
Currently, about 55% of the civilian pilots in the United States
must utilize some form of refractive correction to meet the vision
requirements for medical certi cation. While spectacles are the most
common choice for aviators, recent studies show a growing number
of pilots have opted for refractive surgical procedures, which include
laser refractive surgery. The information in this brochure describes
the bene ts as well as possible pitfalls laser refractive surgery offers
to those considering these procedures.
What is Refractive Error?
Refractive error prevents light rays from being brought to a single
focus on the retina resulting in reduced visual acuity. To see clearly,
refractive errors are most often corrected with ophthalmic lenses
(glasses, contact lenses). The three principal types of refractive
conditions are myopia, hyperopia, and astigmatism. Another
ophthalmic condition that also results in blurred near vision is called
presbyopia. Presbyopia is a progressive loss of accommodation
(decreased ability to focus at near distance due to physiological
changes in the eye’s crystalline lens) that normally occurs around 40
years of age. Bifocals or reading glasses are necessary to correct this
condition.
Myopia (nearsightedness, distant objects appear fuzzy) is a condition
in which light rays are focused in front of the retina. About 30% of
Americans are myopic.
Hyperopia (farsightedness, near objects appear fuzzy) is a condition
in which light rays are focused behind the retina. An estimated
40% of Americans are hyperopic. However, this number may not
be accurate. Young hyperopes (< 40 years), who can compensate
for their farsightedness with their ability to accommodate, are often
not counted in this number and some studies incorrectly include
presbyopes, who also require plus power lenses to see clearly.
Astigmatism is a condition often caused from an irregular curvature
of the cornea. As a result, light is not focused to a single image on the
retina. Astigmatism can cause blurred vision at any distance and may
occur in addition to myopic or hyperopic conditions. Approximately
60% of the population has some astigmatism.
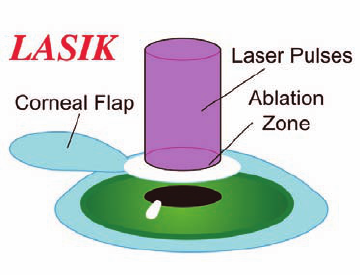
What is Laser Refractive Surgery?
In October 1995, the Food and Drug Administration (FDA) approved
the use of the excimer laser to perform a refractive procedure
called Photorefractive Keratectomy (PRK). PRK improves visual
acuity by altering the curvature of the cornea through a series of
laser pulses. The laser photoablates (vaporizes) the corneal tissue
to a predetermined depth and diameter. PRK can be used to correct
myopia, hyperopia, and astigmatism. Reported PRK problems such
as postoperative pain, prolonged healing period, increased risk of
infection, and glare (halos) at night, has resulted in Laser in situ
Keratomileusis (LASIK) becoming the preferred choice for refractive
surgery by patients and eyecare practitioners. A survey in the United
States found that the percentage of refractive surgeons performing
PRK had decreased from 26% in 1997 to less than 1% in 2002.
LASIK is performed using two FDA approved devices: the
microkeratome and excimer laser. During the LASIK procedure, the
microkeratome slices a thin ap from the top of the cornea, leaving
it connected by a small hinge of tissue. The corneal ap is folded
aside and the excimer laser is used to reshape the underlying corneal
stroma. The ap is then returned to its original position.
Is LASIK an Option for Me?
An eye care specialist should thoroughly evaluate your current
ocular health and correction requirements to determine whether you
are a suitable candidate for refractive surgery. Clinical trials have
established the following selection criteria for LASIK.
Selection Criteria:
4 Age 18 years or older
4 Stable refractive error (less than .50 diopters [D] change within
the last year) correctable to 20/40 or better
4 Less than - 15.00 D of myopia and up to 6 to 7 D of astigmatism
4 Less than + 6.00 D of hyperopia and less than 6 D of
astigmatism
4 No gender restriction, with the exception of pregnancy
4 Pupil size less than or equal to 6 mm (in normal room lighting)
4 Realistic expectations of nal results (with a complete
understanding of the bene ts, as well as the possible risks)
In addition to conforming to the above criteria, it is important that you
possess normal ocular health and be free of pre-existing conditions
that may contraindicate LASIK.
Contraindications:
4 Collagen vascular disease (corneal ulceration or melting)
4 Ocular disease (dry eye, keratoconus, glaucoma, incipient
cataracts, herpes simplex keratitis, corneal edema)
4 Systemic disorders (diabetes, rheumatoid arthritis, lupus, HIV,
AIDS)
4 History of side effects from steroids
4 Signs of keratoconus
4 Use of some acne medication (e.g., Accutane and/or Cordarone)

Is LASIK Safe for Pilots?
Aviators considering LASIK should know that in initial FDA trials
reporting high success rates (> 90%) and low complication rates (<
1%), the criteria for success varied. In most clinical studies, success
was de ned as 20/40 or better distant uncorrected visual acuity
(UCVA) under normal room lighting with high contrast targets, not
20/20 or better UCVA. While the majority of patients do experience
dramatic improvement in vision after laser refractive surgery,
there is no guarantee that perfect UCVA will be the nal outcome.
Even successful procedures may leave many patients with a small
amount of residual refractive error that requires an ophthalmic
device (eyeglasses or contact lenses) to obtain 20/20 visual acuity. If
overcorrection results, patients may need reading glasses.
Compared to its predecessor (PRK), LASIK requires higher technical
skill by the surgeon because a corneal ap must be created. Although
rare, loss of best corrected visual acuity (BCVA) can occur when there
are surgical complications such as those summarized below.
Surgical Complications:
4 Decentered or detached corneal ap
4 Decentered ablation zone
4 Button-hole ap ( ap cut too thin resulting in a hole)
4 Perforation of the eye
Operation of an aircraft is a visually demanding activity performed
in an environment that is not always user friendly. This becomes
particularly evident if the choice of vision correction is ill-suited for
the task. While the risk of serious vision-threatening complications
after having LASIK is low
(< 1%), some complications
could have a signi cant impact
on visual performance in a
cockpit environment.
Relative Risk of Post-Surgical Complications:
4
4
4
4
4
4
4
4
4
Prolonged healing periods: 3 months or more
Night glare (halos, starbursts): 1 in 50
Under/over-correction: less than 1 in 100
Increased intraocular pressure: non signi cant
Corneal haze: 1 in 1,000
Corneal scarring: non signi cant
Loss of BCVA: 1 in 100
Infection: 1 in 5,000
Corneal ap complications (dislocated ap, epithelial ingrowth):
less than 1 in 100
Following LASIK, patients are cautioned to avoid rubbing their eyes
and to stay out of swimming pools, hot tubs, or whirlpools for at
least a week. Contact sports should be avoided for a minimum of 2
weeks, and many eye surgeons recommend wearing safety eyewear
while playing sports. Even after the patient’s vision has stabilized and
healing appears complete, the corneal ap may not be completely re-
adhered. There have been reports of corneal ap displacement due to
trauma up to 38 months after the procedure.
After surgery, patients are cautioned to not wear eye makeup or use
lotions and creams around their eyes for a minimum of 2 weeks and
to discard all previously used makeup to reduce the risk of infection.
In some instances, LASIK may be an option for patients with higher
refractive error than can be safely corrected with PRK or those with
conditions that can delay healing (e.g., lupus, rheumatoid arthritis).
Since LASIK minimizes the area of the epithelium surgically
altered, it reduces some of the risks associated with delayed healing.
Additionally, ablation of the underlying stromal tissue results in less
corneal haze and the tendency for the cornea to revert back to the
original refractive condition during the healing process (refractive
regression), which improves predictability. Most patients do not
require long-term, postoperative steroid use, decreasing the possibility
of steroid-induced complications (cataract, glaucoma).
As with any invasive procedure, there are surgical risks, and the
recovery process often varies with each individual. Post-LASIK
patients report experiencing mild irritation, sensitivity to bright light,
and tearing for a few days after surgery. For most, vision stabilizes
within 3 months to near-predicted results, and residual night glare
usually diminishes within 6 months. In rare cases, symptoms have
lingered longer than a year. Earlier versions of LASIK used a smaller
ablation zone which sometimes resulted in glare problems at night.
Ablation zones have an area of transition between treated and
untreated corneal tissue. As the pupil dilates and becomes larger than
the ablation zone, light (car headlights, streetlights, and traf c signals
lights) entering through these transition areas becomes distorted,
resulting in aberrations perceived as glare. These patients often
complain of dif culties seeing under low-light conditions.
Patients that develop postoperative haze during the healing process
have complained of glare (halos and starbursts). Furthermore, it has
been reported that exposure to ultraviolet radiation or bright sunlight
may result in refractive regression and late-onset corneal haze. It
is therefore recommended that all refractive surgery patients wear
sunglasses with UV protection and to refrain from using tanning beds
for several months after surgery.
For those with larger amounts of refractive correction, the
predictability of the resulting refractive correction is less exact.
This can lead to under-correction (requiring an additional laser
enhancement procedure and/or corrective lenses) or over-correction
of the refractive error. In the case of overcorrection, premature
presbyopia and the need for reading glasses can result.
It has been reported that there can be a slower recovery of BCVA and
UCVA with hyperopic LASIK compared with those having myopic
LASIK. This is especially true for older patients who may be even
less likely to achieve UCVA of 20/20 or better. (Note: Loss of BCVA
is reportedly 5 to 15 times more likely with refractive surgery than
from the use of extended-wear contact lenses.)
Older patients with presbyopia may opt for monovision LASIK,
which corrects the dominant eye for distant vision and the other
eye for near vision. The procedure is intended to eliminate the need
for a patient to wear corrective lenses for near and distant vision.
Anisometropia (difference in correction between the eyes) induced
by monovision may result in decreased binocular vision, contrast
sensitivity, and stereo acuity. After an adaptation period, patients are
often able to see and function normally. Patients who report blurred
vision, dif culty with night driving, and other visual tasks in low-light
conditions typically do not adapt to monovision and may require an
enhancement on their non-dominant eye so that both eyes are fully
corrected for distant vision. Airmen who seek monovision correction
should consult an eye care practitioner to assist them in compliance
with standards outlined in the “Guide for Aviation Medical Examiners
(see below):
Airmen who opt for monovision LASIK must initially wear correction
(i.e., glasses or contact lens) for near vision eye while operating an
aircraft. After a 6-month period of adaptation, they may apply for a
Statement of Demonstrated Ability (SODA) with a medical ight test.
If the airman is successful, the lens requirement is removed from their
medical certi cate.
Advances in Refractive Surgery
Wavefront LASIK
Eye care specialists have traditionally used standard measurement
techniques that identify and correct lower-order aberrations, such as
nearsightedness, farsightedness, and astigmatism. However, no two
people share the same eye irregularities or have similar refractive
needs. Vision is unique and as personal as ngerprints or DNA.
Wavefrontontont technology allows eye surgeons to customize the LASIK
procedure for each eye, providing the possibility of even better vision.
The FDA approved the rst system for general use in October 2002.
A laser beam is sent through the eye to the retina and is re ected
back through the pupil, measuring the irregularities of the light wave
(wavefront) as it emerges from the eye. This process produces a three-
dimensional map of the eye’s optical system. Measuring the cornea’s
imperfections or aberrations in this way allows the refractive surgeon
to develop a personalized treatment plan for the patient’s unique
vision needs. Correcting the patient’s speci c imperfections can result
in sharper vision, better contrast sensitivity, and reduces problems
associated with higher-order aberrations after surgery, such as haloes
and blurred images. Studies indicate that 90-94% of patients receiving
technology allows eye surgeons to customize the LASIK

wavefront LASIK achieved visual acuity of 20/20 or better. However,
those with thin corneas, high degrees of aberrations, severe dry eyes,
or conditions affecting the lens and vitreous uid inside the eye may
not be good candidates for wavefront LASIK.
Other Advances in Refractive Surgery
The eye’s optical system creates a limit as to how wide and deep the
laser ablation should be, i.e., the wider the ablation, the deeper the
laser must ablate into the cornea, which may result in delayed healing
and prolonged visual recovery. The development of new lasers allows
the creation of a wider ablation zone while removing the least amount
of tissue. Studies have shown that this reduces problems with night
vision and other side effects associated with laser refractive surgery.
Laser technology that provides variable optical zone sizes and beam
shapes with scanning capabilities allows the eye surgeon greater
exibility in developing a more personalized laser vision procedure.
A spot laser may be adjusted so minimal spherical aberrations are
produced and a larger optical zone is created. Results from clinical
trials indicate that 67% of eyes had UCVA of 20/16 or better and 25%
had 20/12.5 or better. Additionally, there was an overall improvement
in nighttime visual function and night driving, which is achieved by
preserving the optical zone size and better shaping of the ablation
pro le.
During traditional LASIK, the corneal ap is created with a
mechanical microkeratome manipulated by the surgeon’s hand.
While this method has worked well over the years, the performance
of these devices can be unpredictable and is the source of a majority
of surgical complications. These dif culties result in irregularities in
thickness between the central and peripheral areas of the ap that can
induce postoperative astigmatism.
The IntraLase Femtosecond Laser Keratome, which received FDA
approval in December 1999, is the rst blade-free technology for
creating the corneal ap. The laser keratome beam passes into the
cornea at a predetermined depth, producing a precise cut that is
reportedly more accurate than the microkeratome. Corneal aps made
with the laser keratome appear to adhere more tightly to the corneal
bed at the end of the procedure, which may eliminate problems with
long-term ap displacement. A reported disadvantage to this new
technology is that surgical time is increased, leaving the stroma
exposed several minutes longer, which has led to reported complaints
of photophobia and eye irritation for up to two days after surgery.
While it may take longer (4 to 7 days) to recover good vision, the
approach appears to be associated with a lower incidence of dry eyes,
corneal complications, and enhancement procedures compared with
traditional LASIK.
The FAA requires that civil airmen with refractive surgical procedures
(e.g., PRK, LASIK) discontinue ying until their eyecare specialist
has determined that their vision is stable and there are no signi cant
adverse effects or complications. The airman should submit one of
two documents to the FAA (a report from their eyecare specialist or
“Report of Eye Evaluation” [FAA-8500-7]). These reports can be
submitted directly to the Aerospace Medical Certi cation Division
when released from care, or to their Aviation Medical Examiner
during their next ight physical. This report should state:
“. . . . that the airman meets the visual acuity standards and the
report of eye evaluation indicates healing is complete, visual acuity
remains stable, and the applicant does not suffer sequela, such as
glare intolerance, halos, rings, impaired night vision, or any other
complications. . . .” (Guide for Aviation Medical Examiners, July
2005)
If you are a pilot contemplating refractive surgery, consult an eyecare
specialist to determine if you are a good candidate for laser refractive
surgery. Although the FAA and most major air carriers allow laser
refractive surgery, professional aviators should consider how it
could affect their occupational and certi cation status. As with any
invasive procedure, there are many variables that can in uence the
nal outcome. You should understand all risks as well as the bene ts
before electing to have a procedure performed that could compromise
your visual performance in the cockpit.
MEDICAL FACTS FOR PILOTS
Publication OK-06-148
Written by:
Van B. Nakagawara, O.D., F.A.A.O.
Kathryn J. Wood, CPOT
Ron W. Montgomery, B.S.
For additional copies, download from our Web site:
www.faa.gov/pilots/safety/pilotsafetybrochures/
Or contact:
FAA Civil Aerospace Medical Institute
Aerospace Medical Education Division
AAM-400, P.O. Box 25082
Oklahoma City, OK 73125
