specic information regarding diseases)
• Rabies
• Ascarid roundworm
RECOMMENDED TRAP SIZES (All sizes in inches)
COMMON SITUATIONS ENCOUNTERED
• Denning under a porch, deck, or shed Garden damage
• Holes in yard or eld
• Chewing on wood of home, deck, or shed
• Eating landscape plants
TECHNIQUES FOR DEALING WITH WOODCHUCKS
Trapping: Woodchucks can be caught in live traps. Traps baited with
apple slices, broccoli, lettuce, cabbage or other vegetables that are
changed daily work best. Locate traps at main entrances or major
travel lanes. Place guide logs on either side of the path between the
burrow opening and the trap to help funnel the animal into the trap.
Groundhogs can be released on-site, outside the city or village limits
with permission of the landowner, or may be euthanized. Bodygripping
traps are eective in certain situations. Bodygripping traps are well suit-
ed for use near or under structures where shooting presents a hazard.
Bodygripping traps greater than 5 inches must be covered to prohibit
other animals and domestic pets from getting into the trap from the
outside. Traps can be enclosed with items such as welded wire, screen-
ing, boards, or boxes. Snares are also an eective means of controlling
woodchucks. Only licensed commercial nuisance wild animal control
operators are permitted to use snares without a relaxing lock for the
purpose of taking woodchucks.
Shooting: A rie or other rearm is an eective method to kill a wood-
chuck, especially when in large elds to address holes in the eld or
crop loss. Check local regulations before discharging a rearm within
a city or village.
Exclusion: Fencing is an eective tool to stop garden and landscape
damage. Fences should be at least 3 feet high. However, woodchucks
are good climbers and can easily scale wire fences. To alleviate ground-
hogs climbing over the fence you can place an electric wire 4 to 5 inches
o the ground and the same distance outside the fence. When connect-
ed to a fence charger,
the electric wire will
prevent climbing and
burrowing. Vegeta-
tion near the electric
fence should be re-
moved regularly to
prevent the system
from shorting out.
To prevent burrow-
ing under the fence,
bury the lower edge
10 to 12 inches in the
ground.
Habitat modica-
tion: Remove cover
such as brush piles,
wood piles, and other
piled debris.
Frightening: Scare-
crows and other egies can provide temporary relief
from woodchuck damage. Move them regularly and
incorporate human activity in the susceptible area.
Toxicants and fumigants: Gas cartridges can be used
to kill the woodchuck in the den when used accord-
ing to the label.
Repellents: Woodchucks will also chew on structures.
The damage can be dierentiated from squirrels be-
cause squirrel damage usually is less than 18 inches
o the ground. Placing ashing or spray with cayenne
pepper to help stop the chewing at that location. A
few repellents are commercially available to alleviate
chewing on structures.
Other comments: Woodchuck damage usually starts in one place
along the edge of the garden or crop eld and slowly radiates out
from there. The plants will show clean cuts on the plant because wood-
chucks have sharp teeth. There oftentimes is also a trail leading back to
a hole in the ground where they live or under a porch, deck, or shed. Be
mindful that there may be several woodchucks or other wild animals
using a woodchuck burrow. Care should be taken to ensure that a bad-
ger is not using the burrow. Badger holes closely resemble woodchuck
holes. Because a badger is listed as an endangered species in Ohio, care
should be taken to properly identify if one is using the hole. A hole that
a badger digs will be oval in shape and 8 to 10 inches in diameter, with
a fan-shaped mound of dirt on one side of the hole.
LIFE HISTORY NOTES
Mating: Polygamous
Peak Breeding Activity: March-May
Gestation: 31-32 days
Young are Born: April-early June
Litter Size: 2-7; average is 4
Number of Litters per Year: 1
Seasonal Patterns: Year-round resident;
hibernates in the winter; Active primarily
during the day
Typical Foods: Grasses, clover, alfalfa,
soybeans, lettuce, apples
FOOTHOLD BODYGRIPPING
SNARE LOOP
with HEIGHT
LIVE/CAGE
TRAP
No greater
than 6
5-7 4 – 6 , 2 – 3 32 x 10 x 13
GROUNDHOG (WOODCHUCK)
(MARMOTA MONAX)

24
INTRODUCTION
Many diseases aect wildlife. Some are infectious to humans while
others are more problematic for wildlife alone. As a commercial nui-
sance wildlife control operator, it is important to have knowledge about
potential diseases you may encounter when dealing with wildlife. The
following list includes the wildlife diseases you are most likely to en-
counter. Common terms:
Host- An organism negatively aected by a disease.
Vector – The route of infection of a disease.
Reservoir – An organism that harbors a disease but is not negatively
aected.
ASCARID OR RACCOON ROUNDWORM
Introduction – Raccoons are the vector of ascarid roundworms.
Clinical Signs – No known symptoms.
Diagnosis – Adult parasites can be seen in the intestinal tract of rac-
coons. Fecal otation can be used to examine feces under a microscope
for the presence of eggs.
Transmission – Adult worms present in the intestinal tract shed eggs in
the feces of raccoons. The egg then develops into a larva until they are
ingested by mammals. Once ingested, the larvae develop into adult
worms in the intestinal tract of that animal and then migrate to oth-
er organs and the central nervous system. In wild animals, the cycle is
completed when raccoons eat the carcasses of infected animals. In hu-
mans, raccoon roundworm is an end host.
Public Health Implications – The larvae of raccoon roundworms are
infectious to humans if ingested. There have been human fatalities
conrmed because of the ingestion of raccoon roundworm. Humans
should avoid contact with raccoon feces, particularly where sucient
time has elapsed for the eggs to develop to the infectious larval stage.
Rubber gloves should be worn when handling animals, when handling
traps that have contact with raccoon feces, and when handling other
material that may have contact with raccoon feces. Care should be ex-
ercised in handling infected material to not stir up dried feces. However,
aerosolized infection should be considered low risk. Hands and equip-
ment should be thoroughly washed when contact with raccoon feces
has occurred.
AVIAN CHOLERA
Introduction– Most birds and mammal species can become infected
with this bacterial disease as it has multiple strains. There is usually one
strain, Type 1, that can be found in wild birds. The most commonly af-
fected birds are ducks, geese, coots, gulls, and crows.
Clinical Signs – This disease has a sudden onset and sick birds usually
are not seen because the disease normally kills birds rapidly, resulting
in large die-os in wild ducks and geese. Body condition of the birds is
usually good. If any sick birds are present they will appear lethargic, and
when captured may die in a short period of time. Visual signs to look
for are swimming in circles, throwing head back between wings, errat-
ic ights, and mucous discharge from the mouth, and blood-stained
droppings.
Diagnosis – Look for hemorrhages on the liver, heart, intestines, and
gizzard. The liver may appear dark in color and may be swollen and rup-
ture when handled. In the upper digestive tract, food that was recently
ingested may be present, but the lower tract may contain a thick yel-
lowish viscous uid that contains the bacteria.
Transmission – Bacteria is usually transmitted by bird-to-bird contact,
contact with feces or secretions of infected birds, or ingestion of food or
water that containing the bacteria. Aerosol transmission can occur also.
The bacteria can survive in soil and water for up to four months.
Public Health Implications – Humans are not at high risk for infection,
but it is recommended to wear gloves and wash hands when handling
sick or dead birds.
AVIAN INFLUENZA
Introduction– Avian Inuenza is present in many strains. Wild water-
fowl can be carriers of the Type A virus which can be classied into two
dierent categories: low pathogenic avian inuenza (LPAI) A viruses,
and highly pathogenic avian inuenza (HPAI) A viruses. Wild waterfowl
carry the virus in their intestines and respiratory tract, but usually do
not get sick. Wild birds are viewed as hosts for this virus and it can be
spread to domesticated birds such as ducks, turkey, and chickens. Do-
mesticated birds can get very sick or even die from this virus.
Clinical Signs – In wild birds, there usually are no signs of the virus as
they are carriers of the disease.
Diagnosis – Diagnosis is made through oral or cloacal swabbing. Con-
tact your local ODNR Division of Wildlife district oce to see if the birds
qualify for testing.
Transmission – Infected waterfowl can spread the virus through nasal
secretions, saliva, and feces. Susceptible birds become infected when
they encounter the virus as it is shed by infected birds. Transmission
also occurs when a susceptible bird has contact with surfaces that are
contaminated.
Public Health Implications – Avian Inuenza Type A viruses usually do
not infect humans, but rare cases have been reported. These rare cases
have occurred after direct or close contact with infected poultry.
Chapter 5 – Wildlife Diseases
Information within this chapter was primarily obtained from the Field Manual of Wildlife Diseases in the Southeastern
United States, Third Edition by William R. Davidson
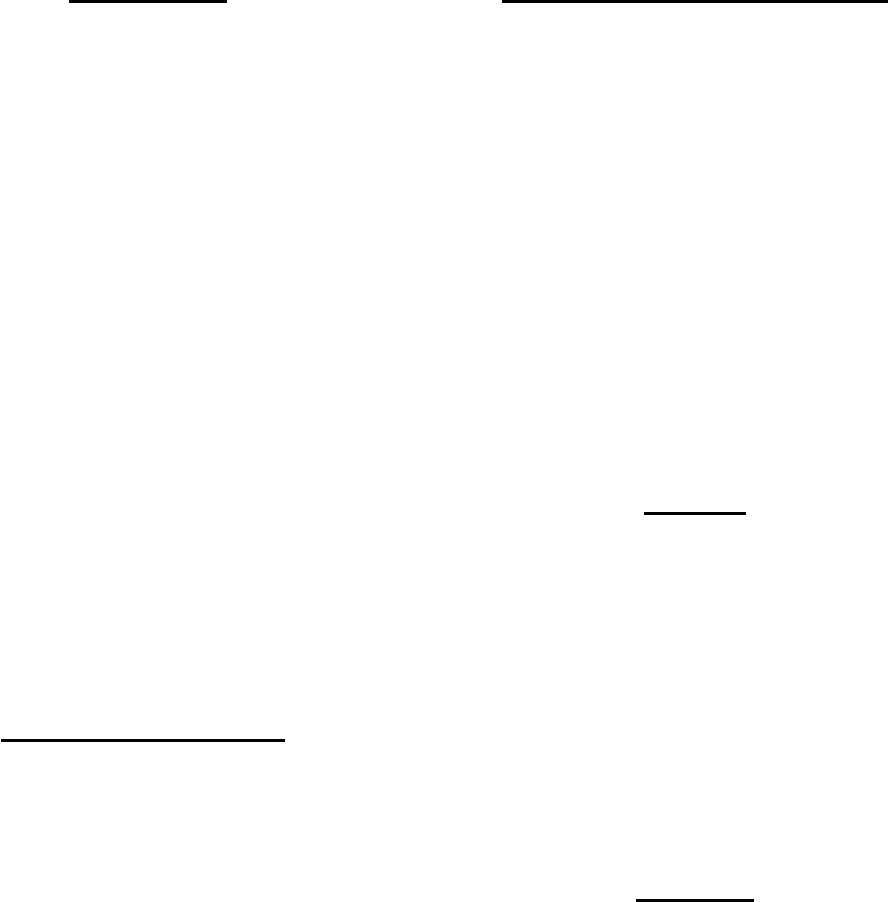
25
BOTULISM
Introduction– Botulism comes in many forms. Botulism Type C is a
common disease of waterfowl, but it can also occur in mammals or oth-
er birds. Botulism Type E is a common disease of mergansers, loons, and
gulls.
Clinical Signs – The botulism toxin produces paralysis of muscles in
animals. Often, the animal has the inability to walk or y. Because of a
paralysis of neck muscles caused by the toxin, the animal often is found
with its head laying to the side or underwater.
Diagnosis – In live birds, botulism is often suspected by visually con-
rming the clinical signs such as birds with their heads under water and
loss of coordination. In many cases there are many dead birds lying in
the water together along with some additional birds that are dying.
Suspected animals can be tested by sampling their blood either right
before death or soon after death. Most times the disease is associated
with periods of hot weather and stagnant water, and therefore animals
needing to be tested must be immediately refrigerated. Frozen samples
often impair the ability to test for the toxins.
Transmission – The bacteria grows in decaying organic matter in the
water, including dead vertebrates (such as dead waterfowl) and inver-
tebrates. Maggots on the carcasses will concentrate the toxins within
the dead animal and when eaten by other animals, passes the large
toxin concentration onto the animal eating the carcass. Recent studies
have shown that botulism spores can persist for years, leading to sub-
sequent outbreaks of the disease.
Public Health Implications – Type C botulism in humans has not been
associated with botulism in waterfowl. However, Type E botulism is
highly toxic to humans. Basic sanitary procedures should be followed
for Type C, however, if Type E is suspected contact your local ODNR Di-
vision of Wildlife district oce to determine if the birds need tested and
the proper way to handle the species aected.
CANINE DISTEMPER
Introduction – Canine distemper in Ohio is often found in foxes and
coyotes. However, raccoons and skunks are also highly susceptible to
canine distemper. Other mustelids including mink, weasel, and otter
are potentially susceptible as well.
Clinical Signs – Canine distemper is often mistaken for rabies because
the signs are similar. In addition to the signs of rabies, you will often
notice respiratory distress, coughing, sneezing, diarrhea, or discharge
from the eyes and nose which causes a crusty appearance around the
eyes or nose. You may also notice the animal having convulsions or a
loss of fear of humans.
Diagnosis –For dead animals, carcasses can be refrigerated to preserve
the specimen until contact can be made with your local ODNR Division
of Wildlife district oce to determine need to test. However, in most
cases the animal is tested for rabies as well when there has been human
or pet exposure.
Transmission – Transmission is by contact with infected animals or
their excretions or secretions such as the discharge from the eyes or
nose or urine.
Public Health Implications – Humans cannot contract canine dis-
temper, however if there has been contact with a human to a suspect
animal the same procedure should be followed for submission of the
animal for rabies testing because of the similarity in the clinical signs.
If a domestic dog has come in contact with a suspect animal and is not
current on its vaccinations, encourage the owner to contact their vet-
erinarian to describe the situation to determine the potential exposure
to the dog.
ECHINOCOCCUS INFECTION
Introduction – This is a parasite disease caused by infection from a tiny
(less than 1/8-inch long) tapeworm. Red foxes are the major host of this
tapeworm.
Clinical Signs – Red foxes that are infected normally do not show signs
of the disease.
Diagnosis – Eggs can be detected in the feces of infected foxes, but
they are impossible to distinguish from eggs of other common tape-
worms. Infected animals can be determined best at necropsy by recov-
ery and identication of adult tapeworms which can be found in the
intestine of the fox.
Transmission – Transmission can be made by accidentally ingesting
eggs shed in the feces of denitive host.
Public Health Implications – Humans are susceptible to infection by
the larval stage of E. multilocularis, which causes alveolar hydatid dis-
ease in people. When eggs that are shed from the host are accidentally
ingested, the larvae develop into large cysts that destroy the liver. Hu-
mans who have regular contact with fox or coyotes are more suscepti-
ble to this disease because eggs are immediately infectious when shed
in the feces of foxes or coyotes.
E. COLI
Introduction – Escherichia coli is a naturally occurring bacteria that can
be found in digestive tracts of warm-blooded animals.
Clinical Signs – E. coli may cause gastrointestinal problems such as
nausea, vomiting, and diarrhea when present in large amounts. Some
E. coli can even cause urinary tract infections and respiratory sickness.
Symptoms usually last for about a week or two.
Diagnosis – Typical diagnosis can be initially made by visualizations of
the clinical signs.
Transmission – E. coli is contagious and can spread easily when a per-
son does not wash their hands after handling raw food or feces.
Public Health Implications – People who are around animals should
wash their hands frequently as the bacteria can spread by handling the
animal or touching objects that are contaminated.
GIARDIA
Introduction – Beavers, muskrats, voles, coyotes, and others are sus-
ceptible to infection by protozoan parasites and are considered a host
for carrying this parasite.
Clinical Signs – Clinical signs are not reported in wild mammals, but
in humans and domestic pets, it may cause diarrhea, upset stomach,
abdominal pain, and dehydration.
Diagnosis – Diagnosis is made by microscopic examination of feces.
Transmission – Once the parasite is passed through feces of the host,
it can survive for weeks or even months. A person can become infected
by swallowing the parasite, for example by drinking contaminated wa-
ter. It cannot be passed through contact with blood.
Public Health Implications – Giardia is one of the most common wa-
terborne diseases. Most outbreaks occur from drinking contaminated
water from streams, rivers, or lakes. It is important to lter or boil any
water for drinking purposes while exploring the outdoors.

26
HANTAVIRUS
Introduction – Rodents are the primary reservoir hosts of Hantavirus.
The deer mouse is likely the principal reservoir in Ohio, however the
white-footed mouse could also be a reservoir. Ultimately, all rodents
likely have the potential for carrying the viruses.
Clinical Signs – Human infection with some Hantavirus causes an acute,
severe respiratory disease in which aected patients have diculty
breathing because of rapid uid build-up in the lungs. Rodents are as-
ymptomatic carriers and do not show any clinical signs when infected.
Diagnosis – Diagnosis of hantavirus is made by looking for antibodies
in the serum of patients or by demonstrating hantavirus antigen or RNA
in tissues.
Transmission – Human infection occurs when virus particles aerosol-
ized from rodent urine, feces, or saliva are inhaled. Transmission is also
possible from handling rodents.
Public Health Implications – Residents of houses with heavy rodent
infestation or workers who have frequent contact with rodents such
as commercial nuisance wildlife control operators have a higher risk
of infection. However, the overall risk of infection with Hantavirus is
considered low. You should use safety precautions such as use of a half-
face air-purifying lter, rubber gloves when handling traps and rodents,
disinfection of supplies, and proper disposal of carcasses.
HISTOPLASMOSIS
Introduction – While wild animals are not directly responsible for
spreading histoplasmosis, animals, especially birds and bats, are re-
sponsible for creating an enriched organic environment in their fecal
droppings that allows the fungus to grow as a mold.
Clinical Signs – Flu-like symptoms with respiratory involvement is the
most common problem in humans.
Diagnosis – Anytime you are working in large areas of bird feces or bat
guano you should assume the fungus is present. Conrmation of its
presence can be made in a laboratory under microscope.
Transmission – Histoplasmosis is not transmissible from human to hu-
man. Transmission occurs when the spores of the fungus are inhaled
either physically or aerially when working around large amounts of bird
feces or bat guano.
Public Health Implications – Up to 80 percent of people become in-
fected with histoplasmosis with an average of 90 percent of infections
in people with normal immune systems going without symptoms. In
some rare cases severe systemic disease can occur. When in areas of po-
tential histoplasmosis such as large quantities of bird feces or bat gua-
no, preventative measures such as minimizing disturbance of the feces
or guano and wetting it before removal as well as use of an appropriate
protective face mask is suggested. Areas can be decontaminated with
the use of household chlorine bleach solution containing 5 percent so-
dium hypochlorite.
LEPTOSPIROSIS
Introduction – This disease can be found any in a wide variety of wild
mammals. It is caused by members of the bacterial species Leptospira
interrogans, which is represented by more than 180 serologically dis-
tinct varieties.
Clinical Signs – Most wild animals have not been studied for signs of
leptospirosis, but isolation from clinically normal animals show very lit-
tle to any signs.
Diagnosis – Diagnosis can be made by using uorescent antibody
staining of fresh tissues. Serologic testing of blood for antibodies can
also be used on wild animals for leptospiral infection. Preferred diag-
nostic specimens are a live animal or fresh tissues such as a kidney,
blood serum, or tissues preserved in 10 percent buered formalin.
Transmission – Organisms can last a long length of time in alkaline
waters or moist soils. Ingesting water or food contaminated with urine
from an infected animal is the primary route of transmission.
Public Health Implications – Humans who are infected with leptospiro-
sis can have unapparent to severe disease with fatalities. Clinical signs
usually result in fever, headaches, weakness, and vomiting. Severe cases
can include meningitis, renal failure, and death. Sources of organisms
can be water, soil, or infected animals.
LYME DISEASE
Introduction – Rodents, especially the white-footed mouse in Ohio, are
the primary reservoir for the disease. All mammals are considered hosts
for the black-legged ticks. There is even evidence that birds and reptiles
can also be considered hosts for Lyme disease.
Clinical Signs – Clinical signs of Lyme disease in an animal typically is
neurologic impairment. There is usually a red rash that appears at the
bite site and the rash may spread out to 5 inches or more from the site
of the bite. The animal usually exhibits u-like symptoms as the spiro-
chete spreads.
Diagnosis – Diagnosis
is typically made by a
physician through
sampling of blood.
Transmission – Trans-
mission occurs when
an animal is bitten
by an infected black-
legged tick and the
tick passes the spiro-
chete onto the ani-
mal. When the host is
bitten by the larvae or
nymph stage of the
blacklegged tick, it
passes the spirochete
onto the tick. The tick then in turn passes the spirochete onto the next
host.
Public Health Implications – Humans and animals in areas where the
blacklegged tick exists should consider themselves susceptible to get-
ting bit especially in areas of mid-height grass and shrubs. However,
the disease is treatable in the early stages with antibiotics. If you de-
velop a rash from the area of a tick bite you should contact your phy-
sician immediately. When possible, it is important to use insect or tick
repellents, tuck pant legs into socks, and frequently search for and ap-
propriately remove the ticks when in areas of known populations of
blacklegged ticks.

27
PARVOVIRUS
Introduction – There are two main carriers of parvovirus in Ohio, rac-
coons and coyotes.
Clinical Signs – Common signs of the parvovirus in animals is diarrhea,
dehydration, and depression followed rapidly by death. Also, the intes-
tines of the animal are often reddened.
Diagnosis – Initial diagnosis can typically be made by visualization of
the clinical signs of an animal. Conrmation can be made by submit-
ting refrigerated fresh intestines for sampling.
Transmission – Transmission from animal to animal is typically through
contact with infected feces. The virus is very stable in the environment
and can persist for several weeks in fecal material.
Public Health Implications – There are no known human health con-
cerns with parvovirus. However, with the canine parvovirus that is car-
ried by coyotes, there is a possibility for transmission to domestic dogs.
There is a pre-exposure vaccination for domestic dogs that will prevent
transmission to them. Owners that notice that their unvaccinated dogs
have eaten or come in contact with coyote feces should contact their
veterinarian.
RABIES
Introduction –In Ohio, raccoons, skunks, and bats are the primary vec-
tor species of rabies. However, all mammals are susceptible to rabies
including humans. Birds are not capable of contracting rabies.
Clinical Signs – Animals with rabies typically have marked changes
from normal behavior. Common signs rabies are aimless wandering,
lethargy, lack of coordination, and paralysis. Less frequent, animals be-
come viscous at any moving object and often leads to self-mutilation.
Diagnosis – Diagnosis of the virus cannot be made on a live animal.
Trapped wildlife suspected of having rabies should be killed without
damage to the brain, double bagged, and contact with the local health
department should be made by the next business day.
Transmission – The primary way the rabies virus is transmitted is by the
bite of an infected animal or by exposure to open wounds of the saliva
or bodily uids of an animal.
Public Health Implications - In cases where there has been contact
with a human or a pet and rabies is a possibility, especially when there
has been contact with raccoons, skunks, or bats you should insist the
person contact their local health department by the next business day
with a history of who and what has had contact with the animal. Rubber
gloves should be used to handle the animals. Human and pet exposure
to rabies should be treated seriously. Once symptoms of rabies start
showing, the disease is almost always 100 percent fatal for the human
or pet. Pre-exposure vaccination is available through your doctor and is
strongly encouraged for those who routinely handle wild animals (such
as commercial nuisance wild animal control operators).
SALMONELLOSIS
Introduction – Almost any animal can be a host for salmonellosis. How-
ever, birds and reptiles tend to be the primary vectors for transmission
to humans.
Clinical Signs – Clinical signs of salmonellosis in wildlife can be dicult
to notice, but can sometimes be recognized when an animal is having
diculty swallowing, loss of appetite, or intense thirst. In humans it
causes diarrhea, acute gastroenteritis, or meningitis.
Diagnosis – This disease is often suspected when several dead birds
are found in an area and when, based on observations, conjunctivitis is
ruled out. However, conrmation can be made by culturing the bacte-
ria in a laboratory from samples of the liver or spleen from refrigerated
carcasses.
Transmission – Transmission primarily occurs when handling individu-
als infected with the bacteria. However, objects that come in contact
with infected animals, such as bird feeders, can also harbor salmonel-
losis and provide a method of transmission to other animals including
humans.
Public Health Implications – Humans and animals are highly suscep-
tible to salmonellosis and proper hand washing as well as washing of
equipment such as cages and bird feeders with hot soapy water will
greatly reduce the spread of the bacteria.
SARCOPTIC MANGE
Introduction – The causative agent leading to the clinical signs are
mites. There are many types of mange and in most cases, mange mites
are species specic. Sarcoptic mange occurs in red fox and coyotes but
can also be passed to domestic dogs. Notoedric mange occurs in gray
and fox squirrels.
Clinical Signs – Animals with mange spend an inordinate amount of
time scratching, chewing, or licking infected skin. The skin of animals
with mange will often have a crusty appearance which is a result of
the scratching or chewing. Signicant hair loss is usually also seen on
animals with mange. At times, animals can appear weak or emaciated,
especially when infected during the winter months.
Diagnosis – A typical diagnosis is made by visualizing clinical signs of
the mite’s presence. Conrmation of the disease can be made by view-
ing skin scrapings under a microscope to look for the mites.
Transmission – Transmission from one animal to another is made when
direct contact is made
with an infected animal.
The mite itself will not kill
the animal. However, the
open wounds caused by
the scratching or chew-
ing can lead to infection,
sometimes causing the
animal to become sick or
die. In addition, animals
with severe hair loss in the
winter may become sus-
ceptible to hypothermia
and die from exposure to
the harsh winter elements.
Public Health Implications
– Humans cannot become
infected with either of these
types of mange through
colonization of the mites.
However, it is possible if
the mites are on a human
for that person to experience severe itching when regularly handling
mangy animals.
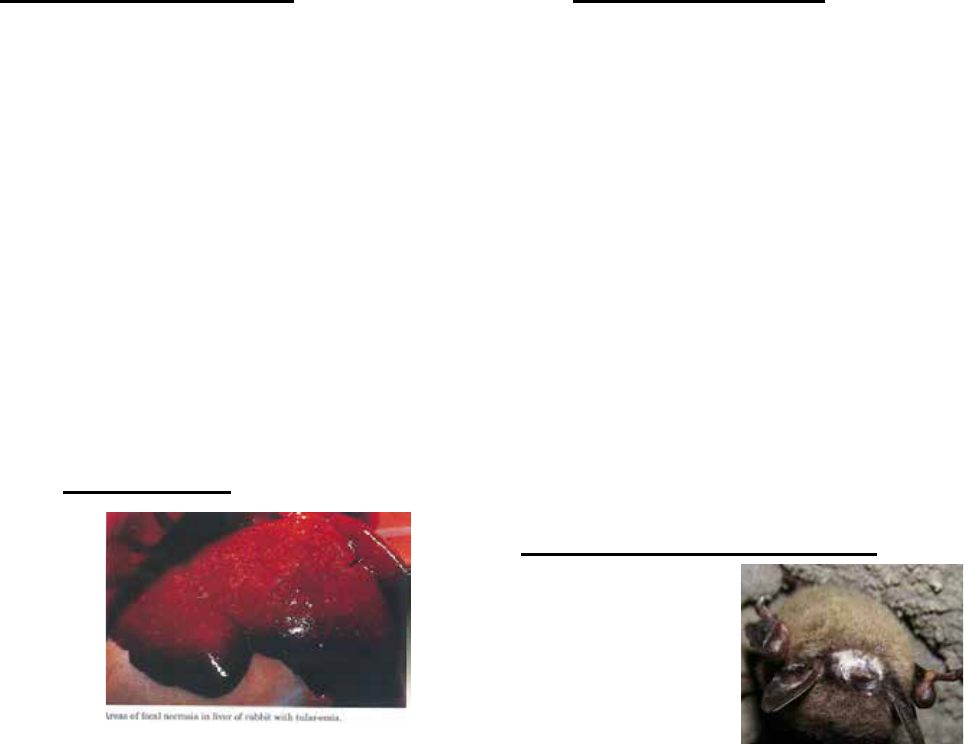
28
STAPHYLOCOCCOSIS
Introduction – Staphylococcosis is a common bacteria found on the
skin and membranes of most animals. It can occasionally be found in
wild rabbits. Caution should be given especially when the person han-
dling an animal has lesions or cuts that may come into contact with the
animal.
Clinical Signs – Clinical signs are not specic although listlessness,
emaciation, and lameness may occur in rabbits.
Diagnosis – Diagnosis is made by examination of the lymph nodes,
blood, or organs from a fresh dead animal with gross lesions. Carcasses
should be refrigerated and preferably not frozen.
Transmission – Biting arthropods such as ticks or eas may produce lo-
calized tissue damage and allow invasion of the bacteria. Transmission
can also occur when a lesion or cut comes into contact with the bacteria
on the animal.
Public Health Implications – Rabbits with staphylococcosis should not
be consumed due to the fact that lesions resemble tularemia. Tularemia
can have signicant human signicance. Properly washing hands after
handling a wild animal will help reduce the potential for transmission.
TULAREMIA
Introduction – The most
common carriers of tulare-
mia are cottontail rabbits and
rodents such as beavers and
muskrats.
Clinical Signs – Clinical signs
of wildlife with tularemia are
often variable and often go
unnoticed. With live animals
they may become lethargic
or show incoordination. Most
times tularemia is detected
with dead animals. On dead animals, the liver and spleen can have pin-
point white spots on them. In humans, tularemia typically manifests in a
fever, infected sores at the point of entry of the disease, swollen lymph
nodes, and general u-like symptoms that progresses rapidly to debili-
tation.
Diagnosis – Diagnosis can initially be made by noticing the pinpoint
white lesions on the liver and spleen.
Transmission – Tularemia has been found to be transmitted by all known
epidemiologic routes. With terrestrial animals, the transmission is typi-
cally through eas and ticks being passed from one animal to the next.
In aquatic mammals the organism is thought to be primarily waterborne.
Public Health Implications – Tularemia is a life-threatening human
disease and extreme caution should be used when handling animals,
especially cottontail rabbits, beavers, muskrats, and other rodents. Any-
one with potential exposure, especially in conjunction with exhibiting
symptoms, should contact their physician immediately. With prompt an-
tibiotic treatment, few cases are fatal. Fortunately, tularemia is not well
documented in Ohio, but all precautions should be taken when handling
species considered as a vector or in areas where it has been documented.
WEST NILE VIRUS
Introduction – The primary hosts of West Nile Virus are birds. However,
mammals, including humans, and even reptiles can contract the virus.
Clinical Signs – Clinical signs can range from unnoticeable to dead ani-
mals but is variable depending on the species. Some animals will exhib-
it lethargic behavior, lack of coordination, or unresponsiveness.
Diagnosis – A conrmation diagnosis cannot be made by visual signs,
however there are several ways to sample for the virus. Diagnosis con-
rmation in Ohio is only needed when a large number of birds in a par-
ticular area are found dead.
Transmission – Transmission is primarily through bites from mosquitos,
primarily of the Culex genus. However, there have been some studies
that have shown transmission by direct contact with some bird species.
Public Health Implications – West Nile Virus primarily aects birds.
However, humans are susceptible to the disease. In most cases, humans
contract the virus from being bitten by an infected mosquito. Because
there is a possibility of direct transmission from birds, care should be
taken to not handle potentially infected dead birds with bare hands.
Also, care should be taken when working in environments of stagnant
water, which is a common breeding area of the Culex mosquitos, by
using mosquito repellent products or wearing long sleeves and pants,
especially during sunset when the mosquitos become very active.
WHITE-NOSE SYNDROME
Introduction– White-nose syndrome
(WNS) is named for the white fungus
observed growing around the noses of
aected bats. This aggressive fungus
attacks the exposed skin of bats while
they hibernate, resulting in dehydra-
tion, unrest, and increased activity. Af-
fected bats quickly burn through stored
energy and often die in the caves and
mines where they hibernate, or out on
the landscape. Since its discovery, WNS has been conrmed in 27 states
(including Ohio) and Canada. Over 6 million bats have died as a result of
this disease, which continues to spread. As a result of the drastic popu-
lation declines caused by WNS, it has become increasingly important to
reduce other sources of bat mortality. Spores of the fungus that causes
WNS can remain on materials and be transported from one location to an-
other. Decontamination protocols should be followed to reduce the risk of
transmission of the fungus to other bats and locations.
Clinical Signs – Bats with white-nose syndrome are characterized by the
following: white fungus on the body, bats ying outside during the day in
very cold temperatures, bats clustered near the entrance of hibernacula,
or dead and dying bats during winter months.
Diagnosis – A presumptive diagnosis can be made by a bat exhibiting
any of the clinical signs. However, a conrmative diagnosis must be done
in a lab.
Transmission – The fungus often grows into white tufts on the muzzles
of infected bats. The fungus infects the exposed epidermis on bat’s skin
during hibernation, which ultimately causes the death of the bats infect
-
ed. Bats infected with WNS transmit the disease and spores to other bats
through direct contact with each other. However, experts believe humans
can carry the spores that cause WNS on their clothing from contaminated
sites which increases the spread of the disease. Anything that comes into
contact with a bat should be disposed of in the trash or decontaminated
according to the most recent national decontamination protocols avail-
able at whitenosesyndrome.org. The most common items that require
disposal or decontamination include cones, tubes, chutes, and mesh that
are used to construct one-way doors.
Public Health Implications – White-nose syndrome does not aect hu
-
man health. However, extreme caution should be taken to eliminate
transmission on equipment and clothing to eliminate the spread from
one location to another.

29
Center for Disease Control - cdc.gov
Internet Center for Wildlife Damage Management – icwdm.org Ohio Department
of Health – odh.ohio.gov
Ohio Division of Wildlife – wildohio.gov
MI Wildlife Disease Manual - http://michigan.gov/dnr/0,1607,7-153-
10370_12150_12220---,00.html
White-Nose Syndrome – whitenosesyndrome.org
ADDITIONAL RESOURCES FOR DISEASE INFORMATION
30
Chapter 6 – Ethics of Commercial Nuisance Wild
Animal Control Operations
Ethics, although not regulated, could impact the future of the commercial nuisance wild animal control op-
erators not only in Ohio, but nationwide. An unethical action by one operator may result in negative feelings
towards the industry and may lead to legislation, locally or statewide, that takes away the ability to perform
these services. Perception sometimes means everything. A good rule to follow is to act as if your actions will
be viewed on the evening news and think, “How would someone watching the evening news think I am
acting?” The following considerations should be made when performing nuisance wild animal control work:
Consider the safety of other people and pets that may come into contact with your traps. Not everyone is
familiar with trapping and homeowners often do not fully understand how traps work. You should take any
opportunity to show a landowner how a trap operates and abate any fears the homeowner may have as well
as showing them where your traps are set.
Animal care should be given a high priority.
Once you set a trap, you take on the responsibility of care for any animal that goes in the trap, both wild and
domestic. Many homeowners don’t regularly deal with wild animals. While it is easy for you as a professional
to become complacent when dealing with animals, it is important to stay vigilant in taking the best care
possible of any animals that you handle. This responsibility also extends to carrying animals in traps to your
vehicle for removal and when using equipment for handling wild animals such as catch-poles and nets.
Handling animals requires consideration of the safety of the handler, minimizing pain and distress to the
animal and public perception.
You are viewed as the expert.
It is important to not take advantage of homeowners by charging them for services that are not needed or
using scare tactics to secure a job.
Be up front, open, and honest.
It is important to be up front, open, and honest with the landowners as well as adjacent property owners.
Not everyone has the same views of trapping. Explaining why the need for nuisance trapping exists can go
a long way to people understanding the reasons for what you are doing. Also, be honest with homeowners
and the public about what you are doing. For instance, it is better to explain why you cannot relocate a
raccoon because of disease concerns rather than telling them you will relocate it and then euthanizing it.
Be courteous to other trappers.
Nuisance trapping is a necessary service to deal with animals that regulated trapping cannot address, such
as a nesting raccoon in the springtime when trapping season is out. It is important to be respectful of the
fact that regulated trapping is also an important economic industry. It is also important to be courteous to
other commercial nuisance wild animal control operators. Instead of speaking poorly about another person
or company, explain the positive practices you and your company follow.
Continue to develop your knowledge and skills.
New techniques are constantly being developed and new equipment is constantly becoming available. In
contrast, some techniques and equipment may, over time, not be the best methods to use. It is important to
actively educate yourself about the most currently accepted and available options for nuisance wild animal
control operators. There are many options including magazines, workshops, and conferences to stay current
with the most up-to-date methods and technology.
Be professional.
Always make a good rst impression. This will help you gain work through referrals and repeat customers,
and shows all commercial nuisance wild animal control operators in a good light. It is not appropriate to use
profanity when on a job site. Be considerate in comments that are made regarding the euthanasia of ani-
mals. You may be recorded or video-taped. You should also strive to keep a clean, professional appearance.
It is also important to make sure all your equipment is in proper working order.
Be complete when working on a job.
You should ensure that when you are done with a nuisance wild animal job that there is little likelihood of
the homeowner experiencing the problem again. Finishing the job with proper exclusion techniques or
properly stopping access is important. If you are not able to complete a job (such as repair siding), direct the
homeowner to a person that can perform the necessary work. In addition, follow up with the homeowner to
ensure that the work was completed. A follow up call can go a long way to getting future business.
