
SERIES ‘‘ATS/ERS TASK FORCE: STANDARDISATION OF LUNG
FUNCTION TESTING’’
Edited by V. Brusasco, R. Crapo and G. Viegi
Number 2 in this Series
Standardisation of spirometry
M.R. Miller, J. Hankinson, V. Brusasco, F. Burgos, R. Casaburi, A. Coates,
R. Crapo, P. Enright, C.P.M. van der Grinten, P. Gustafsson, R. Jensen,
D.C. Johnson, N. MacIntyre, R. McKay, D. Navajas, O.F. Pedersen, R. Pellegrino,
G. Viegi and J. Wanger
CONTENTS
Background ............................................................... 320
FEV
1 and FVC manoeuvre .................................................... 321
Definitions . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 321
Equipment . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 321
Requirements . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 321
Display . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 321
Validation . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 322
Quality control . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 322
Quality control for volume-measuring devices . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 322
Quality control for flow-measuring devices . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 323
Test procedure . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 323
Within-manoeuvre evaluation . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 324
Start of test criteria. . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 324
End of test criteria . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 324
Additional criteria . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 324
Summary of acceptable blow criteria . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 325
Between-manoeuvre evaluation . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 325
Manoeuvre repeatability . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 325
Maximum number of manoeuvres . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 326
Test result selection . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 326
Other derived indices . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 326
FEV
t .................................................................. 326
Standardisation of FEV
1 for expired volume, FEV1/FVC and FEV1/VC.................... 326
FEF
25–75% .............................................................. 326
PEF.................................................................. 326
Maximal expiratory flow–volume loops . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 326
Definitions. . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 326
Equipment . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 327
Test procedure . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 327
Within- and between-manoeuvre evaluation . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 327
Flow–volume loop examples. . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 327
Reversibility testing . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 327
Method . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 327
Comment on dose and delivery method . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 328
Determination of reversibility . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 328
VC and IC manoeuvre ....................................................... 329
Definitions . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . 329
AFFILIATIONS
For affiliations, please see
Acknowledgements section
CORRESPONDENCE
V. Brusasco
Internal Medicine
University of Genoa
V.le Benedetto XV, 6
I-16132 Genova
Italy
Fax: 39 103537690
E-mail: [email protected]
Received:
March 23 2005
Accepted after revision:
April 05 2005
European Respiratory Journal
Print ISSN 0903-1936
Online ISSN 1399-3003
Previous articles in this series: No. 1: Miller MR, Crapo R, Hankinson J, et al. General considerations for lung function testing. Eur Respir J 2005; 26:
153–161.
EUROPEAN RESPIRATORY JOURNAL VOLUME 26 NUMBER 2 319
Eur Respir J 2005; 26: 319–338
DOI: 10.1183/09031936.05.00034805
CopyrightßERS Journals Ltd 2005
c

VCandIVC................................329
IC.......................................329
Equipment . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .329
Test procedure . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .329
VC......................................329
IC.......................................330
Use of a nose clip . . . . . . . . . . . . . . . . . . . . . . . . . . .330
Within-manoeuvre evaluation . . . . . . . . . . . . . . . . . . . . .330
Between-manoeuvre evaluation . . . . . . . . . . . . . . . . . . .330
Test result selection . . . . . . . . . . . . . . . . . . . . . . . . . . .330
Peak expiratory flow ...........................330
Definition . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .330
Equipment . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .330
Test procedure . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .330
Within-manoeuvre evaluation . . . . . . . . . . . . . . . . . . . . .331
Between-manoeuvre evaluation . . . . . . . . . . . . . . . . . . .331
Test result selection . . . . . . . . . . . . . . . . . . . . . . . . . . .331
Maximum voluntary ventilation ...................331
Definition . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .331
Equipment . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .331
Test procedure . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .331
Within-manoeuvre evaluation . . . . . . . . . . . . . . . . . . . . .331
Between-manoeuvre evaluation . . . . . . . . . . . . . . . . . . .331
Test result selection . . . . . . . . . . . . . . . . . . . . . . . . . . .331
Technical considerations ........................331
Minimal recommendations for spirometry systems . . . . . .331
BTPS correction . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .332
Comments . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .332
Test signals for spirometer testing . . . . . . . . . . . . . . . . .333
Method . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .333
Accuracy test . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .333
Repeatability test . . . . . . . . . . . . . . . . . . . . . . . . . . . .333
Test signals for PEF meter testing . . . . . . . . . . . . . . . . .333
Method . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .333
Accuracy test . . . . . . . . . . . . . . . . . . . . . . . . . . . . . .333
Repeatability test . . . . . . . . . . . . . . . . . . . . . . . . . . . .334
Test signals for MVV testing. . . . . . . . . . . . . . . . . . . . . .334
Abbreviations.................................334
Appendix ....................................335
KEYWORDS: Peak expiratory flow, spirometry, spirometry standardisation, spirometry technique, spirometry traning,
ventilation
BACKGROUND
Spirometry is a physiological test that measures how an
individual inhales or exhales volumes of air as a function of
time. The primary signal measured in spirometry may be
volume or flow.
Spirometry is invaluable as a screening test of general
respiratory health in the same way that blood pressure
provides important information about general cardiovascular
health. However, on its own, spirometry does not lead
clinicians directly to an aetiological diagnosis. Some indica-
tions for spirometry are given in table 1.
In this document, the most important aspects of spirometry are
the forced vital capacity (FVC), which is the volume delivered
during an expiration made as forcefully and completely as
possible starting from full inspiration, and the forced expira-
tory volume (FEV) in one second, which is the volume
delivered in the first second of an FVC manoeuvre. Other
spirometric variables derived from the FVC manoeuvre are
also addressed.
Spirometry can be undertaken with many different types of
equipment, and requires cooperation between the subject and
the examiner, and the results obtained will depend on
technical as well as personal factors (fig. 1). If the variability
of the results can be diminished and the measurement
accuracy can be improved, the range of normal values for
populations can be narrowed and abnormalities more easily
detected. The Snowbird workshop held in 1979 resulted in the
first American Thoracic Society (ATS) statement on the
standardisation of spirometry [1]. This was updated in 1987
and again in 1994 [2, 3]. A similar initiative was undertaken by
the European Community for Steel and Coal, resulting in the
first European standardisation document in 1983 [4]. This was
then updated in 1993 as the official statement of the European
Respiratory Society (ERS) [5]. There are generally only minor
differences between the two most recent ATS and ERS
statements, except that the ERS statement includes absolute
lung volumes and the ATS does not.
This document brings the views of the ATS and ERS together
in an attempt to publish standards that can be applied more
TABLE 1
Indications for spirometry
Diagnostic
To evaluate symptoms, signs or abnormal laboratory tests
To measure the effect of disease on pulmonary function
To screen individuals at risk of having pulmonary disease
To assess pre-operative risk
To assess prognosis
To assess health status before beginning strenuous physical activity
programmes
Monitoring
To assess therapeutic intervention
To describe the course of diseases that affect lung function
To monitor people exposed to injurious agents
To monitor for adverse reactions to drugs with known pulmonary toxicity
Disability/impairment evaluations
To assess patients as part of a rehabilitation programme
To assess risks as part of an insurance evaluation
To assess individuals for legal reasons
Public health
Epidemiological surveys
Derivation of reference equations
Clinical research
STANDARDISATION OF SPIROMETRY M.R. MILLER ET AL.
320
VOLUME 26 NUMBER 2 EUROPEAN RESPIRATORY JOURNAL
widely. The statement is structured to cover definitions,
equipment and patient-related procedures. All recording
devices covered by this statement must meet the relevant
requirements, regardless of whether they are for monitoring
or diagnostic purposes. There is no separate category for
‘‘monitoring’’ devices.
Although manufacturers have the responsibility for producing
pulmonary function testing systems that satisfy all the
recommendations presented here, it is possible that, for some
equipment, meeting all of them may not always be achievable.
In these circumstances, manufacturers should clearly identify
which equipment requirements have not been met. While
manufacturers are responsible for demonstrating the accuracy
and reliability of the systems that they sell, it is the user who is
responsible for ensuring that the equipment’s measurements
remain accurate. The user is also responsible for following
local law, which may have additional requirements. Finally,
these guidelines are minimum guidelines, which may not be
sufficient for all settings, such as when conducting research,
epidemiological studies, longitudinal evaluations and occupa-
tional surveillance.
FEV
1 AND FVC MANOEUVRE
Definitions
FVC is the maximal volume of air exhaled with maximally
forced effort from a maximal inspiration, i.e. vital capacity
performed with a maximally forced expiratory effort,
expressed in litres at body temperature and ambient pressure
saturated with water vapour (BTPS; see BTPS correction
section).
FEV
1 is the maximal volume of air exhaled in the first second
of a forced expiration from a position of full inspiration,
expressed in litres at BTPS.
Equipment
Requirements
The spirometer must be capable of accumulating volume for
o15 s (longer times are recommended) and measuring
volumes of o8 L (BTPS) with an accuracy of at least ¡3% of
reading or ¡0.050 L, whichever is greater, with flows between
0 and 14 L?s
-1
. The total resistance to airflow at 14.0 L?s
-1
must
be ,1.5 cmH
2
O?L
-1
?s
-1
(0.15 kPa?L
-1
?s
-1
; see Minimal recommen-
dations for spirometry systems section). The total resistance must
be measured with any tubing, valves, pre-filter, etc. included
that may be inserted between the subject and the spirometer.
Some devices may exhibit changes in resistance due to water
vapour condensation, and accuracy requirements must be met
under BTPS conditions for up to eight successive FVC
manoeuvres performed in a 10-min period without inspiration
from the instrument.
Display
For optimal quality control, both flow–volume and volume–
time displays are useful, and test operators should visually
inspect the performance of each manoeuvre for quality
assurance before proceeding with another manoeuvre. This
inspection requires tracings to meet the minimum size and
resolution requirements set forth in this standard.
Displays of flow versus volume provide more detail for the
initial portion (first 1 s) of the FVC manoeuvre. Since this
portion of the manoeuvre, particularly the peak expiratory
flow (PEF), is correlated with the pleural pressure during the
manoeuvre, the flow–volume display is useful to assess the
magnitude of effort during the initial portions of the
manoeuvre. The ability to overlay a series of flow–volume
curves registered at the point of maximal inhalation may
be helpful in evaluating repeatability and detecting sub-
maximal efforts. However, if the point of maximal inhala-
tion varies between blows, then the interpretation of these
results is difficult because the flows at identical measured
volumes are being achieved at different absolute lung
volumes. In contrast, display of the FVC manoeuvre as a
volume–time graph provides more detail for the latter part
of the manoeuvre. A volume–time tracing of sufficient
size also allows independent measurement and calculation
of parameters from the FVC manoeuvres. In a display of
multiple trials, the sequencing of the blows should be
apparent to the user.
For the start of test display, the volume–time display should
include o0.25 s, and preferably 1 s, before exhalation starts
(zero volume). This time period before there is any change in
volume is needed to calculate the back extrapolated volume
(EV; see Start of test criteria section) and to evaluate effort
during the initial portion of the manoeuvre. Time zero, as
defined by EV, must be presented as the zero point on the
graphical output.
The last 2 s of the manoeuvre should be displayed to indicate a
satisfactory end of test (see End of test criteria section).
When a volume–time curve is plotted as hardcopy, the volume
scale must be o10 mm?L
-1
(BTPS). For a screen display,
5mm?L
-1
is satisfactory (table 2).
The time scale should be o20 mm?s
-1
, and larger time
scales are preferred (o30 mm?s
-1
) when manual measure-
ments are made [1, 6, 7]. When the volume–time plot is used in
conjunction with a flow–volume curve (i.e. both display
methods are provided for interpretations and no hand
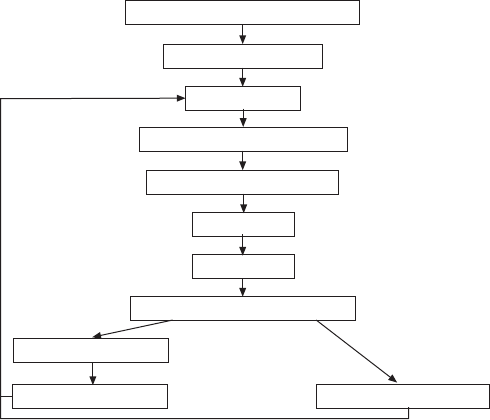
Equipment performance criteria
Equipment validation
Quality control
Subject/patient manoeuvres
Measurement procedures
Acceptability
Repeatability
Reference value/interpretation
Clinical assessment
Quality assessment
Feedback to technician
FIGURE 1. Spirometry standardisation steps.
M.R. MILLER ET AL. STANDARDISATION OF SPIROMETRY
c
EUROPEAN RESPIRATORY JOURNAL VOLUME 26 NUMBER 2 321
measurements are performed), the time scale requirement
is reduced to 10 mm?s
-1
from the usually required minimum
of 20 mm?s
-1
(table 2). The rationale for this exception is
that the flow–volume curve can provide the means for
quality assessment during the initial portion of the FVC
manoeuvre. The volume–time curve can be used to evaluate
the latter part of the FVC manoeuvre, making the time scale
less critical.
Validation
It is strongly recommended that spirometry systems should be
evaluated using a computer-driven mechanical syringe or its
equivalent, in order to test the range of exhalations that are
likely to be encountered in the test population. Testing the
performance of equipment is not part of the usual laboratory
procedures (see Test signals for spirometer testing section).
Quality control
Attention to equipment quality control and calibration is
an important part of good laboratory practice. At a minimum,
the requirements are as follows: 1) a log of calibration results
is maintained; 2) the documentation of repairs or other
alterations which return the equipment to acceptable opera-
tion; 3) the dates of computer software and hardware
updates or changes; and 4) if equipment is changed or
relocated (e.g. industrial surveys), calibration checks and
quality-control procedures must be repeated before further
testing begins.
Key aspects of equipment quality control are summarised in
table 3.
Calibration is the procedure for establishing the relationship
between sensor-determined values of flow or volume and the
actual flow or volume.
A calibration check is different from calibration and is the
procedure used to validate that the device is within calibration
limits, e.g. ¡3% of true. If a device fails its calibration check,
then a new calibration procedure or equipment maintenance is
required. Calibration checks must be undertaken daily, or
more frequently, if specified by the manufacturer.
The syringe used to check the volume calibration of spiro-
meters must have an accuracy of ¡15 mL or ¡0.5% of the full
scale (15 mL for a 3-L syringe), and the manufacturer must
provide recommendations concerning appropriate intervals
between syringe calibration checks. Users should be aware
that a syringe with an adjustable or variable stop may be out
of calibration if the stop is reset or accidentally moved.
Calibration syringes should be periodically (e.g. monthly) leak
tested at more than one volume up to their maximum; this can
be done by attempting to empty them with the outlet corked. A
dropped or damaged syringe should be considered out of
calibration until it is checked.
With regard to time, assessing mechanical recorder time scale
accuracy with a stopwatch must be performed at least
quarterly. An accuracy of within 2% must be achieved.
Quality control for volume-measuring devices
The volume accuracy of the spirometer must be checked at least
daily, with a single discharge of a 3-L calibrated syringe. Daily
calibration checking is highly recommended so that the onset of
a problem can be determined within 1 day, and also to help
define day-to-day laboratory variability. More frequent checks
may be required in special circumstances, such as: 1) during
industrial surveys or other studies in which a large number of
subject manoeuvres are carried out, the equipment’s calibration
should be checked more frequently than daily [8]; and 2) when
the ambient temperature is changing (e.g. field studies), volume
accuracy must be checked more frequently than daily and the
BTPS correction factor appropriately updated.
The accuracy of the syringe volume must be considered in
determining whether the measured volume is within accep-
table limits. For example, if the syringe has an accuracy of
0.5%, a reading of ¡3.5% is appropriate.
The calibration syringe should be stored and used in such a
way as to maintain the same temperature and humidity of the
testing site. This is best accomplished by keeping the syringe in
close proximity to the spirometer, but out of direct sunlight
and away from heat sources.
Volume-type spirometer systems must be evaluated for leaks
every day [9, 10]. The importance of undertaking this daily test
cannot be overstressed. Leaks can be detected by applying a
constant positive pressure of o3.0 cmH
2
O (0.3 kPa) with the
spirometer outlet occluded (preferably at or including the
mouthpiece). Any observed volume loss .30 mL after 1 min
indicates a leak [9, 10] and needs to be corrected.
TABLE 2
Recommended minimum scale factors for time,
volume and flow on graphical output
Instrument display Hardcopy graphical outputParameter
Resolution
required
Scale
factor
Resolution
required
Scale
factor
Volume
#
0.050 L 5 mm? L
-1
0.025 L 10 mm?L
-1
Flow
#
0.200 L?s
-1
2.5 mm?L
-1
?s
-1
0.100 L?s
-1
5mm?L
-1
?s
-1
Time 0.2 s 10 mm?s
-1
0.2 s 20 mm?s
-1
#
: the correct aspect ratio for a flow versus volume display is two units of flow
per one unit of volume.
TABLE 3
Summary of equipment quality control
Test Minimum interval Action
Volume Daily Calibration check with a 3-L syringe
Leak Daily 3 cmH
2
O (0.3 kPa) constant pressure
for 1 min
Volume linearity Quarterly 1-L increments with a calibrating syringe
measured over entire volume range
Flow linearity Weekly Test at least three different flow ranges
Time Quarterly Mechanical recorder check with stopwatch
Software New versions Log installation date and perform test using
‘‘known’’ subject
STANDARDISATION OF SPIROMETRY M.R. MILLER ET AL.
322
VOLUME 26 NUMBER 2 EUROPEAN RESPIRATORY JOURNAL

At least quarterly, volume spirometers must have their
calibration checked over their entire volume range using a
calibrated syringe [11] or an equivalent volume standard. The
measured volume should be within ¡3.5% of the reading or
65 mL, whichever is greater. This limit includes the 0.5%
accuracy limit for a 3-L syringe. The linearity check procedure
provided by the manufacturer can be used if it is equivalent to
one of the following procedures: 1) consecutive injections of
1-L volume increments while comparing observed volume
with the corresponding cumulative measured volume, e.g. 0–1,
1–2, 2–3,…6–7 and 7–8 L, for an 8-L spirometer; and 2)
injection of a 3-L volume starting at a minimal spirometer
volume, then repeating this with a 1-L increment in the start
position, e.g. 0–3, 1–4, 2–5, 3–6, 4–7 and 5–8 L, for an 8-L
spirometer.
The linearity check is considered acceptable if the spirometer
meets the volume accuracy requirements for all volumes
tested.
Quality control for flow-measuring devices
With regards to volume accuracy, calibration checks must be
undertaken at least daily, using a 3-L syringe discharged at
least three times to give a range of flows varying between 0.5
and 12 L?s
-1
(with 3-L injection times of ,6 s and ,0.5 s). The
volume at each flow should meet the accuracy requirement of
¡3.5%. For devices using disposable flow sensors, a new
sensor from the supply used for patient tests should be tested
each day.
For linearity, a volume calibration check should be per-
formed weekly with a 3-L syringe to deliver three relatively
constant flows at a low flow, then three at a mid-range flow
and finally three at a high flow. The volumes achieved at each
of these flows should each meet the accuracy requirement of
¡3.5%.
Test procedure
There are three distinct phases to the FVC manoeuvre, as
follows: 1) maximal inspiration; 2) a ‘‘blast’’ of exhalation; and
3) continued complete exhalation to the end of test (EOT).
The technician should demonstrate the appropriate technique
and follow the procedure described in table 4. The subject
should inhale rapidly and completely from functional residual
capacity (FRC), the breathing tube should be inserted into the
subject’s mouth (if this has not already been done), making
sure the lips are sealed around the mouthpiece and that the
tongue does not occlude it, and then the FVC manoeuvre
should be begun with minimal hesitation. Reductions in PEF
and FEV
1 have been shown when inspiration is slow and/or
there is a 4–6 s pause at total lung capacity (TLC) before
beginning exhalation [12]. It is, therefore, important that the
preceding inspiration is fast and any pause at full inspiration
be minimal (i.e. only for 1–2 s). The test assumes a full
inhalation before beginning the forced exhalation, and it is
imperative that the subject takes a complete inhalation before
beginning the manoeuvre. The subject should be prompted to
‘‘blast,’’ not just ‘‘blow,’’ the air from their lungs, and then he/
she should be encouraged to fully exhale. Throughout the
manoeuvre, enthusiastic coaching of the subject using appro-
priate body language and phrases, such as ‘‘keep going’’, is
required. It is particularly helpful to observe the subject with
occasional glances to check for distress, and to observe the
tracing or computer display during the test to help ensure
maximal effort. If the patient feels ‘‘dizzy’’, the manoeuvre
should be stopped, since syncope could follow due to
prolonged interruption of venous return to the thorax. This is
more likely to occur in older subjects and those with airflow
limitation. Performing a vital capacity (VC) manoeuvre (see VC
and IC manoeuvre section), instead of obtaining FVC, may help
to avoid syncope in some subjects. Reducing the effort part-
way through the manoeuvre [13] may give a higher expiratory
volume in some subjects, but then is no longer a maximally
forced expiration. Well-fitting false teeth should not be
routinely removed, since they preserve oropharyngeal geome-
try and spirometry results are generally better with them in
place [14].
With appropriate coaching, children as young as 5 yrs of
age are often able to perform acceptable spirometry [15].
The technicians who are involved in the pulmonary function
testing of children should be specifically trained to deal
with such a situation. A bright, pleasant atmosphere,
TABLE 4
Procedures for recording forced vital capacity
Check the spirometer calibration
Explain the test
Prepare the subject
Ask about smoking, recent illness, medication use, etc.
Measure weight and height without shoes
Wash hands
Instruct and demonstrate the test to the subject, to include
Correct posture with head slightly elevated
Inhale rapidly and completely
Position of the mouthpiece (open circuit)
Exhale with maximal force
Perform manoeuvre (closed circuit method)
Have subject assume the correct posture
Attach nose clip, place mouthpiece in mouth and close lips around the
mouthpiece
Inhale completely and rapidly with a pause of ,1 s at TLC
Exhale maximally until no more air can be expelled while maintaining an upright
posture
Repeat instructions as necessary, coaching vigorously
Repeat for a minimum of three manoeuvres; no more than eight are usually
required
Check test repeatability and perform more manoeuvres as necessary
Perform manoeuvre (open circuit method)
Have subject assume the correct posture
Attach nose clip
Inhale completely and rapidly with a pause of ,1 s at TLC
Place mouthpiece in mouth and close lips around the mouthpiece
Exhale maximally until no more air can be expelled while maintaining an upright
posture
Repeat instructions as necessary, coaching vigorously
Repeat for a minimum of three manoeuvres; no more than eight are usually
required
Check test repeatability and perform more manoeuvres as necessary
TLC: total lung capacity.
M.R. MILLER ET AL. STANDARDISATION OF SPIROMETRY
c
EUROPEAN RESPIRATORY JOURNAL VOLUME 26 NUMBER 2 323
including age-appropriate toys, reading material and art, is
important in making children feel at ease. Encouragement,
detailed but simple instructions, lack of intimidation and
visual feedback in the teaching are important in helping
children to perform the manoeuvre. Even if unsuccessful at
the first session, children will learn to be less intimidated
and may perform far better in a subsequent session. Testing
children in ‘‘adult’’ laboratories, where no effort is made to
cater for the specific needs of the younger subjects, is to be
discouraged.
The use of a nose clip or manual occlusion of the nares is
recommended, and, for safety reasons, testing should be
preferably done in the sitting position, using a chair with
arms and without wheels. If testing is undertaken with the
patient standing or in another position, this must be
documented on the report.
Within-manoeuvre evaluation
Start of test criteria
The start of test, for the purpose of timing, is determined by the
back extrapolation method (fig. 2) [1, 3, 9, 16]. The new ‘‘time
zero’’ from back extrapolation defines the start for all timed
measurements. For manual measurements, the back extrapola-
tion method traces back from the steepest slope on the
volume–time curve [17]. For computerised back extrapolation,
it is recommended that the largest slope averaged over an 80-
ms period is used [18]. Figure 2 provides an example and
explanation of back extrapolation and the derivation of EV. To
achieve an accurate time zero and assure the FEV
1 comes from
a maximal effort curve, the EV must be , 5% of the FVC or
0.150 L, whichever is greater. If a manoeuvre has an obviously
hesitant start, the technician may terminate the trial early to
avoid an unnecessary prolonged effort.
Rapid computerised feedback to the technician when the start
criteria are not met is strongly encouraged. In addition to the
expiratory manoeuvre, the volume-time curve display (graph)
should ideally include the whole preceding inspiratory
manoeuvre, but must include o0.25 s and preferably o1s
prior to the start of exhalation (time zero). The equipment
should display the EV value. Inspection of the flow–volume
curve may be added as a measure of the satisfactory start of
test. PEF should be achieved with a sharp rise and occur close
to the point of maximal inflation, i.e. the start of exhalation (see
Equipment section).
End of test criteria
It is important for subjects to be verbally encouraged to
continue to exhale the air at the end of the manoeuvre to obtain
optimal effort, e.g. by saying ‘‘keep going’’. EOT criteria are
used to identify a reasonable FVC effort, and there are two
recommended EOT criteria, as follows. 1) The subject cannot or
should not continue further exhalation. Although subjects
should be encouraged to achieve their maximal effort, they
should be allowed to terminate the manoeuvre on their own at
any time, especially if they are experiencing discomfort. The
technician should also be alert to any indication that the patient
is experiencing discomfort, and should terminate the test if a
patient is becoming uncomfortable or is approaching syncope.
2) The volume–time curve shows no change in volume
(,0.025 L) for o1 s, and the subject has tried to exhale for
o3 s in children aged ,10 yrs and for o6 s in subjects aged
.10 yrs.
The equipment should signal to the technician if the plateau
criteria were not met. A satisfactory EOT may still have been
achieved, but an equipment alert will help the technician to
pinpoint where the subject may need more encouragement.
It is of note that a closure of the glottis may prematurely
terminate a manoeuvre at ,6 s, even when the apparent
duration of the blow exceeds 6 s.
For patients with airways obstruction or older subjects,
exhalation times of .6 s are frequently needed. However,
exhalation times of .15 s will rarely change clinical decisions.
Multiple prolonged exhalations are seldom justified and may
cause light headedness, syncope, undue fatigue and unneces-
sary discomfort.
Achieving EOT criteria is one measure of manoeuvre accept-
ability. Manoeuvres that do not meet EOT criteria should not
be used to satisfy the requirement of three acceptable
manoeuvres. However, early termination, by itself, is not a
reason to eliminate all the results from such a manoeuvre from
further consideration. Information such as the FEV
1 may be
useful (depending on the length of exhalation) and can be
reported from these early terminated manoeuvres.
Some young children may have difficulty meeting the ATS
EOT criteria [3], although they may meet other repeatability
criteria [19]. Curve-fitting techniques [20] may prove useful in
developing new EOT criteria specific for young children.
Additional criteria
A cough during the first second of the manoeuvre can affect
the measured FEV
1 value. Coughing in the first second or any
other cough that, in the technician’s judgment, interferes with
the measurement of accurate results [3] will render a test
unacceptable.
0.8
EV
0.0
1.0
0.6
0.4
0.2
Volume L
0.500.250.00
New time zero
Time s
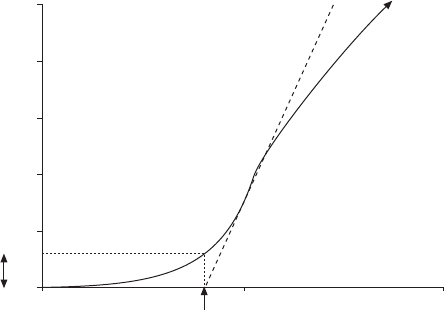
FIGURE 2. Expanded version of the early part of a subject’s volume–time
spirogram, illustrating back extrapolation through the steepest part of the curve,
where flow is peak expiratory flow (PEF), to determine the new ‘‘time zero’’. Forced
vital capacity (FVC)54.291 L; back extrapolated volume (EV)50.123 L (2.9% FVC).
-----: back extrapolation line through PEF.
STANDARDISATION OF SPIROMETRY M.R. MILLER ET AL.
324
VOLUME 26 NUMBER 2 EUROPEAN RESPIRATORY JOURNAL

A Valsalva manoeuvre (glottis closure) or hesitation during the
manoeuvre that causes a cessation of airflow in a manner that
precludes an accurate estimate of either FEV
1 or FVC [3] will
render a test unacceptable.
There must be no leak at the mouth [3]. Patients with
neuromuscular disease may require manual or other assistance
from the technician to guarantee an adequate seal.
Obstruction of the mouthpiece, e.g. by the tongue being placed
in front of the mouthpiece or by teeth in front of the
mouthpiece, or by distortion from biting, may affect the
performance of either the device or the subject.
Summary of acceptable blow criteria
The acceptability criteria are a satisfactory start of test and a
satisfactory EOT, i.e. a plateau in the volume–time curve. In
addition, the technician should observe that the subject
understood the instructions and performed the manoeuvre
with a maximum inspiration, a good start, a smooth
continuous exhalation and maximal effort. The following
conditions must also be met: 1) without an unsatisfactory start
of expiration, characterised by excessive hesitation or false
start extrapolated volume or EV .5% of FVC or 0.150 L,
whichever is greater (fig. 2); 2) without coughing during the
first second of the manoeuvre, thereby affecting the measured
FEV
1 value, or any other cough that, in the technician’s
judgment, interferes with the measurement of accurate results
[3]; 3) without early termination of expiration (see End of test
criteria section); 4) without a Valsalva manoeuvre (glottis
closure) or hesitation during the manoeuvre that causes a
cessation of airflow, which precludes accurate measurement of
FEV
1 or FVC [3]; 5) without a leak [3]; 6) without an obstructed
mouthpiece (e.g. obstruction due to the tongue being placed in
front of the mouthpiece, or teeth in front of the mouthpiece, or
mouthpiece deformation due to biting); and 7) without
evidence of an extra breath being taken during the manoeuvre.
It should be noted that a usable curve must only meet
conditions 1 and 2 above, while an acceptable curve must meet
all of the above seven conditions.
It is desirable to use a computer-based system that provides
feedback to the technician when the above conditions are not
met. The reporting format should include qualifiers indicating
the acceptability of each manoeuvre. However, failure to meet
these goals should not necessarily prevent reporting of results,
since, for some subjects, this is their best performance. Records
of such manoeuvres should be retained since they may contain
useful information.
Between-manoeuvre evaluation
Using the previously described criteria, an adequate test
requires a minimum of three acceptable FVC manoeuvres.
Acceptable repeatability is achieved when the difference
between the largest and the next largest FVC is f0.150 L
and the difference between the largest and next largest FEV
1 is
f0.150 L [21]. For those with an FVC of f1.0 L, both these
values are 0.100 L. If these criteria are not met in three
manoeuvres, additional trials should be attempted, up to, but
usually no more than, eight manoeuvres. Large variability
among tests is often due to incomplete inhalations. Some
patients may require a brief rest period between manoeuvres.
Volume–time or flow–volume curves from at least the best
three FVC manoeuvres must be retained. Table 5 gives a
summary of the within- and between-manoeuvre evaluation.
Manoeuvre repeatability
For FVC measurements, acceptability must be determined by
ascertaining that the recommendations outlined previously on
performing the FVC test are met. The guidelines of the ATS [3]
contain examples of unacceptable volume–time and corre-
sponding flow–volume curves. Figure 3 shows a flow chart
outlining how the criteria for blow acceptability are applied
before those for repeatability.
The repeatability criteria are used to determine when more
than three acceptable FVC manoeuvres are needed; these
criteria are not to be used to exclude results from reports or to
exclude subjects from a study. Labelling results as being
derived from data that do not conform to the repeatability
criteria described previously is recommended. In addition, the
repeatability criteria are minimum requirements. Many sub-
jects are able to achieve FVC and FEV
1 repeatability to within
0.150 L. Manoeuvres with an unacceptable start of test or a
cough (unusable curve) must be discarded before applying the
repeatability criteria and cannot be used in determining the
best values. Manoeuvres with early termination or a Valsalva
manoeuvre may be used for selecting the largest FVC and
FEV
1.
TABLE 5
Summary of within- and between-manoeuvre
acceptability criteria
Within-manoeuvre criteria
Individual spirograms are ‘‘acceptable’’ if
They are free from artefacts [3]
Cough during the first second of exhalation
Glottis closure that influences the measurement
Early termination or cut-off
Effort that is not maximal throughout
Leak
Obstructed mouthpiece
They have good starts
Extrapolated volume ,5% of FVC or 0.15 L, whichever is greater
They show satisfactory exhalation
Duration of o6 s (3 s for children) or a plateau in the volume–time curve or
If the subject cannot or should not continue to exhale
Between-manoeuvre criteria
After three acceptable spirograms have been obtained, apply the following
tests
The two largest values of FVC must be within 0.150 L of each other
The two largest values of FEV
1 must be within 0.150 L of each other
If both of these criteria are met, the test session may be concluded
If both of these criteria are not met, continue testing until
Both of the criteria are met with analysis of additional acceptable spirograms
or
A total of eight tests have been performed (optional) or
The patient/subject cannot or should not continue
Save, as a minimum, the three satisfactory manoeuvres
FVC: forced vital capacity; FEV
1: forced expiratory volume in one second.
M.R. MILLER ET AL. STANDARDISATION OF SPIROMETRY
c
EUROPEAN RESPIRATORY JOURNAL VOLUME 26 NUMBER 2 325
No spirogram or test result should be rejected solely on the
basis of its poor repeatability. The repeatability of results
should be considered at the time of interpretation. The use of
data from manoeuvres with poor repeatability or failure to
meet the EOT requirements is left to the discretion of the
interpreter.
Maximum number of manoeuvres
Although there may be some circumstances in which more
than eight consecutive FVC manoeuvres may be needed, eight
is generally a practical upper limit for most subjects [22, 23].
After several forced expiratory manoeuvres, fatigue can begin
to take its toll on subjects and additional manoeuvres would be
of little added value. In extremely rare circumstances, subjects
may show a progressive reduction in FEV
1 or FVC with each
subsequent blow. If the cumulative drop exceeds 20% of start
value, the test procedure should be terminated in the interest
of patient safety. The sequence of the manoeuvres should be
recorded.
Test result selection
FVC and FEV
1 should be measured from a series of at least
three forced expiratory curves that have an acceptable start of
test and are free from artefact, such as a cough (i.e. ‘‘usable
curves’’). The largest FVC and the largest FEV
1 (BTPS) should
be recorded after examining the data from all of the usable
curves, even if they do not come from the same curve.
Other derived indices
FEV
t
FEVt is the maximal volume exhaled by time t seconds (timed
from the time zero defined by back extrapolation) of a forced
expiration from a position of full inspiration, expressed in litres
at BTPS. Very young children may not be able to produce
prolonged expirations, but there is increasing evidence that
indices derived from blows with forced expiratory times of
,1 s may have clinical usefulness [19]. At present, there are
insufficient data to recommend the use of FEV
0.5 or FEV0.75.
When the subject does not exhale completely, the volume
accumulated over a shorter period of time (e.g. 6 s) may be
used as an approximate surrogate for FVC. When such
surrogates are used, the volume label should reflect the shorter
exhalation time (e.g. FEV
6 for a 6-s exhalation). FEV6 has been
increasingly considered a reasonably reliable surrogate for
FVC [24] and can be used for normalising FEV
1 (e.g. FEV1/
FEV
6). Recording FEV6 seems to have the advantage of being
more reproducible than FVC, being less physically demanding
for patients and providing a more explicit EOT. Confirmation
from other studies is required.
Standardisation of FEV
1 for expired volume, FEV1/FVC and FEV1/
VC
In some patients, a slow or unforced VC or inspiratory vital
capacity (IVC) manoeuvre (see VC and IC manoeuvre section)
may provide a larger and more appropriate denominator for
calculation of the FEV
1/VC%. Some investigators have
reported that the VC is slightly higher than the FVC in normal
subjects [25].
FEF
25–75%
The mean forced expiratory flow between 25% and 75% of
the FVC (FEF
25–75%) has also been known as the maximum
mid-expiratory flow. This index is taken from the blow
with the largest sum of FEV
1 and FVC. The FEF25–75% must
be measured with an accuracy of at least ¡5% of reading or
¡0.200 L?s
-1
whichever is greater, over a range of up to 7 L?s
-1
.
It should be noted that it is highly dependent on the validity of
the FVC measurement and the level of expiratory effort.
PEF
PEF is usually obtained from flow–volume curve data. It is the
maximum expiratory flow achieved from a maximum forced
expiration, starting without hesitation from the point of
maximal lung inflation, expressed in L?s
-1
. When PEF is
recorded using a patient-administered portable PEF meter, it is
often expressed in L?min
-1
. PEF is covered in more detail later.
Maximal expiratory flow–volume loops
The shape of a maximum flow–volume loop (MFVL), which
includes forced inspiratory manoeuvres, can be helpful in
quality control and in detecting the presence of upper airway
obstruction. None of the numerical indices from a MFVL has
clinical utility superior to FEV
1, FVC, FEF25–75% and PEF, and
are not considered in detail here.
Definitions
With regard to instantaneous flows, the recommended
measure is the instantaneous forced expiratory flow when
X% of the FVC has been expired (FEF
X%). The maximal
instantaneous forced expiratory flow when X% of the FVC
remains to be expired (MEF
X%) was the term previously
recommended in Europe.
Instantaneous forced inspiratory flow when X% of the FVC has
been expired (FIF
X%) and mid-inspiratory flow when X% of the
FVC has been expired refer to the flows measured on
the inspiratory limb of a flow–volume loop. FIF
25–75%, also
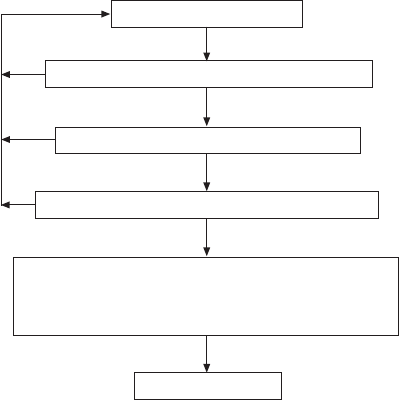
Perform FVC manoeuvre
Met within-manoeuvre acceptability criteria?
Achieved three acceptable manoeuvres?
Met between manoeuvre repeatability criteria?
Determine largest FVC and largest FEV
1
Select manoeuvre with largest sum of FVC+FEV1 to
determine other indices
Store and interpret
Yes
Yes
Yes
No
No
No
FIGURE 3. Flow chart outlining how acceptability and reapeatability criteria are
to be applied. FVC: forced vital capacity; FEV
1: forced expiratory volume in one
second.
STANDARDISATION OF SPIROMETRY M.R. MILLER ET AL.
326
VOLUME 26 NUMBER 2 EUROPEAN RESPIRATORY JOURNAL
referred to as maximal mid-inspiratory flow, is analogous to
FEF
25–75% (see Other derived indices section).
Equipment
Instantaneous flows must be measured with an accuracy of
¡5% of reading or ¡0.200 L?s
-1
, whichever is greater, over a
range of -14–14 L?s
-1
. The level of minimum detectable flow
should be 0.025 L?s
-1
. When a maximum flow–volume loop is
plotted or displayed, exhaled flow must be plotted upwards,
and exhaled volume towards the right. A 2:1 ratio must be
maintained between the flow and volume scales, e.g. 2L?s
-1
of
flow and 1 L of exhaled volume must be the same distance on
their respective axes. The flow and volume scales, used in
reviewing test performance, must be equivalent to that shown
in table 2.
Test procedure
The subject has to make a full expiratory and inspiratory loop
as a single manoeuvre. In many laboratories, this is the
primary manoeuvre for spirometry. The subject is asked to
take a rapid full inspiration to TLC from room air through the
mouth, then insert the mouthpiece and, without hesitation,
perform an expiration with maximum force until no more gas
can be expelled, followed by a quick maximum inspiration. At
this point, the manoeuvre is finished.
An alternative procedure is for the subject to insert the
mouthpiece while undertaking tidal breathing at FRC, and
then, in one continuous sequence, do the following: make a
slow expiration to residual volume (RV); followed directly by a
slow inspiration to TLC; follow this by a rapid full expiration
with maximal effort to RV; and followed by a rapid full
inspiration with maximal effort back to TLC.
This procedure is slightly more complicated and may not be
suitable for all equipment, but it obtains a measurement of VC
as well as FVC.
Within- and between-manoeuvre evaluation
These evaluations are the same as for FVC (see Within-
manoeuvre evaluation and Between-manoeuvre evaluation sec-
tions). Occasionally, a subject is unable to perform a
satisfactory inspiratory limb immediately following a maximal
forced expiratory manoeuvre. This is particularly common in
the elderly and the infirm. In these circumstances, it may be
necessary for the subject to record an inspiratory manoeuvre
separately from the expiratory manoeuvre. Equipment should
be able to perform these separately and then present three or
more loops together on a graphical display or output.
Flow–volume loop examples
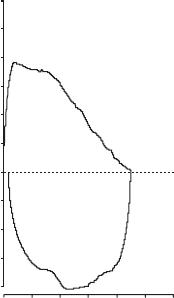
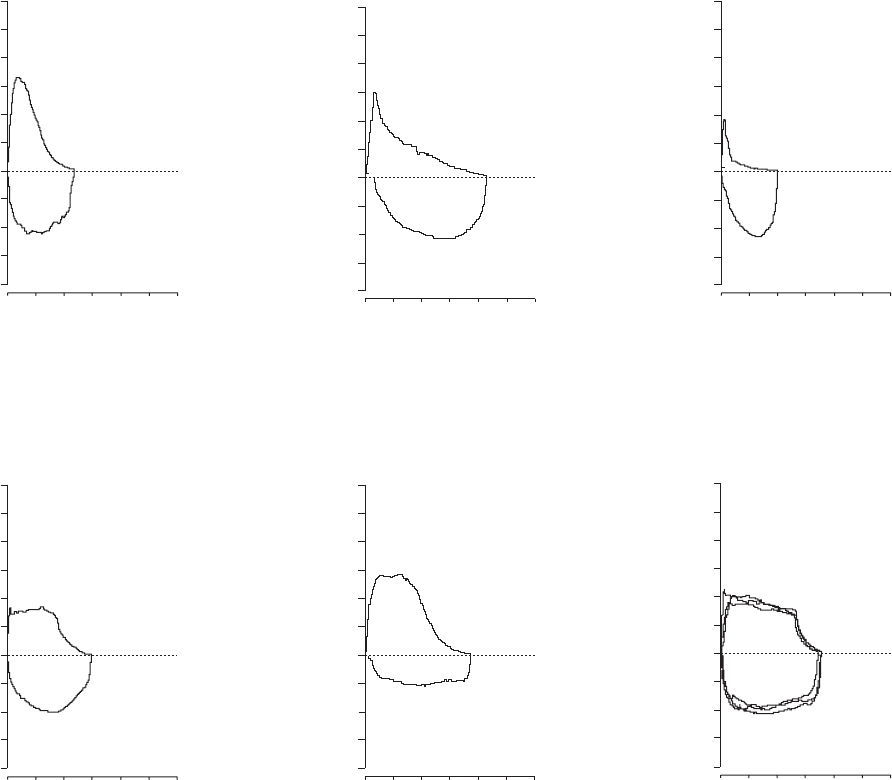
The following figures (figures 4–10) give typical examples of
commonly encountered flow–volume loop configurations. The
advantages of visual pattern recognition from the MFVL can
readily be appreciated. The shapes of the manoeuvres must be
repeatable (fig. 10) for any interpretation to be made. This is
especially true for the plateau effect on expiratory and
inspiratory limbs of the manoeuvre found in upper airway
obstruction, as this can be mimicked by poor effort, which is
usually variable from blow to blow. A further explanation is
given in the ATS/ERS statement on lung function interpreta-
tion [26].
Reversibility testing
A determination of airflow-limitation reversibility with drug
administration is commonly undertaken as part of lung
function testing. The choice of drug, dose and mode of
delivery is a clinical decision depending on what the clinician
wishes to learn from the test.
If the aim of the test is to determine whether the patient’s lung
function can be improved with therapy in addition to their
regular treatment, then the subject can continue with his/her
regular medication prior to the test.
If the clinician wants to determine whether there is any
evidence of reversible airflow limitation, then the subject
should undergo baseline function testing when not taking any
drugs prior to the test. Short-acting inhaled drugs (e.g. the b-
agonist albuterol/salbutamol or the anticholinergic agent
ipratropium bromide) should not be used within 4 h of testing.
Long-acting b-agonist bronchodilators (e.g. salmeterol or
formoterol) and oral therapy with aminophylline or slow-
release b-agonists should be stopped for 12 h prior to the test.
Smoking should be avoided for o1 h prior to testing and
throughout the duration of the test procedure.
Method
The following steps are undertaken. 1) The subject has three
acceptable tests of FEV
1, FVC and PEF recorded as described
previously. 2) The drug is administered in the dose and by the
method indicated for the test. For example, after a gentle and
incomplete expiration, a dose of 100 mg of albuterol/salbuta-
mol is inhaled in one breath to TLC from a valved spacer
device. The breath is then held for 5–10 s before the subject
exhales. Four separate doses (total dose 400 mg) are delivered at
,30-s intervals. This dose ensures that the response is high on
the albuterol dose–response curve. A lower dose can be used if
there is concern about any effect on the patient’s heart rate or
tremor. Other drugs can also be used. For the anticholinergic
agent ipratropium bromide, the total dose is 160 mg(4640 mg).
Three additional acceptable tests are recorded o10 min and
up to 15 min later for short-acting b
2
-agonists, and 30 min later
for short-acting anticholinergic agents.
12
10
8
6
4
2
0
-2
-4
-6
-8
Flow L·s
-1
0
123456
Volume L
FIGURE 4. Flow–volume loop of a normal subject.
M.R. MILLER ET AL. STANDARDISATION OF SPIROMETRY
c
EUROPEAN RESPIRATORY JOURNAL VOLUME 26 NUMBER 2 327
Comment on dose and delivery method
Standardising the bronchodilator dose administered is
necessary in order to standardise the definition of a
significant bronchodilator response. The rate of pulmonary
deposition of a drug with tidal breathing from an unvented
nebuliser will depend on drug concentration, rate of
nebuliser output, particle-size distribution, and the ratio
of the time spent in inspiration over the total respiratory
time (t
i/ttot) [27]. The fraction of the aerosol carried in
particles with a diameter of f5 mm that is expected to
deposit in adult lungs if inhaled through a mouthpiece [28]
is defined as the respirable fraction (RF). For example,
2.5 mg of salbutamol (albuterol) in 2.5 mL of solution,
placed in a Hudson Updraft II (Hudson RCI, Temecula,
CA, USA) driven by a PulmoAide compressor (De Vilbiss,
Somerset, PA, USA), would produce ,0.1 mg?min
-1
in the
RF. For a respiratory rate of 15 breaths?min
-1
and a ti/ttot
of 0.45, this would give ,3 mg deposited in the lungs per
breath, or 45 mg?min
-1
. For adults using a metered dose
inhaler (MDI) with a valve-holding chamber (spacer),
between 10 and 20% [29, 30] of a 100-mg ‘‘puff’’ (or ,15
mg per activation) would be expected to be deposited in
the lung of an adult. Without a spacer, the deposition will
be less, and heavily technique dependent [31]. Pulmonary
deposition from dry-powder inhalers is device specific, and
breath-enhanced nebulisers deposit much more than
unvented ones [32, 33]. CFC-free MDIs produce a smaller
particle-size distribution and improved (up to 50% of dose)
lung deposition compared with those with CFC propellant
[34]. For children, pulmonary deposition is less than that in
adults [35], possibly relating to the size of the upper
airway. Each laboratory should be familiar with the
pulmonary-deposition characteristics of the devices they
use.
Determination of reversibility
This aspect is covered in detail in the interpretative strategy
document of the ATS and ERS [26].
12
10
8
6
4
2
0
-2
-4
-6
-8
Flow L·s
-1
0
123 456
Volume L
FIGURE 5. Flow–volume loop of a normal sub-
ject with end expiratory curvilinearity, which can be
seen with ageing.
12
10
8
6
4
2
0
-2
-4
-6
-8
Flow L·s
-1
0
123456
Volume L
FIGURE 6. Moderate airflow limitation in a
subject with asthma.
12
10
8
6
4
2
0
-2
-4
-6
-8
Flow L·s
-1
0
123456
Volume L
FIGURE 7. Severe airflow limitation in a subject
with chronic obstructive pulmonary disease.
12
10
8
6
4
2
0
-2
-4
-6
-8
Flow L·s
-1
0
123456
Volume L
FIGURE 8. Variable intra-thoracic upper airway
obstruction.
12
10
8
6
4
2
0
-2
-4
-6
-8
Flow L·s
-1
0
12 345 6
Volume L
FIGURE 9. Variable extra-thoracic upper airway
obstruction.
12
10
8
6
4
2
0
-2
-4
-6
-8
Flow L·s
-1
0
12345 6
Volume L
FIGURE 10. Fixed upper airway obstruction
shown by three manoeuvres.
STANDARDISATION OF SPIROMETRY M.R. MILLER ET AL.
328
VOLUME 26 NUMBER 2 EUROPEAN RESPIRATORY JOURNAL

VC AND IC MANOEUVRE
Definitions
VC and IVC
The VC is the volume change at the mouth between the position
of full inspiration and complete expiration, expressed in litres at
BTPS. The slow VC can be derived in two ways. The expiratory
vital capacity (EVC) is the maximal volume of air exhaled from
the point of maximal inhalation. The IVC is the maximal volume
of air inhaled from the point of maximal exhalation, achieved by
a slow expiration from end-tidal inspiration. These manoeuvres
are unforced, except at the point of reaching RV or TLC,
respectively, where extra effort is required [36].
IC
Inspiratory capacity (IC) is volume change recorded at the
mouth when taking a slow full inspiration with no hesitation,
from a position of passive end-tidal expiration, i.e. FRC, to a
position of maximum inspiration, expressed in litres at BTPS.
IC is an indirect estimate of the degree of lung hyperinflation at
rest, and is useful to assess changes in FRC with pharmaco-
logical interventions and physical exercise [37–41].
Equipment
For measurements of VC and IC, the spirometer or flow meter
must comply with the requirements for FVC (as described
previously) and be capable of accumulating volume for o30 s.
Expiratory manoeuvres or, ideally, both inspiratory and
expiratory manoeuvres should be included in the display of
VC manoeuvre. Regardless of whether the inspiratory or
expiratory manoeuvre is used for deriving measurements, a
display of the entire recorded VC manoeuvre must be
provided. The maximal expiratory volume must be assessed
to determine whether the subject has obtained a plateau in the
expiratory effort. For display of the slow VC, the time scale
may be reduced to 5 mm?s
-1
.
Test procedure
VC
VC can be measured using conventional spirometers. It may
also be recorded from equipment used to measure static lung
volumes and their subdivisions [42]. For slow VC, a maximum
of four manoeuvres is a practical upper limit. It is preferable
that VC manoeuvres be performed before FVC manoeuvres
because of the potential for muscular fatigue and volume
history effects, where, after maximal inspiratory efforts, some
patients with severe airways obstruction return to a falsely
high level of FRC or RV, due to gas trapping or stress
relaxation [3]. The VC manoeuvre may be considered either as
an IVC, where the subject inhales completely from a position of
full expiration, or as an EVC, where the subject exhales
completely from a position of full inspiration. Figure 11 shows
the recording of IVC and figure 12 shows an EVC recording.
Important differences between inspiratory (i.e. IVC) and
expiratory (i.e. EVC) manoeuvres may be observed in patients
with airways obstruction [43, 44].
The test is begun by instructing the subject in the VC
manoeuvre and demonstrating the appropriate technique. It
is important that subjects understand they must completely fill
and empty their lungs. The VC manoeuvre is performed with
the subject using a mouthpiece and wearing a nose clip. The
manoeuvre is not forced; it is performed in a relaxed manner,
except near end-inspiration and end-expiration. The subject
exhales completely to RV, then inhales to TLC, and finally
exhales to RV again. The technician should encourage the
subject to reach maximal inhaled and exhaled volumes with a
relatively constant flow. The exhalation should not be unduly
slow, as this can lead to underestimation of VC. Technicians
should observe the subject carefully to ensure that his/her lips
are sealed, nothing obstructs the mouthpiece, no leaks occur,
and that TLC and RV are reached.
Alternatively, the subject inhales maximally, inserts the
mouthpiece just past his/her front teeth, seals his/her lips
around the mouthpiece, and blows slowly and evenly until
there is no volume change (,0.025 L) for a 1-s period (see End
of test criteria section). Patients with neuromuscular disease
may need assistance in maintaining a tight seal at the mouth.
The technician must observe the subject’s inhalation to ensure
TLC
IC
ERV
IVC
FRC
RV
Tidal breathing
Inspiration
Expiration
Time
FIGURE 11. Tracing of tidal breathing followed by an expiratory manoeuvre to
residual volume (RV), followed by a full inspiration to total lung capacity (TLC) to
record inspiratory vital capacity (IVC) and inspiratory capacity (IC). FRC: functional
residual capacity; ERV: expiratory reserve volume.
Tidal breathing
TLC
FRC
RV
IC
EVC
FIGURE 12. Tracing of tidal breathing followed by an inspiratory manoeuvre to
total lung capacity (TLC) to record inspiratory capacity (IC), followed by a full
expiration to residual volume (RV) to record expiratory reserve volume (EVC). FRC:
functional residual capacity.
M.R. MILLER ET AL. STANDARDISATION OF SPIROMETRY
c
EUROPEAN RESPIRATORY JOURNAL VOLUME 26 NUMBER 2 329
that it is complete, and that air is not exhaled while the
mouthpiece is being inserted. The technician should assure
that the expiratory manoeuvre is not forced. In healthy
subjects, adequate maximal inspiratory and expiratory levels
are achieved within 5–6 s.
IC
Subjects should be tested in the seated position wearing a nose
clip with no air leaks between the mouth and the mouthpiece.
Subjects should be relaxed (shoulders down and relaxed) and
asked to breathe regularly for several breaths until the end-
expiratory lung volume is stable (this usually requires at least
three tidal manoeuvres). They are then urged to take a deep
breath to TLC with no hesitation. Figure 12 shows a tracing
from the recording of IC.
Use of a nose clip
The use of a nose clip is encouraged in VC measurements,
since some people breathe through the nose when performing
a slow VC manoeuvre. A nose clip must be used when
performing inspiratory manoeuvres such as the IVC or IC.
Within-manoeuvre evaluation
These are the same as for FVC EOT criteria as described
previously. There must be no leak at the mouth, no hesitation
during the manoeuvre, and no obstruction of the mouthpiece
(see Additional criteria section). The IC may be underestimated
if the inspiratory manoeuvre is too slow due to poor effort or
hesitation, or if there is premature closure of the glottis.
Between-manoeuvre evaluation
As with spirometry, a minimum of three acceptable VC
manoeuvres must be obtained. If the difference in VC between
the largest and next largest manoeuvre is .0.150 L, additional
trials should be undertaken. Meeting repeatability criteria may
require that up to, but usually no more than, four manoeuvres
are performed, with a rest period of o1 min between the
manoeuvres. Large variability in this test is often due to
incomplete inhalations. Volume–time curves from the best two
VC manoeuvres must be retained. For the IC, at least three
acceptable manoeuvres should be performed. The mean
coefficient of variation for IC in chronic airflow obstruction
has been found to be 5 ¡3% [39].
Test result selection
For VC, the largest value from at least three acceptable
manoeuvres should be reported. For IC, the average of at least
three manoeuvres should be reported.
PEAK EXPIRATORY FLOW
Studies on the measurement of PEF are ongoing. Recent
evidence has suggested that the previously applied standards
may allow incorrect measurements to be made [45], and it is
possible that more stringent requirements may be required. A
further statement will be made when the position on the
clinical significance of this is clear. However, since PEF
measurements are part of asthma-management programmes,
the previous recommendations [3, 46] are reiterated here.
Other instantaneous flow measurements (e.g. FEF
50%, FEF75%)
are not proven to be superior to conventional spirometric
indices in a clinical setting, and, therefore, are not considered
further.
Definition
PEF is the highest flow achieved from a maximum forced
expiratory manoeuvre started without hesitation from a posi-
tion of maximal lung inflation [46]. When it is obtained from
flow–volume curve data, it is expressed at BTPS in L?s
-1
. The
defining characteristics of the flow–time curve, in relation to
PEF, are the time taken for flow to rise from 10% of PEF to 90%
of PEF, i.e. the rise time (RT), and the duration that flow is .90%
of PEF, called the dwell time (DT). When PEF is obtained with
portable monitoring instruments, it is expressed in L?min
-1
.
Equipment
Ideally, PEF should be recorded by an instrument that
primarily records flow. Measuring PEF requires an instrument
that has a flat frequency response (¡5%) up to 15 Hz [46].
Although there is evidence of significant frequency content in
PEF up to 20 Hz [47], it is recommended, at this stage, that
manufacturers achieve a goal of recording fidelity up to 15 Hz.
The PEF must be measured with an accuracy of ¡10%
or ¡0.3 L?s
-1
(20 L?min
-1
), whichever is the greater. Mean
instrument resistance measured across the range of the
instrument should be ,2.5 cmH
2
O?L
-1
?s
-1
(0.25 kPa?L
-1
?s
-1
;
table 6). PEF is sensitive to the resistance of the meter; for
example, a resistance of 0.25 kPa?L
-1
?s
-1
decreases PEF by ,8%
compared with PEF measured with a low-resistance pneumo-
tachograph [48].
Intra-instrument repeatability must be ,5% or 0.150 L?s
-1
(10 L?min
-1
), whichever is the greater. Inter-device reproduci-
bility must be ,10% or 0.300 L?s
-1
(20 L?min
-1
), whichever is
the greater. Calculating PEF by differentiating volume–time
data may introduce noise; hence, a parabolic-fitting algorithm
may be used [2] as a smoothing procedure.
Equipment validation is covered in the Test signals for PEF
meter testing section.
Test procedure
PEF is dependent on effort and lung volume, with subject
cooperation being essential. PEF must be achieved as rapidly
as possible and at as high a lung volume as possible, in order
to obtain the maximum value [49]. The subject must be
encouraged to blow as vigorously as possible. The neck should
be in a neutral position, not flexed or extended, and the subject
must not cough. A nose clip is not necessary.
After the point of full lung inflation, the subject must deliver
the blow without any delay. Hesitating for as little as 2 s or
flexing the neck allows the tracheal visco-elastic properties to
relax and PEF to drop by as much as 10% [50]. Tonguing,
spitting or coughing at the start of the blow may falsely raise
the recorded PEF in some devices.
In the laboratory, the subject must perform a minimum of three
PEF manoeuvres. When PEF is a self-administered recording,
it is important that the subject has been adequately taught how
to perform the test, when to perform it and what action to take
depending on the resulting value obtained. Regular checks of
the patient’s PEF technique and meter are an important part of
the follow-up.
STANDARDISATION OF SPIROMETRY M.R. MILLER ET AL.
330
VOLUME 26 NUMBER 2 EUROPEAN RESPIRATORY JOURNAL
Within-manoeuvre evaluation
The subject must be observed to ensure a good seal at the
mouth, no hesitation occurred, and there was no abnormal
start to the manoeuvre.
Between-manoeuvre evaluation
The PEF values and their order must be recorded so that
manoeuvre-induced bronchospasm can be detected. If the
largest two out of three acceptable blows are not reproducible
within 0.67 L?s
-1
(40 L?min
-1
), up to two additional blows can
be performed. Ninety-five per cent of untrained healthy
subjects and patients can reproduce PEF to within 0.67 L?s
-1
(40 L?min
-1
), and 90% to within 0.5 L?s
-1
(30 L?min
-1
) [48]. If
satisfactory repeatability has not been in achieved in five
attempts, more are not likely to be helpful [51].
Test result selection
The largest value from at least three acceptable blows is
recorded.
MAXIMUM VOLUNTARY VENTILATION
This test has been largely superseded by FEV
1, which was
defined as the index from a single maximum forced expiratory
manoeuvre that best correlated with maximum voluntary
ventilation (MVV). If FEV
1 is available, then MVV has little
additional contribution to make in a clinical setting. However,
it may be useful in those conditions where ventilatory capacity
may be impaired by mechanisms that are different from those
affecting FEV
1 [26].
Definition
The MVV is the maximum volume of air a subject can breathe
over a specified period of time (12 s for normal subjects). It is
expressed in L?min
-1
at BTPS.
Equipment
A spirometer used for measuring MVV must have an
amplitude–frequency response that is flat (¡10%) from zero
to o4 Hz, at flows of up to 12 L?s
-1
, over the volume range.
The time for exhaled volume integration or recording must be
no less than 12 s and no more than 15 s [52]. The indicated time
must be accurate to within ¡3%. The MVV must be measured
with an accuracy of ¡10% of reading or ¡15 L?min
-1
,
whichever is greater.
The evaluation of equipment is covered in the Test signals for
MVV testing section.
Test procedure
The technician should provide proper instructions and
demonstrate the manoeuvre prior to the start of testing.
The subject should be tested in the sitting position wearing
a nose clip. After the subject makes an airtight seal around
the mouthpiece, at least three resting tidal breaths should be
obtained, followed by breathing as rapidly and deeply as
possible. The tongue and teeth must be positioned so as to
not obstruct airflow. The technician should enthusiastically
coach the subject throughout the manoeuvre, and may need
to suggest faster or slower breathing to achieve an ideal rate
of 90–110 breaths?min
-1
[53, 54], although subjects with
disease may not always achieve this rate. The technician
will need to carefully observe the subject with occasional
glances at the tracing to help the subject to obtain an
acceptable manoeuvre. An acceptable manoeuvre should be
performed with maximal effort without evidence of leakage,
hesitation or measurement artefact. The subject is instructed
to breathe as deeply and rapidly as possible and the tidal
volume (V
T) during the manoeuvre should be greater than
the subject’s resting V
T.
The test interval (e.g. 12 s) should be reported. A rest between
manoeuvres will improve subsequent efforts.
The MVV should be calculated from the sum of all individual
exhalations, multiplied by the appropriate BTPS correction
factor during the best 12 s of the manoeuvre. From a technical
standpoint, changes in respiratory rate or V
T during the
manoeuvre will influence test results.
Within-manoeuvre evaluation
In normal subjects, the goal for an acceptable MVV should be a
V
T that is ,50% of the VC, with a breathing frequency that is
,90 breaths?min
-1
[54]. It is unlikely that an acceptable
manoeuvre will be obtained when the breathing frequency is
,65 breaths?min
-1
[54]. However, since there are little data on
MVV acceptability criteria, no specific breathing frequency or
volume is required. The emphasis should be on maximal effort
with a goal of 90 breaths?min
-1
and a volume representing
,50% of the VC. V
T during the manoeuvre is probably not as
important as breathing frequency, since patients tend to
breathe on the portion of the expiratory curve where air is
best moved at a given frequency.
Between-manoeuvre evaluation
The subject should perform a minimum of two acceptable
manoeuvres. There are no clinical studies addressing repeat-
ability; however, additional trials should be considered when
the variability between acceptable manoeuvres exceeds 20%.
Test result selection
The highest acceptable MVV (L?min
-1
BTPS) and MVV rate
(breaths?min
-1
) should be reported. An MVV/(406FEV1)
,0.80 indicates that the MVV is low relative to the FEV
1,
and suggests disease or poor effort. Volume versus time
tracings from at least two acceptable manoeuvres should be
retained and available for inspection.
TECHNICAL CONSIDERATIONS
Minimal recommendations for spirometry systems
Accurate results require accurate equipment. Spirometer equip-
ment recommendations apply to all spirometers and are minimal
requirements. In some circumstances, it may be appropriate
to exceed these requirements (i.e. in some research/
surveillance applications). Instrumentation recommendations
should be followed to provide accurate spirometric data and
information that is comparable from laboratory to laboratory and
from one time period to another [1]. The accuracy of a spirometry
system depends on characteristics of the entire system, from the
volume or flow transducer and the use of an in-line filter, to
the recorder, display or processor. Changes in any aspect of
the equipment or errors at any step in the process can affect the
accuracy of the results. For example, if the BTPS correction factor
is wrong, an accurately measured FVC will be incorrectly
reported.
M.R. MILLER ET AL. STANDARDISATION OF SPIROMETRY
c
EUROPEAN RESPIRATORY JOURNAL VOLUME 26 NUMBER 2 331
Spirometers and PEF meters are not required to measure all of
the indices in table 6, but must meet the recommendations for
those that are measured. Accuracy and repeatability recom-
mendations apply over the entire volume range of the
instrument.
BTPS correction
All spirometry values should be reported at BTPS by any
method (measuring temperature and barometric pressure)
proven effective by the manufacturer. For volume-type spirom-
eters, the temperature inside the spirometer should be mea-
sured for each breathing manoeuvre. Regardless of the BTPS
correction technique used, the ambient temperature must
always be recorded with an accuracy of ¡1
˚
C. In situations
where the ambient air temperature is changing rapidly (.3
˚
Cin
,30 min), continuous temperature corrections may be neces-
sary. Spirometer users should be aware of potential problems
with testing performed at lower ambient temperatures: 17
˚
Cis
the lower limit [55–63] for ambient temperature, unless a
manufacturer states that their spirometer will operate accurately
at lower ambient temperatures. If barometric pressure is not
used in calculating the BTPS correction factor, the range of
barometric pressures over which the BTPS correction factor is
valid must be published by the manufacturer.
Comments
The rationale for this recommendation is based, in part, on the
problems with finite cooling times of gases in volume-type
spirometers [55–57] and the problems of estimating BTPS
correction factors for flow devices [58–60]. When a subject
performs an FVC manoeuvre, the air leaving the lungs is ,33–
35
˚
C [61, 62] and saturated with water vapour. If the expired
gas is assumed to be at BTPS, an error of ,1% will result. Most
volume-type spirometers assume instantaneous cooling of the
air as it enters the spirometer. This is not always the case, and
FEV
t can be incorrectly reported because of it. For capillary
and screen pneumotachometers, the signal depends on gas
viscosity, which increases with increasing temperature.
Therefore, for pneumotachometers, a different correction factor
is needed for recording patients as compared with recording
from the calibrating syringe. Also, correction factors will be
different for inspiratory and expiratory manoeuvres. It is
usually assumed that expired gas does not cool as it passes
through the flow sensor. This may not be the case, particularly
with unheated flow sensors [58, 59]. The error will increase if
the flow sensor is located further from the mouth and more
cooling occurs, as is the case when a filter is placed in front of
the flow sensor. Water condensation within or on the surfaces
of a flow sensor may alter its calibration.
Depending on environmental temperature, the BTPS correction
factor may be as large as 10%. The method used to calculate or
estimate the BTPS factor can potentially introduce significant
errors; examples and a fuller explanation can be found
elsewhere [3, 4].
Changes in spirometer temperature can be a source of
variability. Spirometer temperature should be measured and
not assumed to be constant, even over the course of one testing
TABLE 6
Range and accuracy recommendations specified for forced expiratory manoeuvres
Test Range/accuracy (BTPS) Flow range
L?s
-1
Time s Resistance and
back pressure
Test signal
VC 0.5–8 L, ¡3% of reading or
¡0.050 L, whichever is greater
0–14 30 3-L Calibration syringe
FVC 0.5–8 L, ¡3% of reading or
¡0.050 L, whichever is greater
0–14 15 ,1.5 cmH
2
O?L
-1
?s
-1
(0.15 kPa?L
-1
?s
-1
)
24 ATS waveforms,
3-L Cal Syringe
FEV
1 0.5–8 L, ¡3% of reading or
¡0.050 L, whichever is greater
0–14 1 ,1.5 cmH
2
O?L
-1
?s
-1
(0.15 kPa?L
-1
?s
-1
)
24 ATS waveforms
Time zero The time point from which
all FEV
t measurements are taken
Back extrapolation
PEF Accuracy: ¡10% of reading or
¡0.30 L?s
-1
(20 L?min
-1
), whichever is
greater; repeatability: ¡5% of reading
or ¡0.15 L?s
-1
(10 L?min
-1
), whichever
is greater
0–14 Mean resistance at 200, 400,
600 L?min
-1
(3.3, 6.7, 10 L?s
-1
)
must be ,2.5 cmH
2
O?L
-1
?s
-1
(0.25 kPa?L
-1
?s
-1
)
26 ATS flow waveforms
Instantaneous
flows (except PEF)
Accuracy: ¡5% of reading or
¡0.200 L?s
-1
, whichever is greater
0–14 ,1.5 cmH
2
O?L
-1
?s
-1
(0.15 kPa?L
-1
?s
-1
)
Data from manufacturers
FEF
25–75% 7.0 L?s
-1
, ¡5% of reading or
¡0.200 L?s
-1
, whichever is greater
¡14 15 Same as FEV
1 24 ATS waveforms
MVV 250 L?min
-1
at VT of 2 L within
¡10% of reading or ¡15 L?min
-1
,
whichever is greater
¡14 (¡3%) 12–15 ,1.5 cmH
2
O?L
-1
?s
-1
(0.15 kPa?L
-1
?s
-1
)
Sine wave pump
BTPS: body temperature and ambient pressure saturated with water vapour; VC: vital capacity; FVC: forced vital capacity; ATS: American Thoracic Society; FEV
1: forced
expiratory volume in one second; FEV
t: forced expiratory volume in t seconds; PEF: peak expiratory flow; FEF25–75%: mean forced expiratory flow between 25% and 75%
of FVC; MVV: maximum voluntary ventilation; V
T: tidal volume.
STANDARDISATION OF SPIROMETRY M.R. MILLER ET AL.
332
VOLUME 26 NUMBER 2 EUROPEAN RESPIRATORY JOURNAL
session. For volume spirometers, errors up to 6% in FEV1 and
FVC can occur if ambient temperature is used instead of
internal spirometer temperature [64]. For volume spirometers,
the temperature inside the spirometer should be measured for
each breathing manoeuvre.
Test signals for spirometer testing
The diversity of FVC manoeuvres encountered in clinical
practice is currently best simulated by the 24 standard volume–
time waveforms developed by the ATS [3] and H
ANKINSON and
G
ARDNER [65]. These waveforms can be used to drive a
computer-controlled mechanical syringe, or its equivalent, for
testing actual hardware and software [66, 67], or, when put in a
digital form, they can evaluate only the software. Computer-
controlled mechanical syringes (i.e. pump systems) used for
validation should be accurate within ¡50 mL, which is 0.5% of
their full range up to 10 L for FVC and FEV
1. Pump systems
may have accuracy values better than this for many profiles,
but reproduce less accurately those test profiles with short DTs
and RTs to peak flow [68, 69]. The ATS spirometry statement
[3] shows the measured values for each of the 24 standard
waveforms. On request, the ATS can provide these waveforms
in an electronic format. Appropriate corrections for using gas
at the ambient temperature and humidity instead of BTPS may
need to be made for some mechanical syringe–spirometer
combinations.
Method
A production spirometer is connected to the pump system for
testing, orientated as it would be to test human subjects.
Connecting tubing must be kept to the minimum (,0.300 L)
and must not be distensible. If an in-line filter is required for
testing human subjects, one must be included when the
instrument is tested. Each of the 24 ATS waveforms is
discharged into the spirometer five times under ambient
conditions, and all of the readings are recorded.
BTPS conditions are simulated by discharging waveforms 1–4
to the spirometer three times, using air heated to 37¡1
˚
C and
at .98% relative humidity. The time between each of the three
tests should be , 2 min.
Accuracy test
The average of the five tests under ambient conditions is
compared with the standard value in the following way:
Deviation~average{standard ð1Þ
Percentage deviation~100|(average{standard)=standard ð2Þ
The accuracy validation limits for volumes, which include the
waveform-generator inaccuracy, are ¡3.5% of reading or
¡0.100 L, whichever is greater. An accuracy error occurs if
the deviation (for volumes ,2.857 L) or percentage deviation
(for volumes .2.857 L) exceed these limits. These limits
include the allowable inaccuracy of the pump system.
Acceptable spirometer performance is defined as fewer than
three accuracy errors for either FVC or FEV
1 across the 24
waveforms (,5% error rate).
The average FVC and FEV
1 values of the three tests simulating
BTPS conditions are compared with the standard values. The
validation limits for these tests under BTPS conditions are
¡4.5% or 0.200 L, whichever is the greater, and these limits
include the allowable inaccuracy for the pump system.
Acceptable spirometer performance under BTPS conditions is
defined as the accuracy requirement being met for all of the
four profiles used.
Repeatability test
The FEV
1 and FVC data from the accuracy test are used to
derive the span of the five recordings:
Span~maximum minimum ð3Þ
Percentage span~100|span=average ð4Þ
The repeatability validation limits for the volume measured at
ambient conditions are ¡3.5% or ¡0.100 L, whichever is
the greater, and, for BTPS conditions, ¡4.5% or ¡ 0.200 L,
whichever is the greater. A repeatability error occurs if the
span (for volumes ,2.857 L at ambient or 4.444 L at BTPS) or
percentage span (for volumes above this) exceeds these limits.
Acceptable spirometer performance for repeatability under
ambient conditions is defined as fewer than three accuracy
errors for either FVC or FEV
1 across the 24 profiles (,5% error
rate). For BTPS conditions, the acceptable spirometer perfor-
mance for repeatability is defined as the accuracy requirement
being met for all of the four profiles.
Test signals for PEF meter testing
The 26 flow–time ATS waveforms were chosen to represent a
range of PEF profiles suitable for delivery by mechanical
syringe or pump systems to test PEF meters [3]. The range of
profiles and method of delivery may need to be revised, as
research on PEF measurement continues [45]. The mechanical
syringe or suitable pump system used to validate PEF
measuring equipment must have an accuracy of ¡2% in
delivering PEF. Pump systems may have difficulty meeting
this accuracy standard for profiles more demanding than the
set of 26 [68, 69]. Recent evidence suggests that the frequency
content in the first second of the blow that contributes to PEF is
higher [47] than previously determined [70, 71]. The 26
waveforms may not cover the range of RT and DT found in
,25% of the client population [72], and, hence, more
demanding test profiles may be required in future [45].
Method
Two randomly chosen production models of the flow meters
should each have the 26 waveforms delivered to them five
times under ambient conditions and the readings recorded.
Any waveforms with a PEF outside the meter’s stated
operational range would not be included in the testing
sequence. Appropriate correction factors for testing under
ambient conditions should be applied as recommended by the
manufacturer.
Accuracy test
The average reading for each of the two meters is compared
with the standard, as for volumes.
The accuracy validation limits are ¡12% or ¡25 L?min
-1
,
whichever is the larger, and these limits include the 2%
inaccuracy limit for the waveform generator. An accuracy error
M.R. MILLER ET AL. STANDARDISATION OF SPIROMETRY
c
EUROPEAN RESPIRATORY JOURNAL VOLUME 26 NUMBER 2 333

for a given meter and given waveform occurs if the deviation
and percentage deviation exceed these limits.
Acceptable performance is defined as fewer than three
accuracy errors out of the total of 52 tests (26 waveforms,
two meters).
Repeatability test
Flow waveforms 1, 4, 8 and 25 are discharged three times to
each of 10 production meters. The repeatability validation
limits are ¡6% or ¡15 L?min
-1
, whichever is the greater, and
these limits include 1% for waveform-generator variability. A
repeatability error occurs if the span and percentage span
exceed these limits.
Acceptable performance is defined as six or fewer errors in the
120 tests (i.e. maximum error rate of 5%).
Test signals for MVV testing
A spirometry system used to measure MVV should be tested
under ambient conditions with a pump producing a sinusoidal
waveform, with stroke volumes up to 2 L using the four
patterns of delivery previously specified [3]. Testing at BTPS is
not required, and each pattern is tested twice. The accuracy
validation limits of the spirometer used for measuring MVV
with flows up to 250 L?min
-1
are ¡10.5% of reading or
¡20 L?min
-1
, whichever is greater. The pressure at the
mouthpiece must not exceed ¡10 cmH
2
O (1 kPa) at any point
during MVV testing. These requirements apply to volume
spirometers throughout their volume range.
Acceptable performance is defined as no errors in the eight
tests (four patterns, twice).
ABBREVIATIONS
Table 7 contains a list of abbreviations and their meanings,
which will be used in this series of Task Force reports.
TABLE 7
List of abbreviations and meanings
ATPD Ambient temperature, ambient pressure, and dry
ATPS Ambient temperature and pressure saturated with water vapour
BTPS Body temperature (i.e. 37
˚
C), ambient pressure, saturated with
water vapour
C Centigrade
CFC Chlorofluorocarbons
cm Centimetres
COHb Carboxyhaemoglobin
D
L,CO Diffusing capacity for the lungs measured using carbon
monoxide, also known as transfer factor
D
L,CO/VA Diffusing capacity for carbon monoxide per unit of alveolar
volume, also known as K
CO
DM Membrane-diffusing capacity
DT Dwell time of flow .90% of PEF
EFL Expiratory flow limitation
ERV Expiratory reserve volume
EV Back extrapolated volume
EVC Expiratory vital capacity
F
A,X Fraction of gas X in the alveolar gas
F
A,X,t Alveolar fraction of gas X at time t
FEF
25-75% Mean forced expiratory flow between 25% and 75% of FVC
FEF
X% Instantaneous forced expiratory flow when X% of the FVC has
been expired
FEV1 Forced expiratory volume in one second
FEV
t Forced expiratory volume in t seconds
F
E,X Fraction of expired gas X
FIF
X% Instantaneous forced inspiratory flow at the point where X% of the
FVC has been inspired
F
I,X Fraction of inspired gas X
FIVC Forced inspiratory vital capacity
FRC Functional residual capacity
FVC Forced vital capacity
H
2
O Water
Hb Haemoglobin
Hg Mercury
Hz Hertz; cycles per second
IC Inspiratory capacity
IVC Inspiratory vital capacity
K
CO Transfer coefficient of the lung (i.e.DL,CO/VA)
kg Kilograms
kPa Kilopascals
L Litres
L?min
-1
Litres per minute
L?s
-1
Litres per second
lb Pounds weight
MEF
X% Maximal instantaneous forced expiratory flow where X% of the
FVC remains to be expired
MFVL Maximum flow–volume loop
mg Milligrams
MIF Maximal inspiratory flow
mL Millilitres
mm Millimetres
MMEF Maximum mid-expiratory flow
ms Milliseconds
MVV Maximum voluntary ventilation
P
A,O
2
Alveolar oxygen partial pressure
PB Barometric pressure
PEF Peak expiratory flow
P
H
2
O Water vapour partial pressure
P
I,O
2
Inspired oxygen partial pressure
h (theta) Specific uptake of CO by the blood
RT Rise time from 10% to 90% of PEF
RV Residual volume
s Seconds
STPD Standard temperature (273 K, 0
˚
C), pressure (101.3 kPa,
760 mmHg) and dry
TB Tuberculosis
TGV (or V
TG) Thoracic gas volume
t
I Time taken for inspiration
TLC Total lung capacity
Tr Tracer gas
t
tot Total time of respiratory cycle
V
A Alveolar volume
V
A,eff Effective alveolar volume
VC Vital capacity
V
c Pulmonary capillary blood volume
V
D Dead space volume
V
I Inspired volume
V
S Volume of the expired sample gas
mg Micrograms
TABLE 7
(Continued)
STANDARDISATION OF SPIROMETRY M.R. MILLER ET AL.
334
VOLUME 26 NUMBER 2 EUROPEAN RESPIRATORY JOURNAL

APPENDIX
Proposal for a standard data format for spirometry
This proposal would not preclude the use of other data
formats, but would require that a spirometer should at least be
able to output data in the required format. The advantage of a
standard format is the ease of moving data into data
repositories, such as quality control, healthcare and research
databases. It should simplify and reduce the cost of data
transfer when users change instrument models and manufac-
turers. Easier transfer of data into healthcare databases has the
potential for improving the utility of lung function by making
more complete data readily available to clinicians and
healthcare researchers. In research and clinical settings, a
standard data format should simplify and reduce the cost of
transferring data into quality control software and could
contribute to improved overall test quality. Finally, it is time
for this change; pulmonary function is one of the last medical
arenas without a standard data format.
Proposed format
The spirometry data file will consist of an American Standard
Code for Information Interchange, comma-delineated file with
variable length records. Comma-delineated text files are easily
generated and are standard import formats for several
database programs. Although some redundancies will exist,
each record shall represent one curve and will be terminated
with a carriage return and line feed. The ATS will distribute
examples of this data format from their web site.
Table 8 shows a list of parameters that must be included in
every record. If a parameter is unavailable, the space must
remain blank (‘‘,,’’). The flow–time data points must be
provided with a sampling interval of 0.01 s (100 samples?s
-1
)
in mL?s
-1
. If necessary, interpolation or other techniques must
TABLE 8
List of parameters
#
ID (patient identification)
Patient name
Data type (SP followed by E5expiratory or I5Inspiratory, followed by S5single
or B5best curve)
Barometric pressure (mmHg)
Temperature (
˚
C) used in BTPS calculation
Relative humidity (%)
FVC quality attribute (A, B, C, D or F)
FEV
1 quality attribute (A, B, C, D or F)
Effort attribute (A, B, C, D or F)
Interpretation code (see ATS interpretation scheme)
Deleted manoeuvre (Y or N)
Acceptable manoeuvre (Y or N)
Technician quality control code (A, B, C, D or F)
Computer quality code (A, B, C, D or F)
Plateau achieved (Y or N)
Review (N or R for ‘‘needs review’’ or ‘‘was reviewed’’)
Date of review (DD/MM/YYYY)
Reviewer initials
BTPS factor (x.xxx)
Spirometer manufacturer
Spirometer model
Spirometer serial number
Spirometer type
Testing facility name
City
State/region
Zip/post code
Country
E-mail
Phone number
Calibration date (DD/MM/YYYY)
Calibration time (HH:MM)
Calibration result (P or F for ‘‘passed’’ or ‘‘failed’’)
Date (DD/MM/YYYY)
Time (HH:MM)
Technician ID (technician identification code or initials)
Manoeuvre number
Age (integer years)
Height (cm)
Weight (kg)
Sex (M or F)
Race (2-character race code)
Date of birth (DD/MM/YYYY)
Reference values source (first author surname and date of publication, e.g.
‘‘Knudson 1983’’)
Reference values correction factor (x.xx, 1.00 for no correction)
Testing position (standing, sitting or supine)
Test type (pre-, post-, bronchodilator, methacholine concentration or dose)
FVC (mL)
Extrapolated volume (mL)
FEV
1 (mL)
FEV
6 (mL)
PEF (mL?s
-1
)
FEF
25–75% (mL?s
-1
)
VC (mL)
Forced expiratory time (s)
Time to PEF (ms)
Predicted FVC (mL)
Predicted FEV
1 (mL)
Predicted FEV
6 (mL)
Predicted FEV
1/FVC% (xxx.x%)
Predicted FEV
1/FEV6% (xxx.x%)
Comments text
Original sampling interval (ms)
Blank 1 or FEF
25%
Blank 2 or FEF50%
Blank 3 or FEF75%
Blank 4 or FEF90%
Blank 5
Blank 6
Blank 7
Blank 8
Blank 9
Blank 10
Number of data points
Flow data points (mL?s
-1
; variable number contained in number of data points)
Carriage return
Line feed
#
: All text type variables should be enclosed with double quotes (‘‘) to prevent
confusion with control or data separator type characteristics.
TABLE 8
(Continued)
M.R. MILLER ET AL. STANDARDISATION OF SPIROMETRY
c
EUROPEAN RESPIRATORY JOURNAL VOLUME 26 NUMBER 2 335
ACKNOWLEDGEMENTS
M.R. Miller: University Hospital Birmingham NHS Trust,
Birmingham, UK; J. Hankinson: Hankinson Consulting, Inc.,
Valdosta, GA, USA; V. Brusasco: Universita
`
degli Studi di
Genova, Genova, Italy; F. Burgos: Hospital Clinic Villarroel,
Barcelona, Spain; R. Casaburi: Harbor UCLA Medical
Center, Torrance, CA, USA; A. Coates: Hospital for Sick
Children, Toronto, ON, Canada; R. Crapo and R. Jensen:
LDS Hospital, Salt Lake City, UT, USA; P. Enright: 4460
E Ina Rd, Tucson, AZ, USA; C.P.M. van der Grinten:
University Hospital of Maastrict, Maastricht, the
Netherlands; P. Gustafsson: Queen Silvias Children’s
Hospital, Goteborg, Sweden; D.C. Johnson: Massachusetts
General Hospital and Harvard Medical School, Boston, MA,
USA; N. MacIntyre: Duke University Medical Center,
Durham, NC, USA; R. McKay: Occupational Medicine,
Cincinnati, OH, USA: D. Navajas: Universitat de Barcelona
- IDIBAPS, Barcelona, Spain; O.F. Pedersen: University of
Aarhus, Aarhus, Denmark; R. Pellegrino: Azienda
Ospedaliera S. Croce e Carle, Cuneo, Italy; G. Viegi: CNR
Institute of Clinical Physiology, Pisa, Italy; J. Wagner:
Pharmaceutical Research Associates, Inc., Lenexa, KS, USA.
REFERENCES
1 Renzetti AD Jr. Standardization of spirometry. Am Rev
Respir Dis 1979; 119: 831–838.
2 American Thoracic Society. Standardization of spirometry:
1987 update. Am Rev Respir Dis 1987; 136: 1285–1298.
3 American Thoracic Society. Standardization of spirometry,
1994 update. Am J Respir Crit Care Med 1995; 152:
1107–1136.
4 Quanjer PH, ed. Standardized lung function testing.
Report Working Party Standardization of Lung Function
Tests. European Community for Coal and Steel. Bull Eur
Physiopathol Respir 1983; 19: Suppl. 5, 1–95.
5 Quanjer PH, Tammeling GJ, Cotes JE, Pedersen OF,
Peslin R, Yernault J-C. Lung volume and forced ventilatory
flows. Report Working Party Standardization of Lung
Function Tests, European Community for Steel and Coal.
Official Statement of the European Respiratory Society. Eur
Respir J 1993; 6: Suppl. 16, 5–40.
6 Morgan KC. The assessment of ventilatory capacity
(committee recommendations). Chest 1975; 67: 95–97.
7 Gardner RM, Crapo RO, Billings RG, Shigeoka JW,
Hankinson JL. Spirometry: what paper speed? Chest 1983;
84: 161–165.
8 Gardner RM, Clausen JL, Crapo RO, et al. Quality
assurance in pulmonary function laboratories. Am Rev
Respir Dis 1986; 134: 626–627.
9 Morris AH, Kanner RE, Crapo RO, Gardner RM. Clinical
pulmonary function testing: a manual of uniform labora-
tory procedures. 2nd Edn. Salt Lake City, UT,
Intermountain Thoracic Society, 1984.
10 Townsend MC. The effects of leaks in spirometers on
measurement of pulmonary function. J Occup Med 1984; 26:
835–841.
11 Association for the Advancement of Medical
Instrumentation, Standard for spirometers (draft),
October 1980. AAMI Suite 602, 1901 N. Ft. Myer Drive,
Arlington, VA 22209–1699.
12 D’Angelo E, Prandi E, Milic-Emili J. Dependence of
maximal flow-volume curves on time course of preceding
inspiration. J Appl Physiol 1993; 75: 1155–1159.
13 Stoller JK, Basheda S, Laskowski D, Goormastic M,
McCarthy K. Trial of standard versus modified expiration
to achieve end-of-test spirometry criteria. Am Rev Respir
Dis 1993; 148: 275–280.
14 Bucca CB, Carossa S, Colagrande P, et al. Effect of
edentulism on spirometric tests. Am J Respir Crit Care
Med 2001; 163: 1018–1020.
15 Eigen H, Bieler H, Grant D, et al. Spirometric pulmonary
function in healthy preschool children. Am J Respir Crit
Care Med 2001; 163: 619–623.
16 Smith AA, Gaensler EA. Timing of forced expiratory
volume in one second. Am Rev Respir Dis 1975; 112:
882–885.
17 Horvath EP Jr, ed. Manual of spirometry in occupational
medicine. Division of Training and Manpower
Development, National Institutes for Occupational Safety
and Health. Cincinnati, NIOSH, 1981.
18 Hankinson JL, Gardner RM. Standard waveforms for
spirometer testing. Am Rev Respir Dis 1982; 126: 362–364.
19 Aurora P, Stocks J, Oliver C, et al. Quality control for
spirometry in preschoolchildren with and without lung
disease. Am J Crit Care Med 2004; 169: 1152–1159.
20 Desmond KJ, Allen PD, Demizio DL, Kovesi T, Coates AL.
Redefining end of test (EOT) criteria for pulmonary
function testing in children. Am J Respir Crit Care Med
1997; 156: 542–545.
21 Hankinson JL, Bang KM. Acceptability and reproducibility
criteria of the American Thoracic Society as observed in a
sample of the general population. Am Rev Respir Dis 1991;
143: 516–521.
22 Ferris BG Jr, Speizer FE, Bishop Y, Prang G, Weener J.
Spirometry for an epidemiologic study: deriving optimum
summary statistics for each subject. Bull Eur Physiopathol
Respir 1978; 14: 146–166.
23 Kanner RE, Schenker MB, Munoz A, Speizer FE.
Spirometry in children: methodology for obtaining optimal
results for clinical and epidemiological studies. Am Rev
Respir Dis 1983; 127: 720–724.
24 Swanney MP, Jensen RL, Crichton DA, Beckert LE,
Cardno LA, Crapo RO. FEV(6) is an acceptable surrogate
for FVC in the spirometric diagnosis of airway obstruction
and restriction. Am J Respir Crit Care Med 2000; 162:
917–919.
25 Paoletti P, Pistelli G, Fazzi P, et al. Reference values for
vital capacity and flow-volume curves from a general
population study. Bull Eur Physiopathol Respir 1986; 22:
451–459.
be used to provide the 0.01-s sampling interval. The record
length will vary, depending on the number of data points
present in the flow–time portions of the record. The curve data
must include o0.25 s of data points prior to the onset of the
inspiratory or expiratory manoeuvre.
Volume–time curves may be calculated by adding the flow–
time values (mL?s
-1
) and multiplying the sum by 0.01 s. To
obtain the highest precision, the sum of the flow values should
be calculated for each volume data point before multiplying by
0.01 s.
STANDARDISATION OF SPIROMETRY M.R. MILLER ET AL.
336
VOLUME 26 NUMBER 2 EUROPEAN RESPIRATORY JOURNAL
26 Pellegrino R, Viegi G, Enright P, et al. Interpretative
strategies for lung function tests. Eur Respir J 2005 (In
press).
27 Coates AL, Allen PD, MacNeish CF, Ho SL, Lands LC.
Effect of size and disease on expected deposition of drugs
administered using jet nebulization in children with cystic
fibrosis. Chest 2001; 119: 1123–1130.
28 Coates AL, Ho SL. Drug administration by jet nebulization.
Pediatr Pulmonol 1998; 26: 412–423.
29 Newman SP, Clark AR, Talaee N, Clark SW. Pressurized
aerosol deposition in the human lung with and without an
‘‘open’’ spacer device. Thorax 1989; 44: 706–710.
30 Tal A, Golan H, Grauer N, Aviram M, Albin D,
Quastel MR. Deposition pattern of radiolabeled salbutamol
inhaled from a meter-dose inhaler by means of a spacer
with mask in young children with airway obstruction. J
Pediatr 1996; 128: 479–484.
31 Newhouse MT. Asthma therapy with aerosols: are
nebulizers obsolete? A continuing controversy. J Pediatr
1999; 135: 5–8.
32 Coates AL, MacNeish CF, Lands LC, Meisner D,
Kelemen S, Vadas EB. A comparison of the availability of
tobramycin for inhalation from vented versus unvented
nebulizers. Chest 1998; 113: 951–956.
33 Devadason SG, Everard ML, Linto JM, LeSoue
¨
f PN.
Comparison of drug delivery form conventional versus
‘‘Venturi’’ nebulizers. Eur Respir J 1997; 10: 2479–2483.
34 Leach CL, Davidson PJ, Hasselquist BE, Boudreau RJ.
Lung deposition of hydofluoroalkane-134a beclometha-
sone is greater than that of chlorofluorocarbon fluticasone
and chlorofluorocarbon beclomethasone: a cross-over
study in healthy volunteers. Chest 2002; 122: 510–516.
35 Wildhaber JH, Devadason SG, Hayden MJ, Elber E,
Summers QA, LeSoue
¨
f PN. Aerosol delivery to wheezy
infants: a comparison between a nebulizer and two small
volume spacers. Pediatr Pulmonol 1997; 23: 212–216.
36 Guidelines for the measurement of respiratory function.
Recommendations of the British Thoracic Society and the
Association of Respiratory Technicians and Physiologists.
Respir Med 1994; 88: 165–194.
37 Babb TG, Viggiano R, Hurley B, Staats B, Rodarte JR. Effect
of mild-to-moderate airflow limitation on exercise capa-
city. J Appl Physiol 1991; 70: 223–230.
38 O’Donnell DE, Lam M, Webb KA. Spirometric correlates of
improvement in exercise performance after cholinergic
therapy in chronic obstructive pulmonary disease. Am J
Respir Crit Care Med 1999; 160: 542–549.
39 Pellegrino R, Rodarte JR, Brusasco V. Assessing the
reversibility of airway obstruction. Chest 1998; 114:
1607–1612.
40 Pellegrino R, Brusasco V. Lung hyperinflation and flow
limitation in chronic airway obstruction. Eur Respir J 1997;
10: 543–549.
41 Younes M, Kivinen G. Respiratory mechanics and breath-
ing pattern during and following maximal exercise. J Appl
Physiol 1984; 57: 1773–1782.
42 Wanger J, Clausen JL, Coates A, Pedersen OF.
Standardisation of the measurement of lung volumes.
Eur Respir J 2005; (In press).
43 Brusasco V, Pellegrino R, Rodarte JR. Vital capacities
during acute and chronic bronchoconstriction: dependence
on flow and volume histories. Eur Respir J 1997; 10:
1316–1320.
44 Hansen LM, Pedersen OF, Lyager S, Naerra N.
[Differences in vital capacity due to the methods
employed]. Ugerkr Laeger 1983; 145: 2752–2756.
45 Miller MR, Atkins P, Pedersen OF. Inadequate peak
expiratory flow meter characteristics detected by a
computerised explosive decompression device. Thorax
2003; 58: 411–416.
46 Quanjer PH, Lebowitz MD, Gregg I, Miller MR,
Pedersen OF. Peak expiratory flow: conclusions and
recommendations of the European Respiratory Society.
Eur Respir J 1997; 10: Suppl. 24, 2s–8s.
47 Miller MR, Lloyd J, Bright P. Recording flow in the first
second of a maximal forced expiratory manoeuvre: influ-
ence of frequency content. Eur Respir J 2002; 19: 530–533.
48 Pedersen OF, Rasmussen TR, Omland Ø, Sigsgaard T,
Quanjer PH, Miller MR. Peak expiratory flow and the
resistance of the mini-Wright peak flow meter. Eur Respir J
1996; 9: 828–833.
49 Pedersen OF, Pedersen TF, Miller MR. Gas compression in
lungs decreases peak expiratory flow depending on
resistance of peak flow meter. J Appl Physiol 1997; 83:
1517–1521.
50 Kano S, Burton DL, Lanteri CJ, Sly PD. Determination of
peak expiratory flow. Eur Respir J 1993; 6: 1347–1352.
51 Ferris BG Jr, Speizer FE, Bishop Y, et al. Spirometry for an
epidemiologic study: deriving optimum summary statis-
tics for each subject. Bull Eur Physiopathol Respir 1978; 14:
145–166.
52 Federal Register, 38:4265, Feb. 12, 1973, Section of
pulmonary function specifications. Washington, DC,
United States Government Printing Office.
53 Bernstein L. The effect of the rate of breathing on
maximum breathing capacity determined with a new
spirometer. Thorax 1952; 7: 255–262.
54 Miller WF, Johnson RL Jr, Wu N. Relationships between
maximal breathing capacity and timed expiratory capa-
cities. J Appl Physiol 1959; 14: 510–516.
55 Hankinson JL, Viola JO. Dynamic BTPS correction factors
for spirometric data. J Appl Physiol 1983; 44: 1354–1360.
56 Hankinson JL, Castellan RM, Kinsley KB, Keimig DG.
Effects of spirometer temperature on FEV
1 shift changes.
J Occup Med 1986; 28: 1222–1225.
57 Pincock AC, Miller MR. The effect of temperature on
recording spirograms. Am Rev Respir Dis 1983; 128: 894–
898.
58 Hankinson JL, Viola JO, Petsonk EL, Ebeling TR. BTPS
correction for ceramic flow sensors. Chest 1994; 105:
1481–1486.
59 Miller MR, Pincock AC. Linearity and temperature control
of the Fleisch pneumotachograph. J Appl Physiol 1986; 60:
710–715.
60 Perks WH, Sopwith T, Brown D, Jones CH, Green M.
Effects of temperature on Vitalograph spirometer readings.
Thorax 1983; 38: 592–594.
61 Cole P. Recordings of respiratory air temperature. J
Laryngol 1954; 68: 295–307.
62 Madan I, Bright P, Miller MR. Expired air temperature at
the mouth during a maximal forced expiratory manoeuvre.
Eur Respir J 1993; 6: 1556–1562.
M.R. MILLER ET AL. STANDARDISATION OF SPIROMETRY
c
EUROPEAN RESPIRATORY JOURNAL VOLUME 26 NUMBER 2 337
63 Liese W, Warwick WJ, Cumming G. Water vapour
pressure in expired air. Respiration 1974; 31: 252–261.
64 Johnson LR, Enright PL, Voelker HT, Tashkin DP. Volume
spirometers need automated internal temperature sensors.
Am J Respir Crit Care Med 1994; 150: 1575–1580.
65 Hankinson JL, Gardner RM. Standard waveforms for
spirometer testing. Am Rev Respir Dis 1982; 126: 362–364.
66 Nelson SB, Gardner RM, Crapo RO, Jensen RL.
Performance evaluation of contemporary spirometers.
Chest 1990; 97: 288–297.
67 Gardner RM, Hankinson JL, West BJ. Evaluating commer-
cially available spirometers. Am Rev Respir Dis 1986; 134:
626–627.
68 Hankinson JL, Reynolds JS, Das MK, Viola JO. Method to
produce American Thoracic Society flow–time waveforms
using a mechanical pump. Eur Respir J 1997; 10: 690–694.
69 Miller MR, Jones B, Xu Y, Pedersen OF, Quanjer PH. Peak
expiratory flow profiles delivered by pump systems:
limitations due to wave action. Am J Respir Crit Care Med
2000; 162: 1887–1896.
70 Peslin R, Jardin P, Bohadana A, Hannhart B. Contenu
harmonique du signal de de
´
bit pendant l’expiration force
´
e
chez l’homme normal [Harmonic content of the flow signal
during forced expiration in normal man]. Bull Eur
Physiopath Respir 1982; 18: 491–500.
71 McCall CB, Hyatt RE, Noble FW, Fry DL. Harmonic
content of certain respiratory flow phenomena of normal
individuals. J Appl Physiol 1957; 10: 215–218.
72 Miller MR, Pedersen OF, Quanjer PH. The rise and dwell
time for peak expiratory flow in patients with and without
airflow limitation. Am J Respir Crit Care Med 1998; 158:
23–27.
STANDARDISATION OF SPIROMETRY M.R. MILLER ET AL.
338
VOLUME 26 NUMBER 2 EUROPEAN RESPIRATORY JOURNAL
